Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
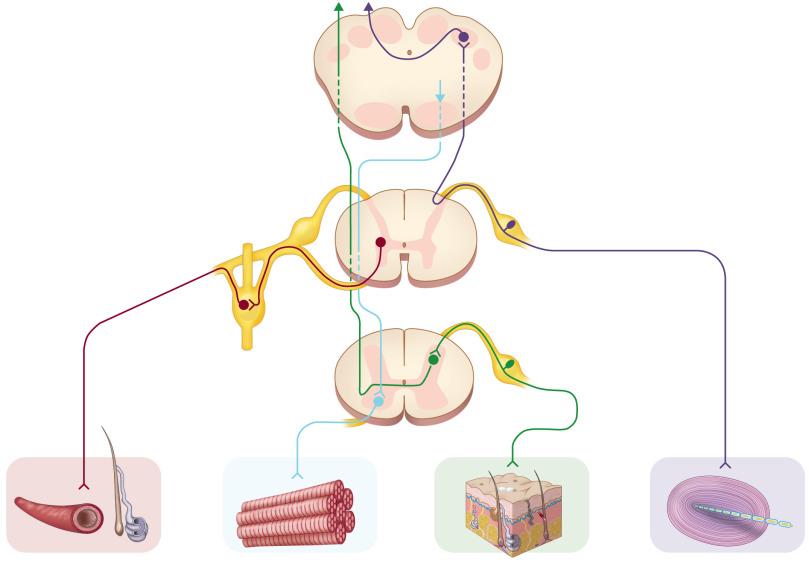
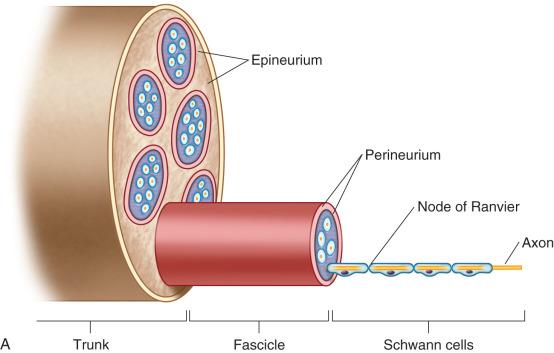
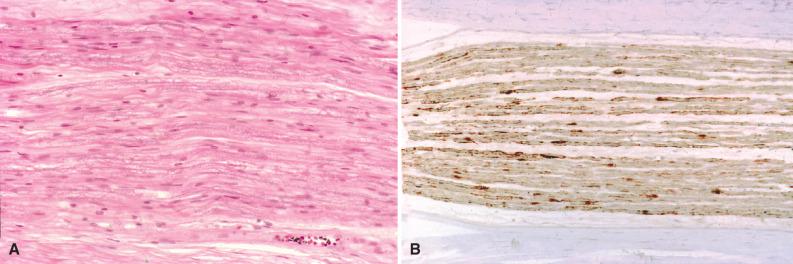
Peripheral nerves consist of nerve sheaths and their invested axons lying both within and outside the craniospinal dura. The axons arise from centrally or peripherally situated neurons ( Fig. 15.1 ). Of all nerve sheath cells, Schwann cells are most important to this chapter given their prominent role in the formation of peripheral nerve tumors. Anatomically, they lie in closest proximity to axons. Beginning at the point where oligodendrocytes cease lining axonal processes emanating from the brain or spinal cord, Schwann cells line up to form a continuous periaxonal coat. Like oligodendrocytes, Schwann cells form myelin. The cross-sectional anatomy of peripheral nerve is illustrated in Fig. 15.2A–D . Longitudinal sections are less informative ( Fig. 15.3A ). Peripheral nerve fibers, or axons, lie within the endoneurium, which provides the microenvironment necessary for nerve conduction, and are arranged in parallel fashion within fascicles. Perineurial cells, the only other intrinsic cells of peripheral nerve and a critical component of the blood-nerve barrier, form the perineurium, which surrounds individual fascicles and separates the intrafascicular endoneurium from the extrafascicular epineurium, each representing soft tissue and consisting of fibroblasts, collagen fibers, and small blood vessels. As for the immunophenotype of nerve, Schwann cells are strongly immunoreactive for S-100 protein ( Fig. 15.3B ) and SOX10, and stain inconsistently for Leu-7 (CD57) and glial fibrillary acidic protein (GFAP). Perineurial cells are nonreactive for all four markers but are immunoreactive for epithelial membrane antigen (EMA), GLUT1, a glucose transporter, and claudin-1, a protein associated with tight junctions. Axons are neurofilament protein positive ( Fig. 15.3C ). Variations in myelin thickness are a reflection of axon size, with large fibers featuring thicker Luxol fast-blue (LFB) positive sheaths ( Fig. 15.3D ).
The peripheral nerve tumors discussed herein either arise from identifiable peripheral nerves or show differentiation toward nerve sheath cells.
Termed traumatic or amputation neuroma, this non-neoplastic proliferation results from significant nerve injury leaving it in continuity (“neuroma in continuity”) or completely transected. It consists of all essential nerve elements (axons, Schwann cells, and perineurial cells) typically arranged as disordered tangles or microfascicles set within a fibrous stroma. Traumatic neuroma is the most common reparative proliferation affecting nerves. In that all nerve components are represented, the lesion is a so-called “true neuroma.”
Reinnervation of the distal stump of a transected nerve requires an influx of axons and Schwann cells after the distal segment has been vacated of its cellular debris (axons and myelin sheaths). This process, termed Wallerian degeneration, is seen in as little as 24 hours after transection ( Fig. 15.4 ). On a Luxol fast-blue/periodic acid–Schiff (LFB-PAS) stain, the color of macrophage granules varies from blue in an early phase (intact myelin) to red with progression (PAS-positive degraded myelin). At approximately 1 month, most axonal and myelin debris has been removed. Cords and tubes of basement membrane–enshrouded Schwann cells termed “bands of Büngner” await the ingrowth of new axons.
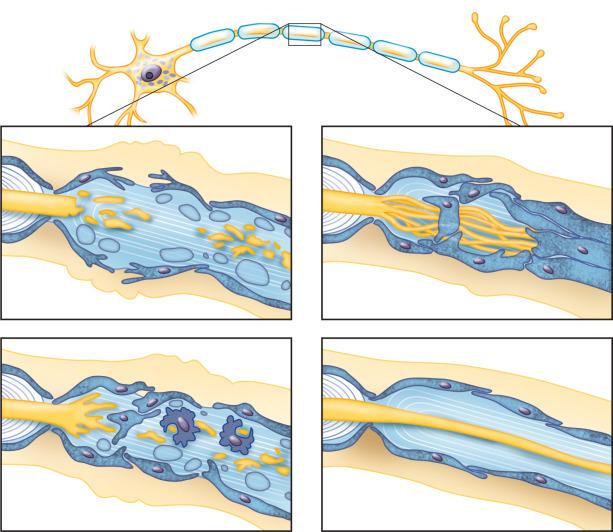
Between 1 and 3 months after nerve injury, the stumps of proximal axons become expanded and organelle rich. Neurites emerge from the expansion under the influence of nerve growth factor, elaborated by Schwann cells and trophic factors of macrophage origin. Growing 1 to 2 mm a day, the new axons cross the gap, reach the distal nerve segment, and colonize the band of Büngner. If misdirection of the process occurs, connections cannot be firmly established, and the new axons atrophy.
Traumatic neuromas are essentially aborted attempts at regeneration in which the distal stump is too far removed to establish continuity or is blocked by tissue destruction and inflammatory reaction.
Traumatic neuromas are often tender or painful nodules. Either neuromas in continuity or ones occurring after complete transection (“stump neuromas”) represent common postoperative sequelae. Some, particularly neuromas in continuity, arise after seemingly insignificant injury. Traumatic neuromas also occur at visceral sites, such as the region of the gallbladder and bile ducts; most present months to years after cholecystectomy or in association with lithiasis.
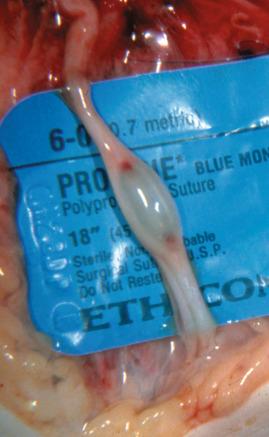
On imaging studies, traumatic neuromas show no specific features, but on CT most include a centrally radiolucent nodule with a peripherally dense rim. Traumatic neuromas are grossly firm, circumscribed, gray-white nodules situated at the proximal stump of transected or incompletely transected nerves ( Fig. 15.5 ). At sites such as the brachial plexus, severe postganglionic injury may result in multiple traumatic neuromas, either in continuity or at rupture(s) of the nerve. Nearly all traumatic neuromas measure less than 5 cm, although occasional brachial plexus examples may approach 10 cm.
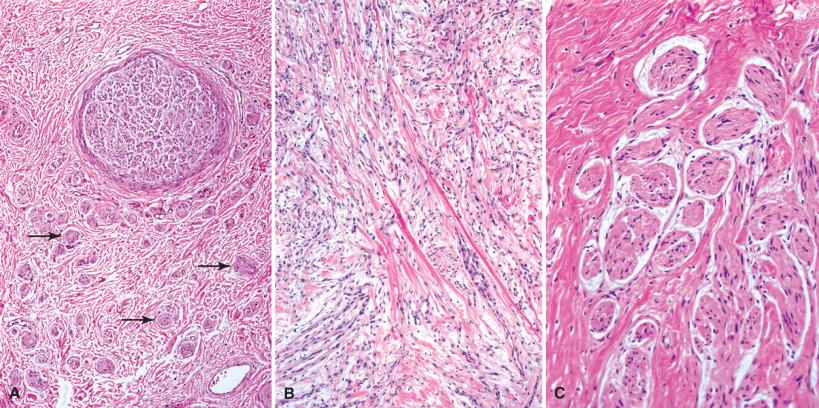
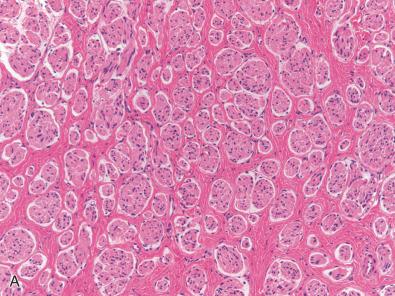
Traumatic neuromas consist of haphazard tangles of nerve fibers —that is, regenerated axons accompanied by ensheathing Schwann cells ( Figs. 15.6 and 15.7 ). The fibers are far less heavily myelinated than those of the parent nerve. When axons are grouped, they form small bundles (microfascicles) ( Figs. 15.6C and 15.7 ). In cross section, the latter are surrounded by perineurium ( Fig. 15.7B ). The stroma surrounding microfascicles often contains a mucoid matrix, but in well-established lesions, it is fibrocollagenous. Extension of microfascicles into adipose tissue may be seen. Chronic inflammation and even residual trauma-related foreign body reaction may be evident.
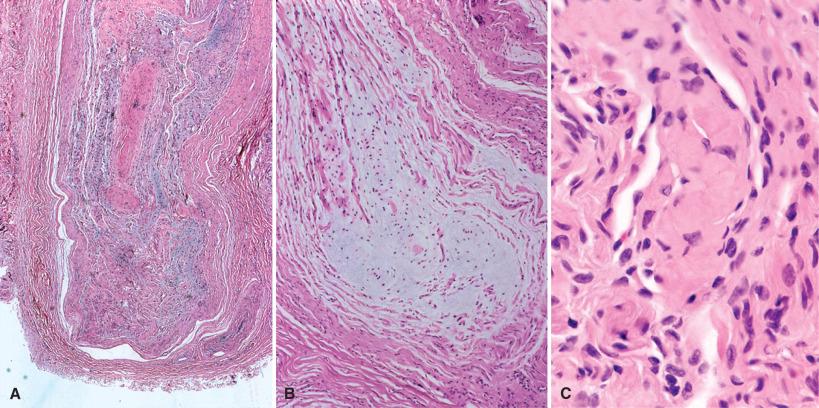
Principal lesions include other “true neuromas,” specifically localized interdigital neuritis (Morton neuroma), palisaded encapsulated neuroma, and mucosal neuromatosis, as well as neoplasms such as plexiform examples of schwannoma and neurofibroma. Morton (interdigital) neuroma is closely related to the traumatic neuroma. Its characteristic involvement of interdigital nerves of the foot is distinctive. Unlike traumatic neuromas, which usually result from transection and feature proliferative changes with the formation of microfascicles, Morton neuroma is a fusiform enlargement or thickening of the intact but chronically compressed nerve. Attachment to bursa or surrounding soft tissue is often seen. Microscopically, it shows primarily degenerative changes affecting all nerve layers including endoneurium, perineurium, and epineurium ( Fig. 15.8 ). Nerve fiber loss is significant as is endoneurial edema, perineurial fibrosis and elastosis, and vascular hyalinization.
Pacinian neuromas, which in actuality represent hypertrophy of pacinian corpuscles, often occur in the digits following trauma. Most are greater than 1.5 mm. Their structure consists of single or clustered corpuscles attached to nerve by a stalk or grouped in a subepineurial location ( Fig. 15.9A ). Fibrosis is common ( Fig. 15.9B ). Their lamellae are EMA positive and one, two, or even no nerve fibers may be seen at their centers.
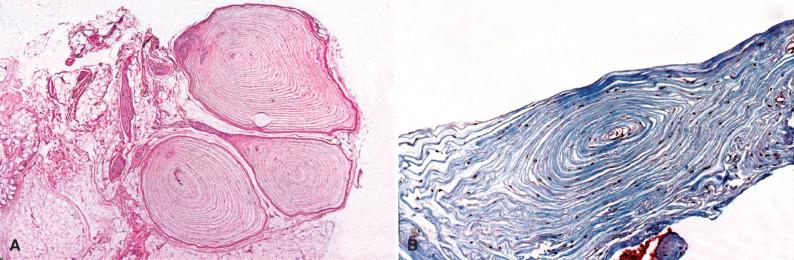
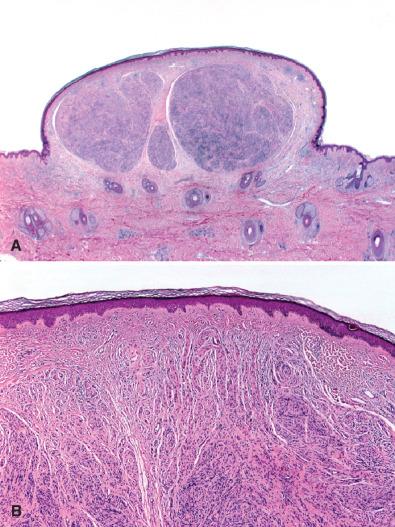
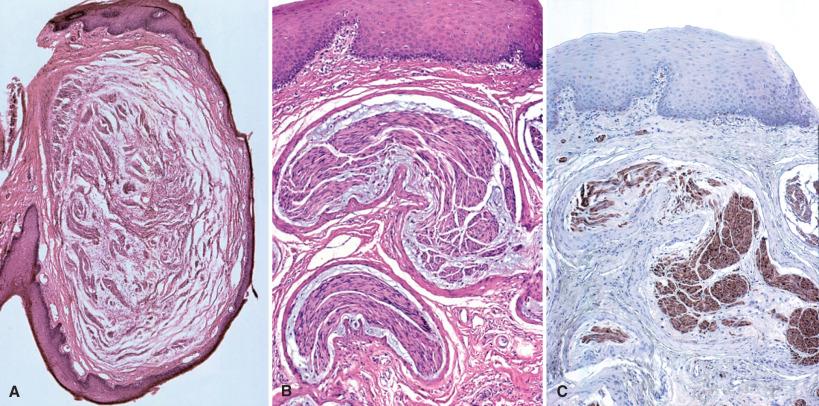
Palisaded encapsulated neuromas (PENs) are also true neuromas. There is a slight female predilection. Most involve skin and occasionally superficial subcutaneous tissue of the face rather than deeper soft tissue. No definite NF or MEN-IIb association is seen, although hybrid PEN-like and mucosal neuromas have recently been described in the latter. Whether uninodular or multinodular ( Fig. 15.10A ), the bulk of the lesion consists of Schwann cells and a variable numbers of axons, often vertically oriented with respect to the skin surface ( Fig. 15.11 ). The involved nerve is seen only at the microscopic level, at the base of the lesion. Scant perineurium is seen at the periphery of the lesion but not at its apex where the proliferation appears to splay ( Fig. 15.10B ). Well-formed microfascicles are lacking.
Mucosal neuromas typically, but not invariably, occur in the setting of multiple endocrine neoplasia (MEN) type IIb (bilateral pheochromocytoma, C cell hyperplasia, medullary thyroid carcinoma, parathyroid hyperplasia), wherein they may be an early feature. Sites most affected include the lip, mouth, eyelids, and viscera (intestine, urinary bladder), with lesions formed by irregular, tortuous nerve bundles having prominent perineurium and variable myxoid change ( Fig. 15.12 ). In viscera, both submucosal and myenteric plexus is involved, replete with an increase in ganglion cells. Solitary mucosal neuromas occurring in the biliary system and appendix can closely resemble traumatic neuroma and may be trauma related.
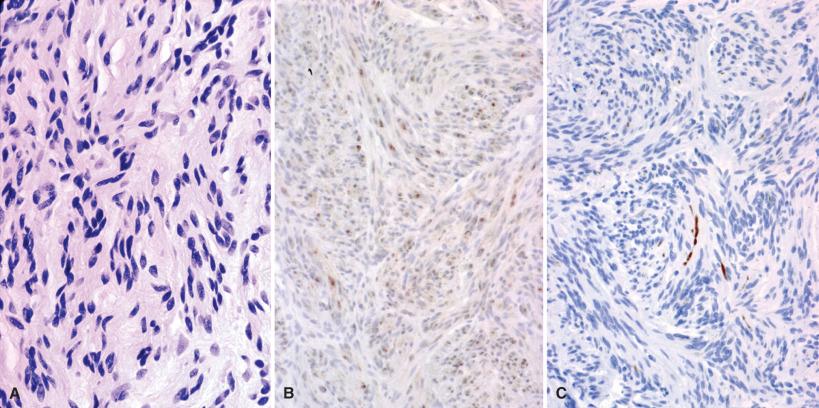
The constituents of traumatic neuromas show the expected immunoreactivities, with axons being reactive for neurofilament protein; Schwann cells for S-100 protein, SOX10, and Leu-7; and perineurial cells for EMA, glut-1, and claudin-1. In early phases of nerve regeneration, axons are unmyelinated and simply surrounded by Schwann cell cytoplasm. With time, some degree of myelin wrapping takes place and nerve fibers become surrounded by perineurial cells to form microfascicles.
Awareness of neuroanatomy in the operative field may prevent the occurrence of traumatic neuromas. Once they occur, optimal treatment is controversial. Any attempt at surgical repair or reconstruction will, by definition, result in a new neuroma, although symptom reduction is the treatment goal. Different strategies have been employed. Excision of the traumatic neuroma, followed by embedding of the proximal stump into normal nerve tissue away from a joint, is often effective. Nerve reconstruction by direct repair or grafting may also be performed. These treatment approaches still may not remedy the problem. Lastly, removal of traumatic neuromas may also be necessary when, in the setting of prior cancer surgery, it is necessary to exclude recurrent neoplasm.
Schwannomas are among the most common of peripheral nerve neoplasms. Based on differing clinical, gross, and histologic features, three major forms are recognized : conventional schwannoma, cellular schwannoma, and plexiform schwannoma. Rare variants include epithelioid schwannoma and microcystic/reticular schwannoma, with the latter showing a predilection for visceral locations. The first three variants are mainly globular tumors displacing and compressing the remainder of the parent nerve. Nerve fibers are sometimes found in subcapsular and deeper areas of the tumor.
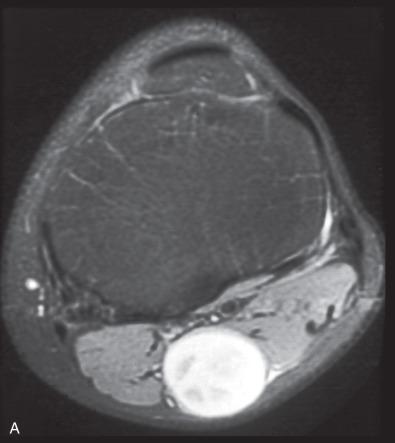
As with other nerve sheath tumors, the neuroimaging features of schwannomas are relatively nonspecific. Nonetheless, the origin of the tumor from a nerve is often demonstrable, particularly if it is carefully sought, and its finding often suggests a nerve sheath tumor rather than another soft tissue neoplasm. On MR images, they are usually contrast enhancing with isointense signal relative to skeletal muscle on T1-weighted and increased signal intensity on T2-weighted images ( Fig. 15.13A ). With respect to the spinal cord, schwannomas are typically intradural extramedullary masses, often forming dumbbell-shaped tumors with a narrowing where they traverse the spinal foramen. Sacral examples may be massive (“giant sacral schwannoma”) ( Fig. 15.13B ). Intracranially, involvement and expansion of the internal auditory meatus creates an “ice cream cone” pattern with the tapering growth within the meatus representing the “cone” and the unimpeded growth of the intracranial component representing the “scoop of ice cream” ( Fig. 15.13C ); this appearance greatly favors schwannoma over other cerebellopontine tumors, such as meningioma. In contrast, the presence of a dural tail favors meningioma. The radiologic finding of bilateral vestibular schwannomas is pathognomonic for type 2 neurofibromatosis (NF2; see Chapter 22 ). Other cranial nerves, such as the trigeminal and facial nerves, are also occasionally the source of schwannomas, but much less frequently than the vestibular nerve. Clinicopathologic features of schwannomas are further discussed in the next section according to histologic subtype.
This most common form of schwannoma generally presents in adults with a peak incidence between the third and sixth decades, there being no gender prevalence.
Sites commonly affected include the head and neck, flexor surfaces of the extremities, and spinal as well as cranial nerves, most often of sensory type. Visceral tumors are rare. The same is true of osseous examples. Schwannomas are generally solitary, but multiple schwannomas occur in two disorders: NF2 and schwannomatosis (see Chapter 22 ). Multiple schwannomas affecting primarily the eighth cranial (vestibular branch) nerves bilaterally are pathognomonic of NF2.
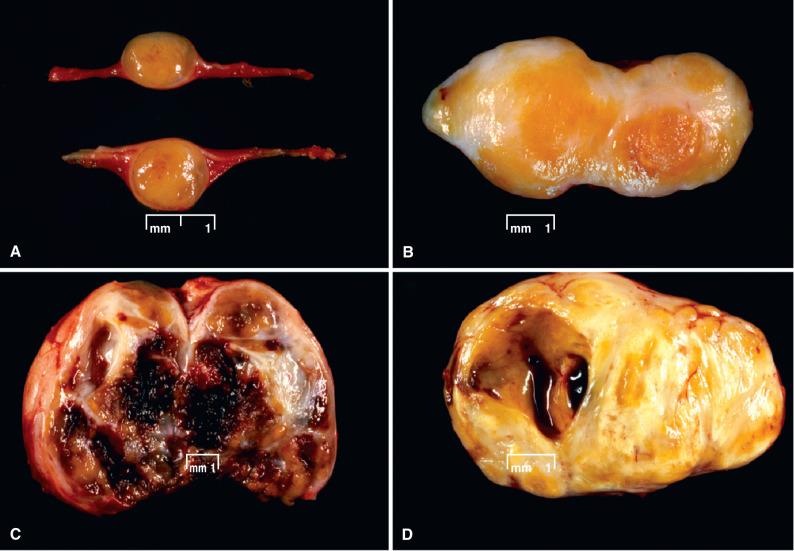
In most cases, gross inspection of a schwannoma provides important clues to the diagnosis. In addition to their generally globular shape, the tumors are truly encapsulated and an associated parent nerve is often apparent. The cut surface reveals a subcapsular zone of smooth, slightly dull, homogeneously light tan and firm tissue. This is readily evident in the majority of schwannomas, as are bright yellow areas (aggregates of lipid-laden histiocytes; Fig. 15.14A and B ), hemorrhagic foci, and cystic change ( Fig. 15.14C and D ). Necrosis may be seen, particularly in large examples.
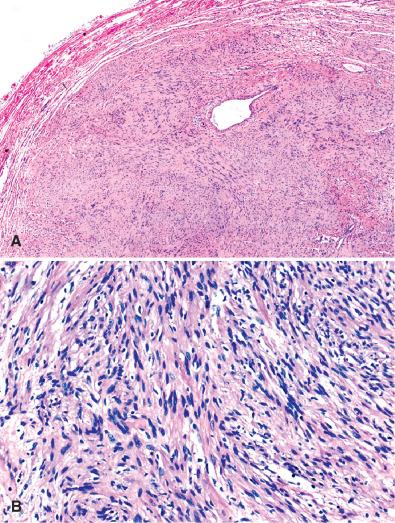
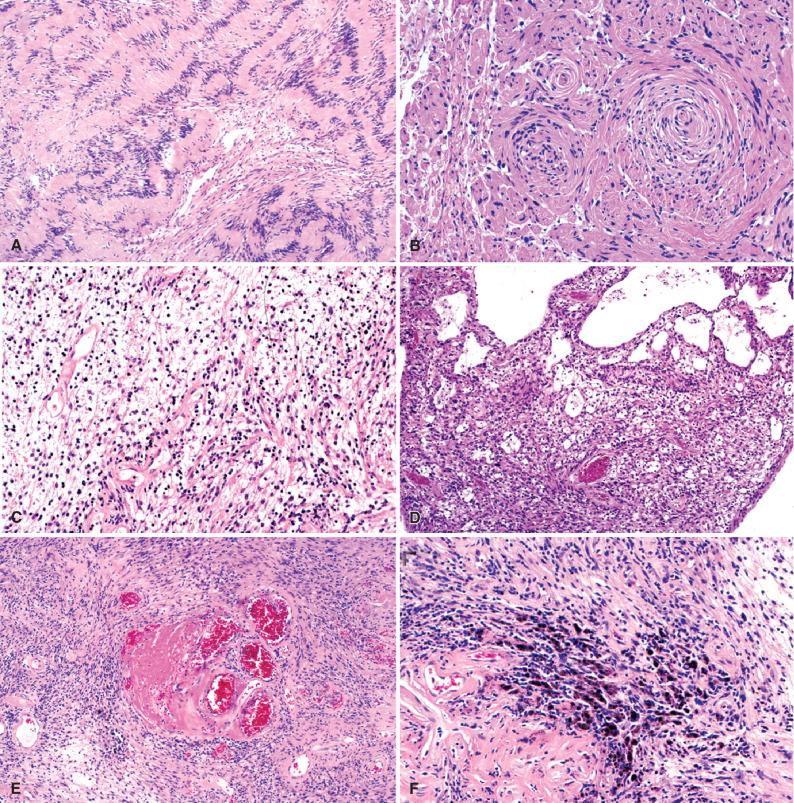
As a rule, schwannomas begin within single nerve fascicles ( Fig. 15.15 ). Histologic findings in conventional schwannomas include fibrous encapsulation of a largely spindle cell tumor ( Fig. 15.16 ). The compact regions comprise the so-called Antoni A component ( Fig. 15.16A ). Tumor cells and their processes are occasionally arranged in a manner that gives rise to palisaded nuclei ( Verocay bodies; Fig. 15.17A ) or whorls ( Fig. 15.17B ), and a loose-textured (Antoni B) element featuring round nuclei and loose-knit cell processes ( Fig. 15.17C ). This tissue is prone to undergo microcystic change ( Fig. 15.17D ). Thick-walled, hyalinized blood vessels ( Fig. 15.17E ) associated with hemosiderin deposits ( Fig. 15.17F ), as well as collections of foamy histiocytes, are also most frequent in Antoni B tissue. Only occasional schwannomas show myxoid change. Entrapped intratumoral axons are few, often subcapsular, and seen only on special stains. Degenerative atypia in the form of large, hyperchromatic nuclei with smudgy chromatin and lack of nucleoli may be seen ( Fig. 15.18A ), but mitotic figures are lacking or infrequent. Necrosis may also be seen ( Fig. 15.18B ).

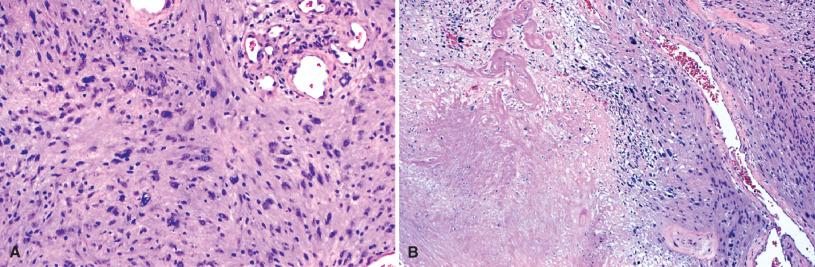
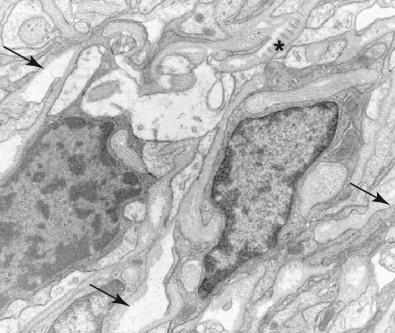
All schwannomas are strongly, uniformly S-100 protein immunoreactive ( Fig. 15.19A ). SOX10 staining is also common ( Fig. 15.19B ) as is collagen IV reactivity ( Fig. 15.19C ). A minority also show patchy GFAP staining. Neurofilament protein-positive axons are scant ( Fig. 15.19D ). The capsule of schwannomas consists of EMA-reactive perineurial cells. Ultrastructurally, the tumor cells show features of well-differentiated Schwann cells, including continuous basal lamina and the formation of long-spacing collagen (“Luse bodies”) ( Fig. 15.20 ).
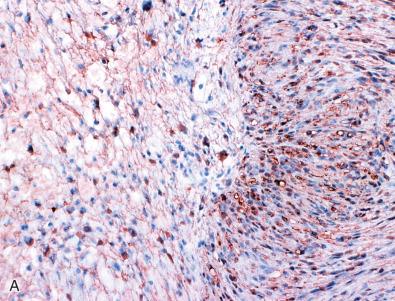
The clinicopathologic distinction of schwannoma from neurofibroma is important. Schwannomas are occasionally NF2 or schwannomatosis associated, globular, eccentric to the remainder of the nerve, encapsulated, variably lipidized (and thus yellow), feature Antoni A and B patterns as well as Verocay bodies, show little or no stromal mucin, contain few mast cells, and rarely undergo malignant change. In contrast, neurofibromas are often NF1 associated and fusiform with respect to the parent nerve; are variably mucoid; show occasional Meissnerian corpuscles or onion bulb–like structures; consist of a wider mix of cells with features of Schwann, perineurial, and intermediate cells; commonly show mast cells; and, when affecting large, deep nerves, have a low but significant capacity for malignant transformation. At the gross level, confusion may also arise with hypervascular tumors, such as hemangioma and paraganglioma. A helpful diagnostic gross feature is the presence of homogeneously light tan, firm tissue. Histologically, the closest mimics of conventional schwannoma are palisaded leiomyoma, palisaded myofibroblastoma of inguinal lymph nodes (PMILN), and gastrointestinal stromal tumor (GIST). Palisaded leiomyoma usually presents in müllerian tissues and is immunoreactive for smooth muscle actin as well as desmin. In contrast to schwannoma, GIST is usually immunoreactive for KIT (CD117) and DOG1.
Conventional schwannomas are benign tumors that can be cured by complete resection. When incompletely excised, they occasionally recur and become clinically symptomatic. Recurrences are more frequent in so-called “giant sacral schwannomas,” which are often subtotally resected, as well as in the setting of NF2. Effective surgical treatment of schwannomas needs to include within the resection specimen, the entering and exiting nerve fascicle, which can often be separated from the parent nerve. This permits preservation of neurologic function, even when tumors are large. There is no compelling evidence that schwannomas undergo accelerated growth during pregnancy, and as such, surgery can typically be delayed until after delivery. The exceptionally rare occurrence of malignant transformation in conventional schwannoma is discussed later in the chapter.
This is a variant of schwannoma with a female predominance and a site predilection for the posterior mediastinum and pelvis. Craniospinal and cutaneous nerves may also be affected. About 4% occur in the setting of NF1. Cellular schwannomas are benign and should neither be considered a MPNST precursor nor mistaken for MPNST.
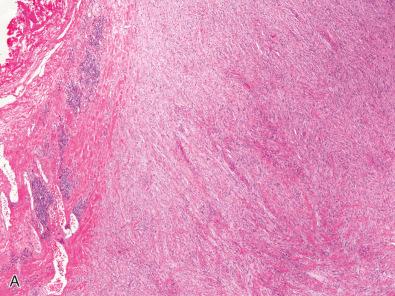
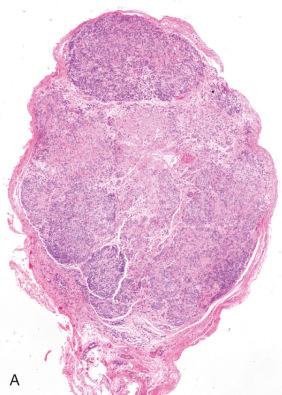
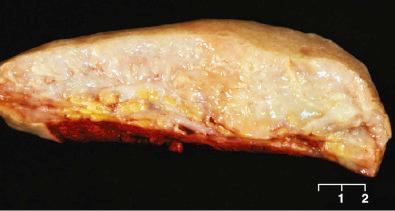
Grossly, cellular schwannomas are ovoid but more solid than the conventional variant, usually having a relatively uniform, firm, tan cut surface ( Fig. 15.21 ) with only occasional white and yellow patches. If hemorrhage is present, it is usually focal, perhaps related to prior biopsy. Furthermore, there is usually no gross evidence of necrosis. Some examples are plexiform/multinodular (discussion to come). Bone erosion may be seen, especially in paraspinal cases.
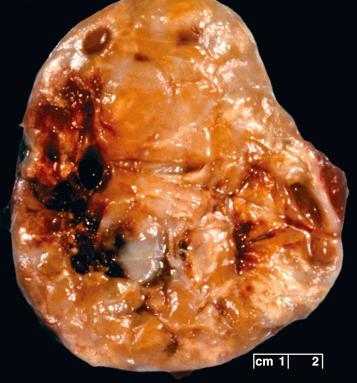
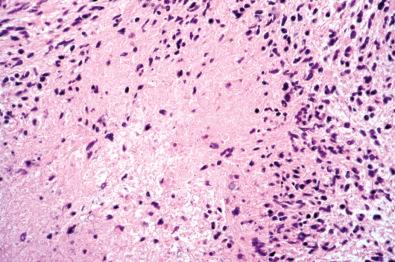
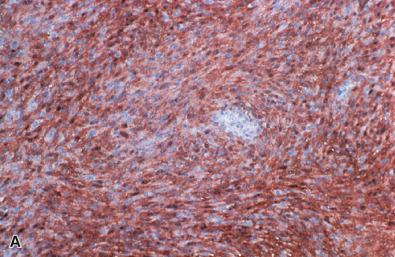
Like conventional schwannoma, cellular schwannomas are encapsulated ( Fig. 15.22A ) and exhibit vascular hyalinization ( Fig. 15.22B ), but are composed predominantly or exclusively of Antoni A type tissue without well-formed Verocay bodies. They consist mostly of spindle cells closely arrayed in fascicles ( Fig. 15.22C ), a storiform arrangement, or in a nonspecific pattern. Cellular whorls are a notable but inconstant finding. Lymphoid aggregates are often seen in or beneath the capsule ( Fig. 15.22D ) as are intratumoral collections of lipid-laden histiocytes. The spindle cells possess eosinophilic cytoplasm. Nuclei generally show minor pleomorphism and hyperchromasia. Mitoses usually are easily found ( Fig. 15.22C ). Microfoci of necrosis may be seen but are typically nonpalisading in nature ( Fig. 15.23 ). Intratumoral nerve fibers, quite dispersed due to tumor volume, are few and generally subcapsular. The immunohistochemical ( Fig. 15.24 ) and ultrastructural features are those of a well-differentiated schwannoma.
Much has been written about the differential diagnosis of cellular schwannoma. In brief, the two tumors with which it is most often confused are (1) benign and low-grade malignant smooth muscle tumors, and (2) malignant peripheral nerve sheath tumor (MPNST). Although there are subtle cytologic differences between cellular schwannomas and smooth muscle tumors, a few simple observations aid in this distinction. Smooth muscle tumors are typically unencapsulated, whereas cellular schwannomas feature a capsule and are invariably strongly and diffusely reactive for S-100 protein, but immunonegative for muscle markers.
Far more troubling for pathologists are the histologic similarities of cellular schwannoma to MPNST. Cellular schwannomas are usually globular, encapsulated tumors whereas MPNSTs are fusiform or globoid in configuration and are pseudo-encapsulated, the latter consisting of infiltrated surrounding tissue. Antoni A tissue predominates in cellular schwannoma by definition, the cells being arranged in fascicles or whorls; hyperchromasia and nuclear pleomorphism are generally mild. Hyalinized blood vessels and subcapsular lymphoid deposits are also common features. In contrast, MPNSTs are composed of spindle cells showing greater hyperchromasia and nuclear atypia. Whereas cellular schwannomas show only microscopic foci of necrosis, MPNSTs often show grossly obvious necrosis, which is often palisading in type. Schwannomas typically feature relatively low mitotic counts (<4 per 10 HPF), whereas MPNSTs far exceed that number. Cellular schwannomas are composed of a uniform cell population of Schwann cells, but MPNSTs may feature considerable cytologic variation. Cellular schwannomas are diffusely positive for S-100 protein and SOX10; podoplanin (D2-40) expression is also a feature. In contrast, MPNSTs show only minor reactivity for Schwann cell markers. S-100 protein is the most frequently expressed marker, but even with the inclusion of multiple other Schwann cell markers, only 50% to 65% of MPNSTs show some degree of labeling. Recently described features that favor the diagnosis of MPNST over cellular schwannoma include neurofibromin and H3K27 trimethylation loss. Lastly, cellular schwannomas may show significant bone erosion but do not metastasize. Instead, MPNSTs destroy surrounding soft tissue, permeate bone, and frequently metastasize. Surprising clinical and operative associations include: (a) the rare occurrence of cellular schwannoma in a patient with NF1, and (b) the even rarer finding of concurrent and separate cellular schwannoma and MPNST.
Cellular schwannomas are benign but capable of recurrence when incompletely excised. This is particularly true of proximal tumors involving the spinal nerves extending into the spinal canal, sacral tumors, and intracranial examples. In such instances, fully 30% to 40% recur. There have been no reports of a cellular schwannoma metastasizing.
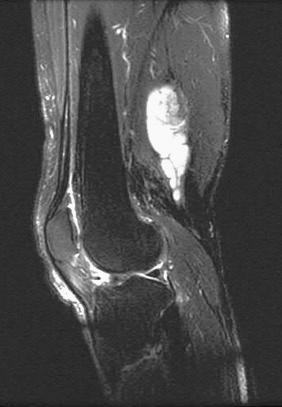
Roughly 5% of all schwannomas are multinodular or plexiform and of either conventional or cellular subtype. In a large study, head and neck (23%) and skin (15%) were found to be most often affected. Deep-seated examples are uncommon, favor females, tend to be syndrome unassociated, and often show their plexiform nodular feature radiographically ( Fig. 15.25 ). Prior to its recognition two decades ago, examples were regarded as plexiform neurofibromas or as MPNSTs arising in the same. A frequent feature, most notably in cutaneous examples, is lack of encapsulation. The same is not true of large soft tissue examples. Although there is no association with NF1, superficially situated tumors occur in NF2 and in schwannomatosis, each accounting for approximately 5% of all cases.
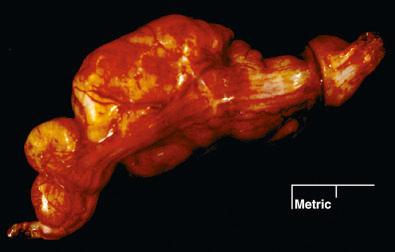
Plexiform schwannomas vary in size. Their plexiform multinodular nature may not be grossly evident in small cutaneous tumors, but is obvious in sizable, soft tissue lesions ( Fig. 15.26 ). Only occasionally do they show the entwining “worms” appearance of plexiform neurofibroma. The same is true of rare visceral examples. As in conventional schwannomas, patchy yellow discoloration may be seen on the cut surface of larger tumors.
Microscopic sections show contorted profiles of affected tumor consisting of compact, elongate neoplastic Schwann cells, more Antoni A than B in pattern ( Fig. 15.27A ). Epithelioid cytology is rarely encountered. Occasional mitoses may be seen. Hyalinized blood vessels are usually limited to larger examples. As a rule, lymphoid aggregates and clusters of lipid-laden histiocytes are absent. The tumor is uniformly S-100 protein positive ( Fig. 15.27B ) and shows pericellular collagen IV staining. In small tumors, entrapped axons are few or absent on neurofilament protein stain but are more readily seen in larger examples. The fascicles of affected nerves are surrounded by residual EMA-immunoreactive perineurium.
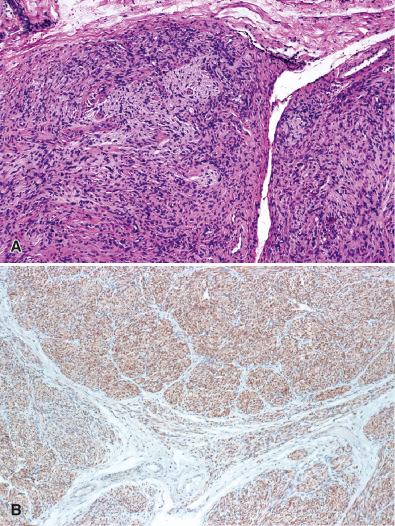
Some cellular childhood examples of this tumor may mimic MPNST, but should not be considered malignant. Although such tumors may recur locally, both their immunohistochemistry and lack of metastatic potential argue in favor of their status as cellular schwannoma subtypes. Emphasis has been placed on the presence of four or more mitoses/10 HPF in many cases, but some studies have not found mitotic activity to be prognostically important when evaluating plexiform or cellular schwannomas. Local recurrence is a problem that may be attributed to failure to achieve a total resection, due either to lack of encapsulation or to irregular tumor contours in the form of finger-like protrusions.
Plexiform schwannomas must also be distinguished from plexiform neurofibromas, palisaded encapsulated neuroma (PEN), and neurotropic melanoma. Plexiform neurofibromas are far less cellular, contain more mucinous matrix, and show fewer S-100 protein staining cells. In contrast to plexiform schwannoma, PENs contain more numerous axons as seen on neurofilament protein immunostain and often demonstrate a nerve twig entering on their deep aspect. Like most plexiform schwannomas, neurotropic melanomas occur in the skin and subcutaneous tissue. Given profound differences in prognosis, it is of utmost importance to distinguish the two. Neurotropic melanoma favors the head and neck and is often associated with an overlying lentigo-type in situ melanoma. Both tumors involve nerves, but plexiform schwannomas form a mass pushing the distorted, remnant parent nerve to one side, such that residual normal nerve is often difficult to identify. In contrast, in neurotropic melanoma, nerve fibers are often readily identified. Neurotropic melanomas primarily occupy the epineurium and encase as well as invade the perineurium to form distinctive, concentric rings surrounding intact endoneurium. Additionally, neurotropic melanomas have nuclei that are larger, more irregular in shape, and more often markedly hyperchromatic. Lastly, neurotropic melanoma is commonly associated with prominent desmoplasia, whereas plexiform schwannoma is not. Although S-100 protein immunoreactivity is seen, staining for HMB-45 is often lacking in desmoplastic melanoma.
Plexiform schwannomas must be interpreted as benign neoplasms. As mentioned, however, a small proportion of incompletely excised tumors do recur.
Both neurofibromas and schwannomas may show epithelioid features. Epithelioid schwannomas are uncommon and may be histologically uniform ( Fig. 15.28 ). Most are subcutaneous and behave in a benign fashion, even when atypical features (i.e., increased mitotic activity) are present. Immunohistochemical features are those of conventional schwannomas.
Of conventional, cellular, and plexiform schwannomas, only the first two, on very rare occasion, have been found to undergo malignant transformation. When it occurs, the malignant Schwann cells are cytologically high grade and often epithelioid in appearance. Rarer still is transformation to a small cell, neuroepithelial tumor. The malignant epithelioid cells possess abundant eosinophilic cytoplasm, vesicular nuclei, and prominent nucleoli. Also of note are rare schwannomas containing clusters of atypical epithelioid cells with nuclear hyperchromasia and small nucleoli. Such cells are thought by some to represent “premalignancy” or early epithelioid malignant change (EMC). When an MPNST arises in a patient with NF2 or schwannomatosis, the possibility of a schwannoma with EMC should be considered.
In addition to the malignant transformation noted, angiosarcoma may also develop in conventional schwannomas, and most show epithelioid cytology. The sarcoma cells typically show CD31, CD34, ERG, or other vascular marker immunoreactivity, but not for S-100 protein. Sarcomatous differentiation of the Schwann cell component of a schwannoma is extremely rare and may take the form of rhabdomyosarcoma.
The term melanotic schwannoma is likely a misnomer, and most now consider this tumor to be a unique diagnostic entity, rather than merely a histologic variant of schwannoma. This very uncommon, clinicopathologically and genetically unique tumor has a predilection for posterior spinal nerves and their ganglia. Autonomic nerves may also be affected. Its peak incidence is in the fourth decade, and in contrast to schwannomas a subset of these tumors metastasize. In a recent study of 40 cases, local recurrences and metastases developed in 35% and 44% of cases, respectively. The authors therefore proposed the designation of malignant melanotic schwannian tumors, given the substantial number of cases with more aggressive biology, in contrast to schwannoma.
Melanotic schwannomas are usually solitary and ovoid, but a multifocal nodular presentation may be seen, in which case the tumor is often malignant. The tumors generally are covered entirely or in large part by a thin fibrous membrane; their cut surface varies from gray to pitch black and often has the feel of dried tar ( Fig. 15.29 ). Nearby bone may be eroded, but intraosseous examples are quite rare.

Most melanotic schwannomas are characterized by plump spindle and epithelioid cells ( Fig. 15.30 ). Nonetheless, considerable histologic variation may be seen. The cells are disposed in lobules, nests, sheets, and/or somewhat fascicular arrangements ( Fig. 15.30A and B ), and have indistinct cell borders, thus yielding a syncytial appearance. Melanin pigmentation is variable as is cytoplasmic volume ( Fig. 15.30A–C ). Nuclei are round to ovoid with delicate chromatin and small nucleoli. Melanocytic markers such as HMB-45, Melan-A (MART-1), and tyrosinase are positive. Ultrastructural studies show variably pigmented melanosomes. Coarse chromatin and prominent, “violaceous” nucleoli in association with numerous mitoses and necrosis are suggestive of malignancy. Melanotic schwannomas arising from paraspinal ganglia may contain residual ganglion cells.
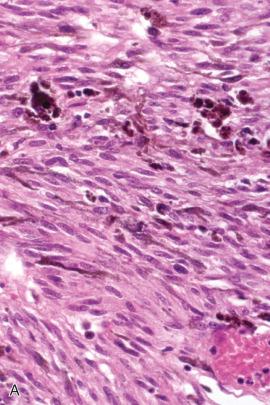
About 45% of the melanotic schwannomas contain psammoma bodies ( Fig. 15.31A ); termed “ psammomatous melanotic schwannomas (PMS),” such tumors often also feature lipoma-like fat accumulation ( Fig. 15.31B ). This variant of melanotic schwannoma is more often associated with Carney complex, although the reported frequency of the association is highly variable (see also Chapter 22 ). The mean age of complex-affected patients is 22 years, a full decade younger than for those with non-syndromic melanotic schwannomas. Components of the disorder include lentiginous pigmentation; blue nevi; myxomas of heart, skin, or breast; congenital osteochondromyxoma; and endocrine overactivity (variably due to pigmented nodular adrenocortical hyperplasia producing Cushing syndrome, large cell Sertoli cell tumors of testis associated with sexual precocity, or pituitary adenoma, typically acromegaly associated). A complex tumor with myoid, neuroendocrine, and perineurial features has also been described in this setting.
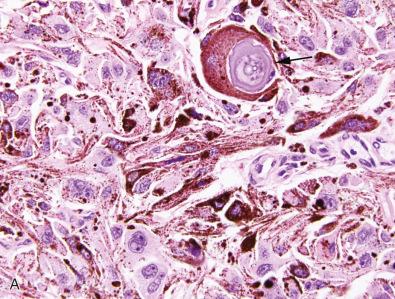
Half of Carney complex patients have mutations of the PRKAR1A tumor suppressor gene, located on 17q 22-24 and encoding for the type 1 alpha regulatory subunit of cAMP-dependent protein kinase A (PKA). Loss of heterozygosity for this gene locus has been found in associated tumors. Loss of expression of the PRKAR1A protein, the Carney complex–associated tumor suppressor gene product, has been observed in melanotic schwannoma and is not limited to Carney complex–associated neoplasms ( Fig. 15.32A ).
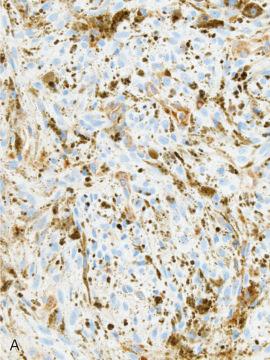
The differential diagnosis of melanotic schwannoma includes malignant melanoma (both primary meningeal and metastatic) and meningeal melanocytoma, all of which express melanocytic markers including SOX10 ( Fig. 15.32B ). In contrast to melanoma, the cells of melanotic schwannoma are often disposed in lobules or clusters, some collagen IV delineated ( Fig. 15.32C ), and generally bland with only slight cytologic atypia and often syncytial cytology of cells. Melanomas do not feature psammoma bodies or adipose-like cells. The same is true of melanocytomas, which originate from leptomeninges, often feature whorling, lack atypia, but may exhibit perilobular basal lamina formation. Additionally, primary leptomeningeal melanomas follow a similar genetic progression as that of blue nevi–associated melanomas and uveal melanomas, more commonly displaying GNAQ or GNA11 mutations, often followed by loss of BAP1 expression.
Since their clinical and pathologic associations differ significantly, recognizing neurofibromas and distinguishing them from schwannomas are important. In contrast to schwannomas, neurofibromas are often NF1 associated and undergo malignant transformation far more frequently.
The term neurofibroma is applied to a spectrum of benign peripheral nerve sheath tumors including localized or diffuse cutaneous lesions, intraneural lesions of localized or plexiform type, and a massive soft tissue variant. All consist of a mixture of Schwann cells, perineurial-like cells, fibroblasts, and cells with intermediate features.
Many neurofibromas, particularly intraneural and plexiform, are associated with a recognizable nerve, as evidenced by the finding of residual axons within the tumor, either myelinated or unmyelinated. Genetic studies showing deletion of the NF1 gene, specifically in the Schwann cell element, mouse models, and the well-known tendency of some neurofibromas to transform into MPNST all support their neoplastic nature. Relative to tumorigenesis, all NF1 patients have one nonfunctional NF1 gene as the result of a germline mutation. Neurofibromas in these patients are apparently initiated by a second, somatic mutation. Neurofibromas unassociated with NF1 occur instead as a result of two somatic mutations in the NF1 gene. Atypical neurofibromas may additionally show CDKN2A inactivation with loss of p16 expression. MPNSTs that arise in transformation from neurofibromas contain additional genetic mutations involving other tumor suppressor genes and oncogenes (see later discussion).
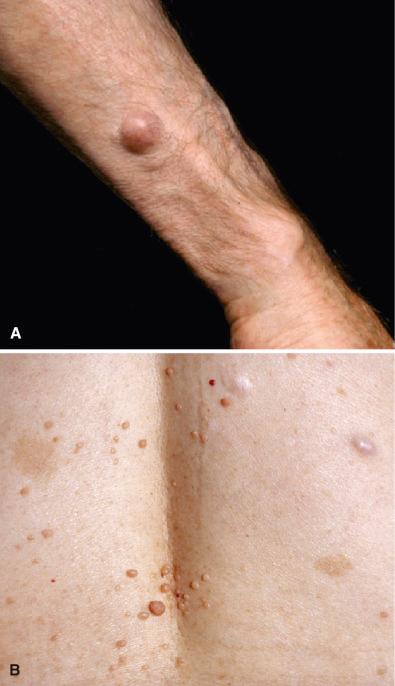
The majority of neurofibromas occur sporadically as individual lesions ( Fig. 15.33A ). However, the finding of multiple neurofibromas is one of the principal features of NF1 ( Fig. 15.33B ). Rare examples are said to arise in NF2, although this issue is still debated.
As in schwannomas, the radiologic features of neurofibromas are not specific. The differential diagnosis is often lengthy, including both benign and malignant processes in some cases. Nevertheless, the association with a nerve and the overall growth pattern can be extremely helpful, typically reflecting the gross pathology described in each histologic variant discussed in the following section. The classic constellation of a sizable plexiform and/or multiple paraspinal intraneural tumors is virtually pathognomonic for NF1 (see also Chapter 22 ). Monitoring these multiple and often large tumors for early signs of malignant transformation is challenging. Some have demonstrated the value of PET studies in detecting early malignant transformation.
Although they share a common cellular makeup, several clinicopathologic variants of neurofibroma have been described. Their clinical characteristics, gross appearance, and even microscopic features vary considerably. Therefore, they are discussed separately, as follows, and include cutaneous neurofibromas of both localized and diffuse subtypes, intraneural neurofibromas of localized and plexiform subtypes, and massive soft tissue tumors often composed of both diffuse and plexiform elements. In addition, neurofibromas of viscera commonly feature one or both of these patterns. Although the clinicopathologic characteristics of these various lesions differ considerably, morphologic overlap is often seen. Their gross appearance, however, is a reflection of their patterns of growth and spread. For example, cutaneous lesions either form localized polypoid nodules or diffusely infiltrate dermal and subcutaneous tissues. In contrast, intraneural neurofibromas originate in sizable nerves and undergo endoneurial spread with resultant fusiform enlargement of fascicles. Tumor involvement of multiple fascicles of the affected nerve is the key feature of plexiform neurofibromas. When affected nerves branch, the result is a “bag of worms” appearance. Plexiform tumors are also often accompanied by an element of diffuse soft tissue infiltration. Massive soft tissue neurofibromas often feature a minor plexiform component as well. In addition to multiple cutaneous neurofibromas, plexiform and massive soft tissue tumors are also manifestations of NF1. Each is discussed now.
In contrast to intraneural neurofibromas occurring at deep sites, cutaneous neurofibromas are mainly extraneural proliferations. Nonetheless, they no doubt originate from small nerves residing in dermal and/or subcutaneous tissue.
Localized cutaneous neurofibromas elevate the skin as soft, hemispheric to pedunculated lesions having no particular distribution. Painless, freely movable, and ranging in size up to 2 cm, the vast majority of the localized type are solitary and sporadic, occurring in 20- to 30-year-old patients (see Fig. 15.33A ). On the other hand, when multiple, they are a key feature of NF1, becoming particularly evident at puberty ( Fig. 15.33B ). In later life, NF1-associated tumors may be innumerable.
In contrast to localized lesions, diffuse cutaneous neurofibromas are uncommon. Plaque-like, they form cutaneous and often subcutaneous lesions, frequently in the head and neck region of children or young adults ( Fig. 15.34 ). An association with NF1 is seen in only about 10%.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here