Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
An estimated 108 million Americans over the age of 18 years have hypertension (HTN).
HTN is the most common cardiovascular condition observed in competitive athletes.
Athletes are usually considered to be free from cardiovascular disease because of their apparent high level of fitness.
The overall incidence of HTN in athletes is approximately 50% less than that in the general population.
HTN begins in young adulthood; incidence increases with age
Almost 80% of adolescents with an elevated blood pressure (BP) (>142/92 mmHg) during preparticipation physical examinations have HTN.
Normal BP: Systolic <120 mmHg and diastolic <80 mmHg
Elevated BP: Systolic 120–129 mmHg and diastolic <80 mmHg
HTN:
Stage 1: Systolic 130–139 mmHg or diastolic 80–89 mmHg
Stage 2: Systolic ≥140 mmHg or diastolic ≥90 mmHg
If there is a disparity in category between systolic and diastolic pressures, the higher value determines stage ( Table 36.1 )
| Systolic (mmHg) | Diastolic (mmHg) | |
|---|---|---|
| Normal | <120 | <80 |
| Elevated blood pressure | 120–129 | <80 |
| Hypertension | ||
| Hypertension: Stage 1 | 130–139 | 80–89 |
| Hypertension: Stage 2 | ≥140 | ≥90 |
Stage 1: systolic 130–139 mmHg or diastolic 80–89 mmHg
Associated with increased cardiac output (CO), which primarily increases systolic BP, along with “normal” vascular total peripheral resistance (TPR)
TPR is normal compared with resting levels in normotensives but inappropriately high when CO is elevated.
In nonhypertensive patient, TPR falls to compensate for rise in CO, thereby maintaining normal BP.
Lack of decrease in TPR is result of impaired baroreceptor function.
Baroreceptors are “reset” to maintain elevated rather than normal BP over time.
People with stage 1 HTN are hypersensitive to catecholamine secretion and mental stress and have a hyperkinetic circulatory state.
Stage 2:
Systolic BP 140–159 mmHg and diastolic BP 90–99 mmHg
Increased heart rate (HR) and CO and decreased TPR
Decreased arterial lumen and disturbed autoregulation of peripheral blood flow
Systolic BP >160 mmHg and diastolic BP >100 mmHg
Normal HR and CO; increased TPR
Increased afterload leads to left ventricular hypertrophy (LVH) and increased diastolic BP. Severe and/or uncontrolled HTN may lead to development of diastolic dysfunction and congestive heart failure (CHF).
CO can no longer increase in response to exercise or other physiologic demands.
Loss of contractility and CHF may develop.
Most active individuals with HTN will fall into stage 1 or lower stage 2 (<160 mmHg/<100 mmHg).
Those with comorbidities, such as diabetes or renal disease, should be treated at stage 1 levels.
Values for pediatric athletes under age 13 are adjusted for age, gender, and height ( Table 36.2 ).
| For Children Aged 1 to <13 Years | For Children Aged ≥13 Years | |
|---|---|---|
| Normal BP | Systolic and diastolic BP <90th percentile | Systolic BP <120 and diastolic BP <80 mmHg |
| Elevated BP | Systolic and diastolic BP ≥90th percentile to <95th percentile or 120/80 mmHg to <95th percentile (whichever is lower) | Systolic BP 120–129 and diastolic BP <80 mmHg |
| Stage 1 HTN | Systolic and diastolic BP ≥95th percentile to <95th percentile + 12 mmHg or 130/80—139/89 mmHg (whichever is lower) | 130/80–139/89 mmHg |
| Stage 2 HTN | Systolic and diastolic BP ≥95th percentile + 12 mmHg or ≥140/90 mmHg (whichever is lower) | ≥140/90 mmHg |
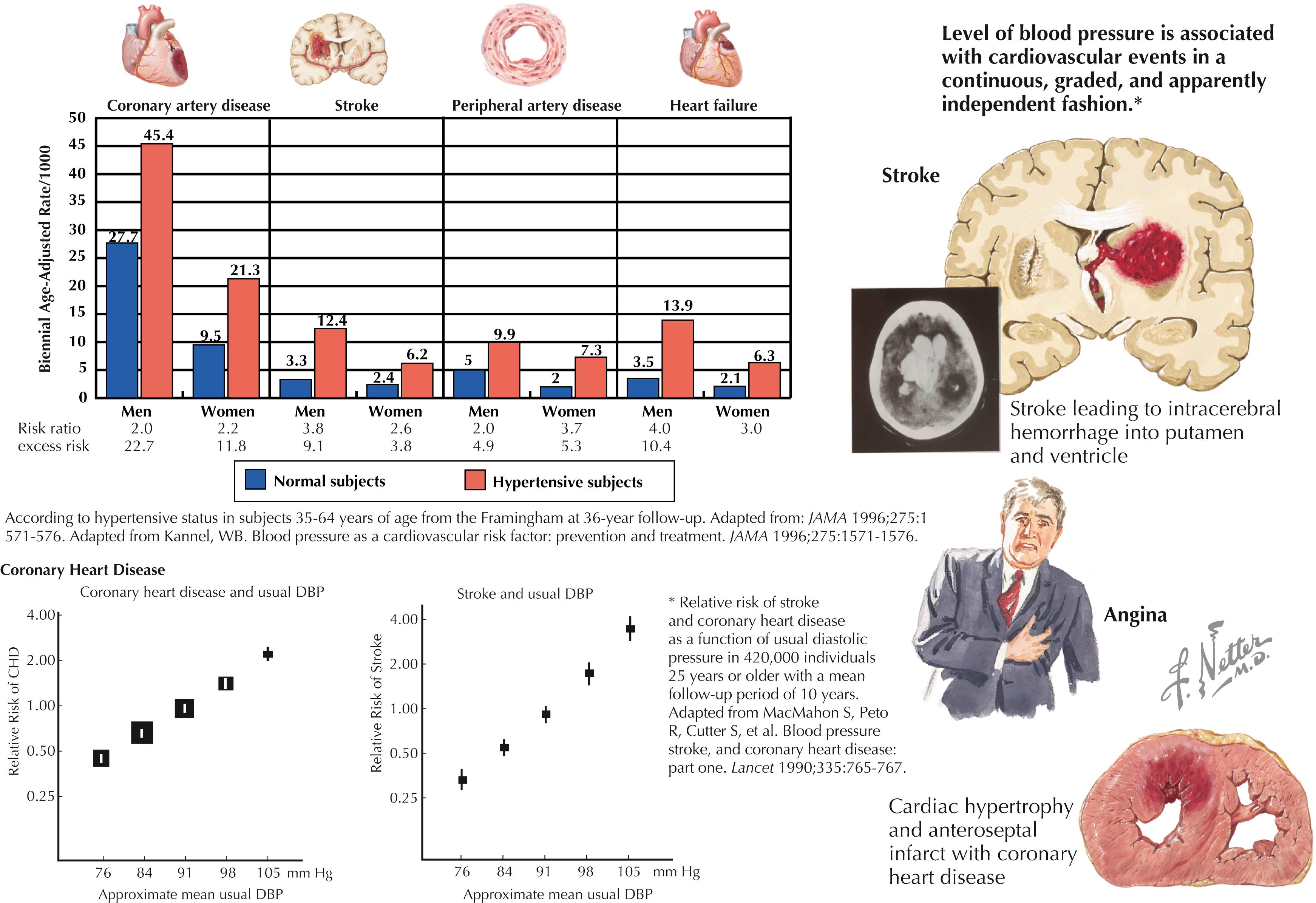
Higher stages are associated with a higher risk of nonfatal and fatal cardiovascular disease in addition to progressive renal disease ( Fig. 36.1 ).
Ninety-five percent of cases
Abnormal neuroreflexes and sympathetic control of peripheral resistance
Abnormal renal and metabolic control of vascular volume and compliance
Abnormal local smooth muscle and endothelial control of vascular resistance
Sustained increases in systemic vascular resistance (SVR)
Five percent of cases
Younger patients or adults with rapid onset of HTN and no prior history of HTN
BP is often poorly responsive to routine therapy.
Renal (most common)
Renovascular disease
Increased renin stimulates conversion of angiotensin I to angiotensin II, which is a vasoconstrictor, in addition to release of aldosterone
Renal retention of sodium and water
Fibromuscular dysplasia in younger patients and atherosclerosis in older patients
Renal parenchymal disease
Inability of damaged kidneys to excrete sodium and water
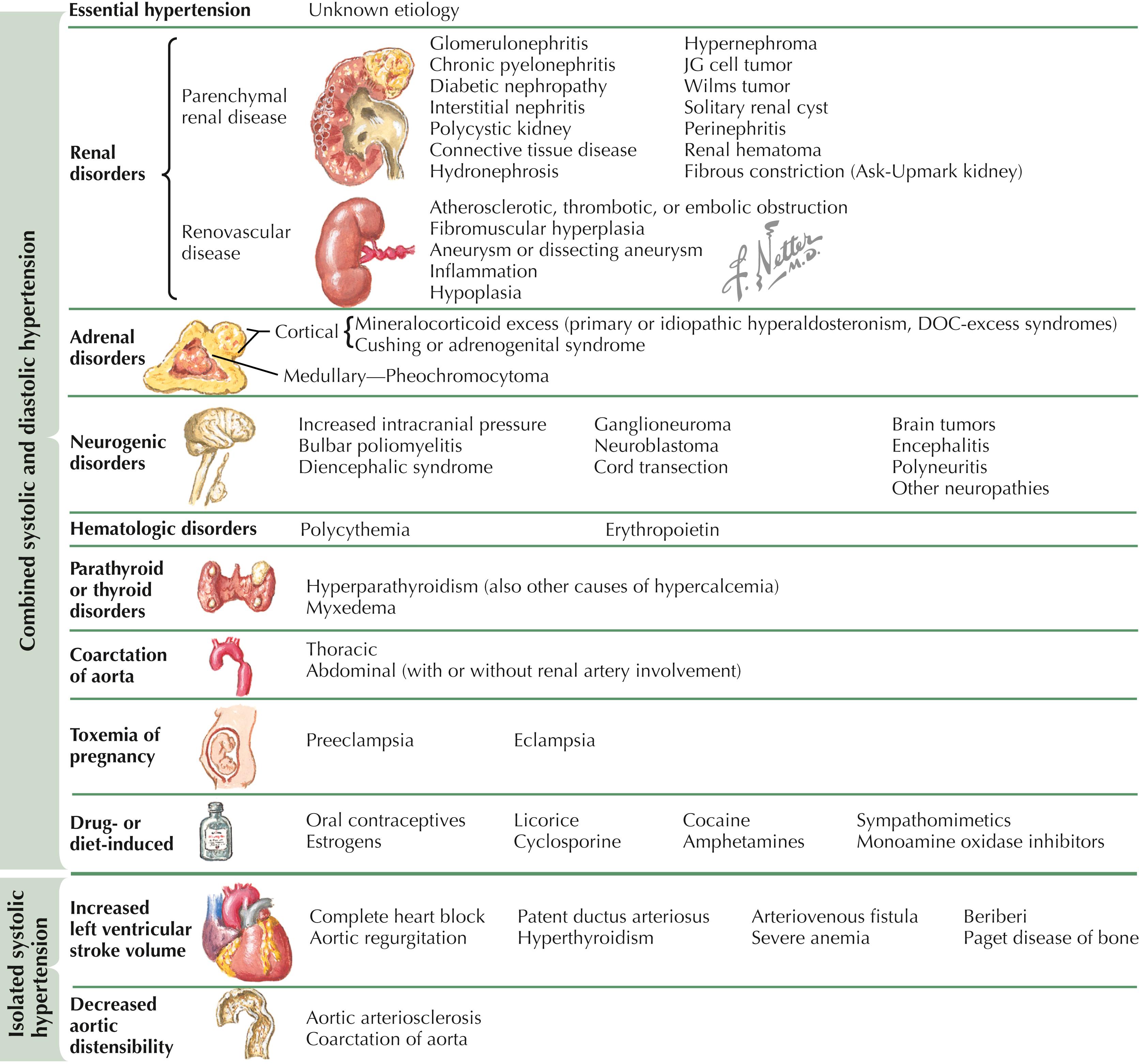
Endocrine
Adrenal
Pheochromocytoma
Cushing syndrome
Primary aldosteronism
Thyroid
Hyperthyroidism
Hypothyroidism
Acromegaly
Hyperparathyroidism
Other
Coarctation of the aorta
Obstructive sleep apnea
Age
Five to ten percent in adults aged 20–30 years
Twenty to thirty-five percent in middle-aged adults
More than 50% in adults aged over 60 years
Residual lifetime risk of 90%
Genetic factors
Males more than females
African Americans more than Caucasians (2:1); Asians lowest risk
Family history (HTN twice as common if either parent has HTN)
Metabolic factors
Obesity
Glucose intolerance
Endocrine disorders (see “Causes”)
Stress
Environmental
Social
Leads to chronic neurogenic activation of the sympathetic nervous system
Behavioral factors
High sodium intake
Excessive alcohol consumption
Drug abuse (see later)
Medications
Oral contraceptive pills (OCPs); 5% will develop HTN over 5 years
Nonsteroidal anti-inflammatory drugs (NSAIDs), particularly chronic use
Antidepressants, including tricyclic antidepressants, selective serotonin reuptake inhibitors, and monoamine oxidase inhibitors
Corticosteroids, including both glucocorticoids and mineralocorticoids
Decongestants, such as phenylephrine and pseudoephedrine
Some weight-loss medications
Attention-deficit/hyperactivity disorder (ADHD) medications such as methylphenidate and amphetamines
Illicit drug use
Recreational: cocaine, methamphetamines or tobacco (chew)
Ergogenic: stimulants, erythropoietin, human growth hormone, or anabolic steroids
Diagnosis of HTN can be confirmed by serial (at least three) office-based BP measurements with a mean of ≥130/≥80 mmHg spaced over a period of weeks to months (see Table 36.1 ).
Should be confirmed with home BP monitoring or ambulatory blood pressure monitoring (ABPM) if possible.
In children and early adolescents, HTN is defined as average systolic or diastolic BP ≥95th percentile for age, gender, and height, measured on three separate occasions. Adolescents over age 13 use the same measurements as adults (see Table 36.2 ).
Measurement of BP should be performed in a standard measurement situation, preferably a quiet area.
Avoid exercise and caffeine for >30 minutes before measurement.
Let the athlete sit in a chair with back supported and feet flat on the floor for a few minutes if possible.
Choose the appropriate-size BP cuff. Many athletes will need a large cuff, and a thigh cuff should be available for very large athletes.
BP cuff’s inflatable bag should cover approximately 80% of arm’s circumference.
BP may be overestimated if the BP cuff is too small, whereas BP may be underestimated if the BP cuff is too big.
Avoid rapid deflation of the cuff.
Repeat BP measurements if elevated.
In younger athletes, if BP in arm is elevated, obtain BP measurement in leg to assess for aortic coarctation.
Anxiety provoked by medical examination or other sources of mental stress can lead to artificially elevated BP, known as “white coat” HTN.
Average of several readings is a better estimate of true BP.
If initial BP is high, have athlete rest for 5 minutes and repeat BP measurement.
If BP remains elevated, check BP at least once per week for at least two additional visits.
Averaged daily BP is a better predictor of later end-organ damage than random office BP.
Twenty-four-hour ABPM may more accurately assess BP in people with variable readings in the office or at home but can be difficult and expensive.
Home BP monitoring correlates well with ABPM.
Athletes/exercisers can take their own BP, but must be well trained in measurement of BP.
Emphasize importance of accurate readings.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here