Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
This chapter includes an accompanying lecture presentation that has been prepared by the authors: ![]() .
.
MRI is the primary imaging modality for brain tumor detection and characterization.
CT is a useful imaging modality to evaluate bone involvement of extra-axial tumors.
Advanced MRI techniques can help differentiate between tumor types and help noninvasively determine prognosis and tumor grade.
Advanced positron emission tomography (PET) techniques may also have utility in noninvasively grading brain tumors and determining prognosis.
Functional MRI (fMRI) can localize motor and speech centers relative to tumor.
The noninvasive localization and characterization of brain tumors with CT and MRI can facilitate treatment planning. Imaging also plays important roles in determining extent of resection following surgery, as well as monitoring treatment response after chemotherapy or radiation therapy. This chapter presents a general approach for evaluating brain tumors, with emphasis on how current imaging techniques can inform patient management in various clinical settings. The radiologic features of commonly encountered brain tumors relevant to diagnostic, prognostic, and therapeutic implications are also presented.
Preoperative diagnoses of brain tumors should be based on both clinical and radiologic features to increase the accuracy in distinguishing among various tumor types as well as nontumor mimics. The patient age and sex, the presenting symptoms and signs, and the underlying medical conditions often give important initial clues to diagnosis; they can provide demographic and temporal information that improves diagnostic accuracy beyond that based on imaging findings alone.
The decision regarding which imaging modalities are used during initial work-up of patients with suspected brain tumor now largely depends on the availability of scanners. Because of the similarity in radiographic density between brain tumors and normal brain, small brain tumors may not be detectable by CT unless there is either significant surrounding edema or distorting mass effect. MRI provides optimal characterization of intracranial tumors in almost all cases but is not readily available in all locations. Contrast-enhanced MRI allows detection of very small parenchymal or meningeal lesions—1 to 2 mm. Use of advanced contrast-enhanced techniques, such as magnetic resonance perfusion (MRP) and magnetic resonance angiography (MRA), can provide functional data that help characterize the differences between pathologic and normal tissues. Finally, advanced MRI techniques such as blood oxygen level–dependent (BOLD) imaging and diffusion tensor imaging (DTI), the basis of functional brain activation and tractography studies, respectively, are widely used in presurgical planning.
CT has advantages over MRI for visualization of bone-centered lesions and in the acute emergency setting. CT imaging of the bony matrix can demonstrate patterns that can help identify the underlying pathology. For example, benign lesions often grow slowly and can be accompanied by bone remodeling that is evident as smooth cortical margins. The presence of soft tissue calcifications, often found in a subset of brain tumors such as oligodendroglioma, meningioma, germ cell neoplasm, and craniopharyngioma, is better demonstrated on CT evaluation. In the emergency setting, CT is the screening test of choice owing to its wider availability and speed, which are particularly important when tumor-related mass effect or other urgent disease conditions, such as hemorrhage and ischemia, are causing acute neurological symptoms or decline. CT may also be the only available option if patients have contraindications for MRI, such as ferromagnetic foreign bodies, implants, and surgical devices that cannot be removed or replaced.
The general imaging approach to patients with brain tumors consists of the following steps: (1) identification of mass effect, (2) localization of tumor within distinct anatomic regions of brain, and (3) analysis of imaging features within and around lesion(s).
Although many brain tumors manifest as rounded, measurable masses at presentation, a number of tumors, particularly intra-axial neoplasms, can have irregular shapes with unclear boundaries. Features of mass effect on imaging include direct expansion of brain, meninges, nerves, or cranium, as well as indirect signs, including sulcal, ventricular, or cisternal effacement, displacement of vessels or cranial nerves, obstructive hydrocephalus, and herniation. More complex evaluation of mass effect is based on evaluation of the degree of mass effect with relation to the size of the lesion.
Determining mass lesions as being in intra-axial (within brain parenchyma) or extra-axial (external to brain parenchyma) locations can greatly facilitate imaging diagnosis as well as surgical planning. Although the majority (>80%) of extra-axial tumors in adults are benign, including meningiomas and schwannomas, the majority of intra-axial tumors are malignant, including metastases and high-grade gliomas that carry a poor prognosis.
Extra-axial masses frequently exhibit the following characteristics:
Displacement or compression of adjacent cortex
Cerebrospinal fluid (CSF) or cortical vessels between mass and brain
Contrast enhancement and thickening of dura, leptomeninges, or cranial nerves
Invasion of adjacent bone
Features supporting intra-axial location are as follows:
Containment of all the margins of the lesions by brain parenchyma
Expansion of the cortex
Although intra-axial and extra-axial tumors can be reliably differentiated in most cases, a small number of tumors may have features of both tumor locations, making determination difficult. Gliosarcoma as well as other sarcomatous tumors can involve both intra-axial and extra-axial compartments.
A number of imaging features are routinely evaluated to help narrow the differential diagnosis of brain tumors. Each feature is discussed individually in this section and summarized in Table 144.1 .
| Location | ||
|---|---|---|
| Imaging Feature(s) | Intra-Axial | Extra-Axial |
| Calcification | Oligodendroglioma, central neurocytoma, metastases (genitourinary or gastrointestinal origins, osteosarcomas, and chondrosarcomas) | Meningioma, craniopharyngioma |
| Cysts | Metastasis, hemangioblastoma, pilocytic astrocytoma, desmoplastic infantile ganglioglioma, dysembryoplastic neuroectodermal tumor, ganglioglioma | Craniopharyngioma, schwannoma, meningioma, epidermoid/dermoid |
| Necrosis | Glioblastoma, metastasis | Metastasis, meningioma |
| High cellularity | Lymphoma, glioblastoma, primitive neuroectodermal tumors, metastasis | Meningioma, lymphoma, metastasis |
| High vascularity | Glioblastoma, hemangioblastoma, metastasis (renal cell carcinoma, choriocarcinoma, and thyroid carcinoma) | Meningioma, Hemangiopericytoma/solitary fibrous tumor |
Vascular permeability can be affected by the presence of tumor, due either to direct breakdown of the blood-brain barrier (BBB) or to indirect effect from tumor-related vasoactive secretions. These physiologic changes are responsible for the qualitative lesion enhancement observed on CT scans or T1-weighted MR images obtained after administration of a contrast agent, as a result of extravascular leakage of the contrast agent. Among intra-axial tumors, most aggressive tumors, including metastases, higher-grade astrocytomas, primitive neuroectodermal tumors (PNETs), and lymphomas, enhance. On the other hand, nonenhancing tumors tend to be observed among low-grade tumors such as low-grade astrocytoma and subependymoma. Also, a number of nonaggressive tumors can enhance, including many extra-axial tumors, such as meningiomas and schwannomas, and some intra-axial tumors, including pilocytic astrocytoma, glioneuronal tumors, and a small subset of low-grade gliomas. Contrast enhancement is not specific to brain tumors; other pathologic processes, including infarct, inflammation, and infection, can also affect the integrity of the BBB and thus cause leakage of contrast material to interstitial space. Finally, many high-grade gliomas demonstrate heterogeneous contrast enhancement, with both enhancing and nonenhancing components, as a manifestation of their genetic heterogeneity. The enhancing component typically correlates with more aggressive, high-grade tumor components that should therefore be targets for biopsy or resection in order to optimize treatment planning and achieve the best outcome.
Increase in interstitial water content is one consequence of greater vascular permeability and can manifest as either decreased attenuation on CT or hyperintense signal on T2-weighted or T2–fluid-attenuated inversion recovery (FLAIR) MRI. Evaluation of the edema pattern surrounding brain lesions can also be very helpful in making a diagnosis, because a vasogenic pattern is most commonly observed in peritumoral edema. This pattern is characterized by edema that does not violate the boundary at the gray matter–white matter junction and is easily discernable by visual inspection, because the difference in image intensity between gray matter and white matter is greater on both CT and MRI. This is in contradistinction to the cytotoxic edema pattern, such as in cases of ischemic infarction, in which gray matter is also affected, causing a reduction in contrast (blurring) at the gray matter–white matter junction. Extra-axial tumors, primarily meningiomas and schwannomas, are less frequently associated with edema in adjacent brain parenchyma. Intratumor hemorrhage can also cause rapid expansion of tumor volume and thereby cause secondary edema from compressive effect. Among intra-axial primary brain tumors, edema is typically absent with low-grade astrocytomas, oligodendrogliomas, gangliogliomas, ependymomas, and hemangioblastomas. Although low-grade gliomas typically lack surrounding edema, these tumor tissues can be difficult to distinguish from edema on conventional MRI sequences because of their similarities in high T2 signal. Furthermore, infiltrative tumor and edema can coexist within the same image pixels, such that it is often difficult to determine whether high T2 signal is due to edema or an infiltrative lesion. Nonetheless, low-grade infiltrative tumors tend to have a more indolent clinical course, with slow change in imaging appearance on serial MRI examinations. Edema associated with higher-grade intra-axial brain tumors often evolves rapidly, causes associated symptoms, and may be modulated by therapeutic interventions including administration of steroids. Intra-axial metastases almost always exhibit peritumoral edema, the extent of which is often significantly greater than the actual tumor size. When untreated brain metastases are observed without associated edema, involvement of extra-axial space (i.e., leptomeninges) must be suspected. Finally, edema that occurs in response to radiation therapy is often indistinguishable from edema induced by tumor.
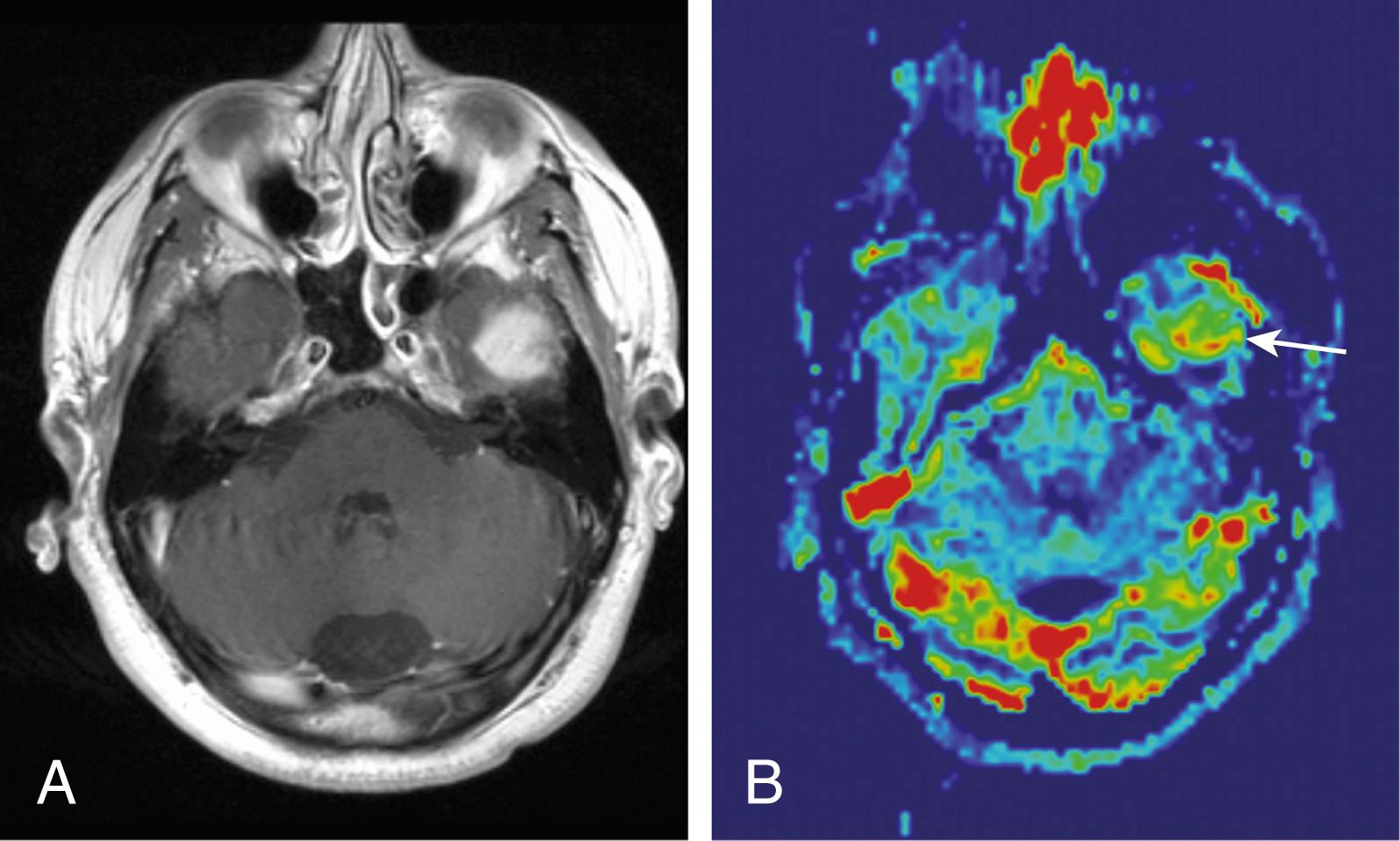
In addition to increases in vascular permeability observed in a number of brain tumors, intravascular blood volume, or tumor vascularity, can be augmented as a result of tumor-induced angiogenesis. This augmentation creates an increase in tissue microvessel density (MVD) within the tumor that corresponds to greater regional cerebral blood volume (rCBV) on the perfusion imaging study. Estimation of intravascular volume in tumors requires use of dynamic imaging methods, such as dynamic contrast-enhanced MRI (DCE-MRI), dynamic susceptibility contrast MRI (DSC-MRI), arterial spin-labeled MRI (ASL-MRI), and dynamic contrast-enhanced CT. Correlation between rCBV and tumor histologic grades has been demonstrated in astrocytic tumors, but there is wide variability in sensitivity, specificity, and scanning techniques. rCBV maps can help identify focal regions within a brain tumor for biopsy. Perfusion data can be used to differentiate glioma from metastasis and to differentiate tumor recurrence or progression from the similar-looking enhancement that is secondary to posttherapy radiation necrosis. Care must be given to consider vascular lesions such as arteriovenous malformation or venous varix, which can mimic mass lesions with elevated blood volume but often can be differentiated on the basis of morphologic characteristics. Among extra-axial tumors, lower- grade meningiomas often demonstrate markedly elevated cerebral blood volume (CBV) ( Fig. 144.1 ), consistent with its typical angiographic features: early arterial blush and delayed washout.
Tumor cellularity, or the density of tumor cells per unit volume they occupy, is a prognostic histologic marker. The tumor cell density has been shown to directly correlate with CT attenuation values, with regions of hypercellularity demonstrating hyperdensity. On MRI, apparent diffusion coefficient (ADC) values derived from diffusion-weighted imaging (DWI) have also been correlated with cell density. Hypercellularity typically manifests as reduced diffusivity on the ADC map. In the setting of gliomas, higher-grade tumors typically demonstrate hypercellularity. Tumor cellularity also has diagnostic value in differentiating lesion types, selecting biopsy sites, and evaluating treatment response. For example, central nervous system (CNS) lymphoma is well known for its higher cellularity than other common CNS tumor types , ; moreover, management of CNS lymphoma is nonsurgical and based primarily on chemoradiation regimens. Therefore preoperative assessment of tumor cellularity can help define surgical goals in terms of both making the decision regarding biopsy versus resection and determining the biopsy site by targeting the hypercellular component of the tumor. Germinomas and medulloblastomas are also hypercellular, a feature that can aid their diagnoses when patient demographics and tumor locations are considered. ,
It is important to recognize that these imaging markers of cellularity have limitations—namely, recent intratumor hemorrhage can appear as hyperdensity on CT and, depending on the age of the blood products, the attenuation values may overlap with those of hypercellular tumor. Lack of contrast enhancement can be a useful sign to distinguish between the two. Calcifications can also appear as increased densities within tumor, although in most cases these calcifications are either coarse or stippled and readily distinguished from hypercellular tumors. ADC values of tumor can also be decreased by the presence of blood products and can also be observed in several nontumor processes, such as abscess and infarct, requiring correlation with presenting clinical signs and symptoms, as well as other imaging features.
Necrosis, generally seen as nonenhancing tissue with irregular and sometimes nodular rim enhancement, is a common imaging feature in high-grade gliomas, particularly in glioblastomas, although necrosis observed in histologic specimens of glioblastomas may not be evident on imaging. Metastasis also frequently demonstrates necrosis and appears similar to glioma when manifesting as a solitary mass. Necrosis is uncommon in lymphomas among immunocompetent patients; in the immunocompromised population, tumor necrosis is much more common and can mimic other brain lesions, such as toxoplasmosis. Following chemotherapy or radiation therapy, necrosis can commonly occur within and around tumor tissues, occasionally accompanied by enlargement of overall tumor size, requiring close imaging follow-up to determine durability of treatment response.
Cysts are frequently observed in a number of primary brain tumors, including hemangioblastoma, pilocytic astrocytoma, desmoplastic infantile ganglioglioma (DIG), dysembryoplastic neuroepithelial tumor (DNET), ganglioglioma, and craniopharyngioma. Identification of cysts can often narrow the diagnosis to include these tumors when combined with patient’s age, tumor location, and presenting symptoms. When cystic lesions are encountered, it is important to consider infectious causes such as brain abscesses, particularly when the content of cysts shows low diffusivity (hyperintensity) on DWI. Unlike postchemotherapy or postradiation necrosis, which typically indicates treatment response, growth of cysts is often a sign of tumor growth and treatment resistance.
Intratumoral calcifications are frequently found in a number of intracranial tumors, most notably meningiomas, oligodendrogliomas, neurocytomas, and craniopharyngiomas. On CT, calcifications tend to exhibit density greater than 100 HU, and this threshold allows differentiation of calcification from other dense materials including fibrosis and blood products. The signal characteristics of calcification are variable on MRI sequences depending on its chemical environment, but it is often faintly hyperintense on T1-weighted imaging and hypointense on T2-weighted imaging. Calcification is commonly observed in meningiomas and is an imaging marker of lower tumor grade and longer survival. , Presence of calcification in an extra-axial mass is also a helpful sign to distinguish meningioma from other extra-axial tumors such as dural metastases. The calcifications of oligodendrogliomas tend to be coarse and, when combined with the typical cortical involvement, allow these tumors to be diagnosed with high specificity. Among brain metastases, mucinous adenocarcinomas from genitourinary or gastrointestinal origins, osteosarcomas, and chondrosarcomas are sometimes associated with intratumoral calcifications. Untreated lymphomas rarely calcify; yet, as with many other tumor types, calcifications commonly occur after lymphoma treatment.
Magnetic resonance spectroscopy (MRS) can noninvasively measure concentrations of tissue metabolites and has shown promising applications in evaluating brain tumors, including their diagnosis, grading, pretherapy planning, and posttherapy assessment. Modern MR equipment allows for acquisition of in vivo spectroscopic data from regions of interest on the order of 1 cm 3 . MRS can be obtained using single-voxel spectroscopy (SVS) technique, through manual selection of target lesions on the basis of conventional T1- or T2-weighted sequences. Alternatively, the multivoxel spectroscopy (MVS) method can produce two- or three-dimensional spatial maps of both tumor and peritumoral regions for better delineation of specific regional metabolic changes in cases of heterogeneous tumor or posttreatment changes ( Fig. 144.2 ). Chemical shift imaging (CSI) is a method that uses an MVS data set to display regional variation in specific metabolites in a voxelwise method using a gray or color scale.
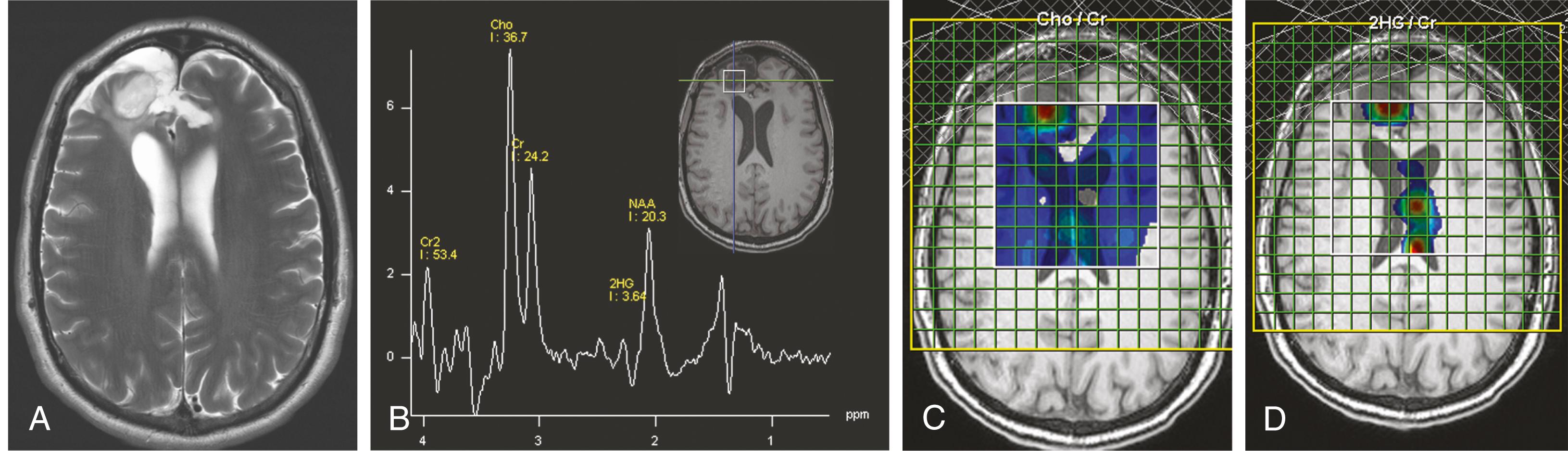
The most commonly analyzed metabolites in brain and brain lesions include N -acetyl aspartate (NAA), choline (Ch), creatine (Cr), myo-inositol (mI), lactate (lac), and lipid. NAA is a neuronal marker that decreases in concentration in most known brain pathologic conditions that damage neurons, including tumor, inflammation, and infection. The usual concentration peak can be absent when brain parenchyma is completely replaced by nonneuronal tissues such as metastasis, cyst, and abscess. Choline is a marker of cellular turnover and is typically elevated in neoplastic processes because of increased cellular proliferation. In certain tumor types, particularly glioblastomas, choline levels can be many times higher than in normal brain. Elevation of the Ch:NAA ratio in the peritumoral region can be a sign of tumor infiltration rather than edema induced by tumor, and this finding may allow differentiation of high-grade gliomas from brain metastases. , A high mI concentration has been observed in low-grade astrocytomas. Lipid and lactate levels are best measured using a short echo time (TE) (32 milliseconds); they typically increase with higher tumor grade as a result of hypoxia and necrosis and are associated with poor survival. MRS has also been optimized to detect a subtype of gliomas with isocitrate dehydrogenase ( IDH1 and IDH2 ) mutations on the basis of elevated 2-hydroxyglutarate concentration , (see Fig. 144.2 ), thus providing promising opportunities to preoperatively diagnose gliomas carrying these mutations, , to determine extent of disease, and to monitor posttreatment efficacy. ,
Other metabolites observed in brain neoplasms include taurine in PNET, alanine in meningiomas, and glycine in high-grade pediatric tumors. Nonneoplastic lesions such as abscesses and tuberculomas often demonstrate elevations in amino acids and lipids. Inflammatory diseases, most notably in demyelinating processes, can also result in increased cell turnover and increased choline level, thereby posing a diagnostic dilemma requiring another imaging modality. MRS in conjunction with perfusion imaging has a sensitivity of 72% and a specificity of 92% in the differentiation of tumors from nonneoplastic lesions.
For infiltrative gliomas, it is well known from histologic analyses that glioma tumor cells often migrate far beyond the margin of the main tumor bulk defined by conventional imaging sequences. MRS can detect distant tumor infiltration with increased mI and glutamine levels in the contralateral hemisphere of patients with untreated glioblastomas. In one series, the area of abnormality defined by MRS was at least 24% larger than that delineated by T2-weighted imaging, and the accuracy of an elevated Ch:NAA ratio on MRS was confirmed with histologic findings for tumor cells. With the ability to more accurately define tumor margins, MRS can perform a valuable role in preoperative and preirradiation planning, as well as intraoperative imaging guidance. The Ch:NAA ratio can also help differentiate areas of tumor with the highest cell density from edema for biopsy target selection. , A Ch:NAA ratio greater than 2, a lactate:NAA ratio greater than 0.25, and the presence of lipid at MRS imaging allow demarcation of brain parenchyma infiltrated by tumor. Intraoperative MRS has helped differentiate tumor from a nontumor abnormality, as indicated by a high Ch:Cr ratio and by the presence of lactate in more than half of suspected cases in one series, improving both surgical success and patient outcome. A Ch:NAA ratio of more than 2.1 at MRS has been used to identify regions of aggressive tumor phenotype within glioblastoma to improve Gamma Knife radiosurgery.
In comparison with normal brain tissues, tumors often carry greater metabolic activity, which can be detected by positron emission tomography (PET) as increased uptake of fluorine 18 fluorodeoxyglucose ( 18 F-FDG), a radiolabeled glucose analogue. For primary brain neoplasms, the degree of 18 F-FDG uptake on PET has been correlated with both tumor grade , and patient survival. Increased 18 F-FDG uptake is not specific to tumor, however, being found in infectious and inflammatory processes; therefore PET using this tracer (FDG-PET) has a limited number of applications in the diagnosis of brain tumors.
Several potentially more useful amino acid radiotracers have been developed over the last 5 to 10 years and have been more readily adopted in Europe than in the United States to date. The radiotracer fluorothymidine F-18 (FLT) has been shown to predict glioma proliferation and survival but has surprisingly failed to discriminate between tumor progression and pseudoprogression. Fluoro-ethyl-tyrosine F-18 (FET) and methionine C-11 (MET) appear to be superior to FDG-PET in identifying glioma grade. FET uptake by gliomas has been shown to correlate with progression-free survival, to have prognostication value in lower-grade gliomas, and to serve as a predictor of IDH status. Perhaps the most promising amino acid radiotracer to date is fluorodopa F-18 (FDOPA), which has shown association with IDH status, growth rate in diffuse lower-grade gliomas, and survival in treatment-naïve gliomas.
Meningiomas express somatostatin receptors and therefore can be imaged with somatostatin analogues, of which the most common in the United States is gallium-68 DOTATATE. DOTATATE-PET is highly sensitive for intracranial meningioma, with the tumor differential diagnosis including hemangioblastoma and metastatic neuroendocrine tumor. DOTATATE-PET can help differentiate recurrent meningioma from posttreatment change, improve detection of meningioma intraosseous extension, and predict meningioma growth rate.
Meningiomas are the most common intracranial extra-axial neoplasm in adults, accounting for about one-third of primary CNS neoplasms in the United States. Meningiomas typically have higher density than normal brain parenchyma on CT, although the difference is small and these tumors can be difficult to differentiate from adjacent cortex without intravenous contrast. On MRI, meningiomas are typically isointense on T1-weighted images relative to gray matter, are slightly hyperintense on T2-weighted images, and demonstrate avid homogeneous enhancement ( Fig. 144.3 ). However, the signal characteristics of meningiomas can be highly variable, occasionally having cystic or necrotic components ( Fig. 144.4 ) and at times exhibiting fatty degeneration ( Fig. 144.5 ). Some reports suggest that syncytial, transitional, and angioimmunoblastic meningiomas may have differing signal intensity characteristics depending on their internal histology. Meningiomas may show stippled or coarse calcifications, which can be an important diagnostic clue for differentiating meningiomas from other malignant extra-axial lesions such as metastasis and lymphoma.
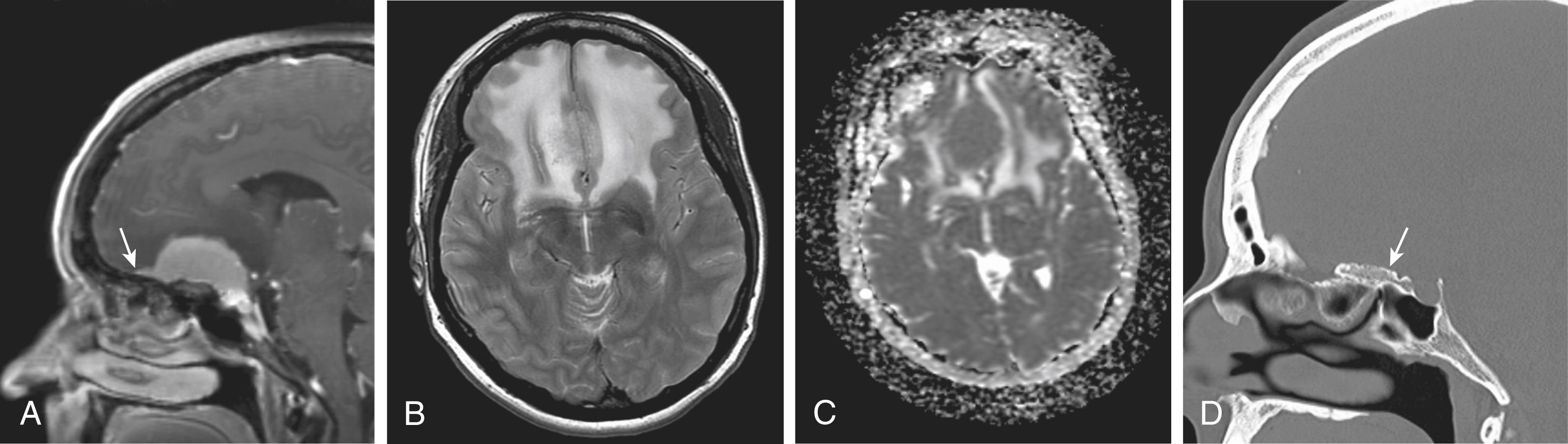
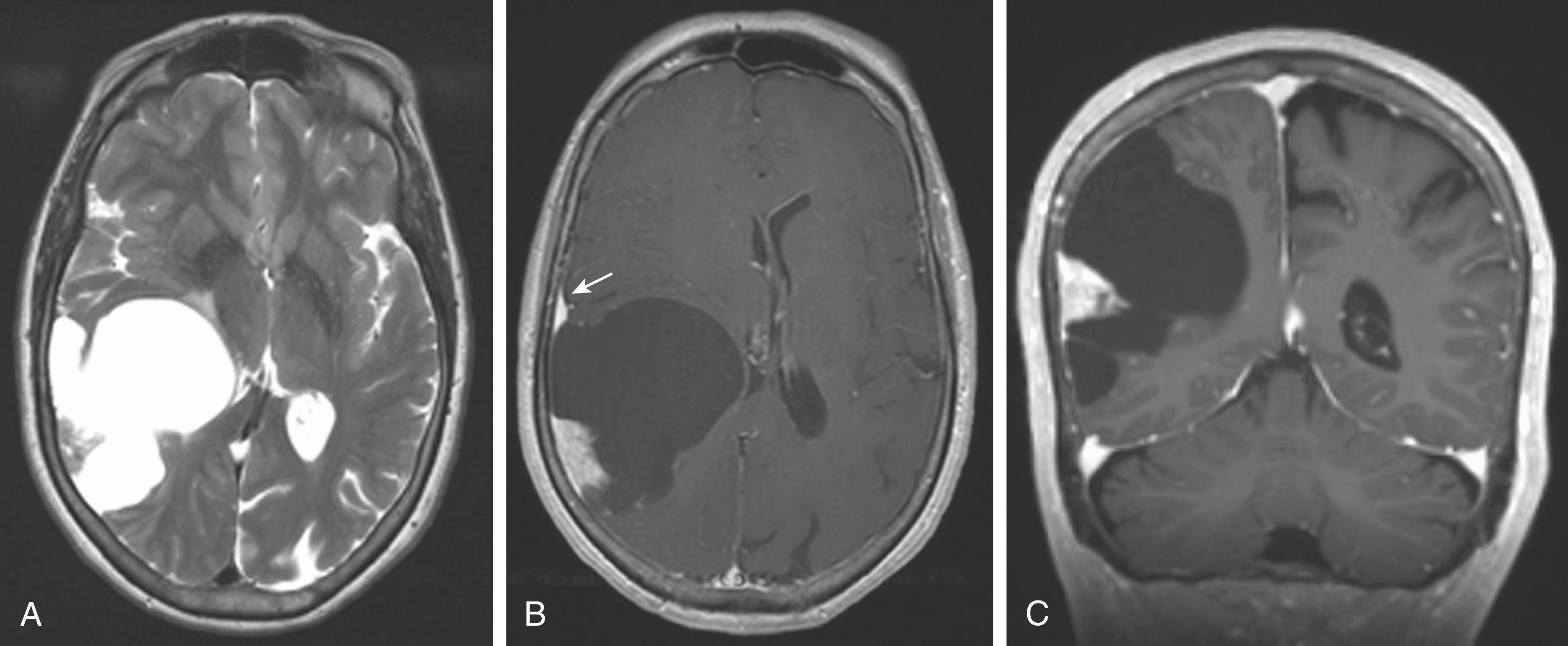
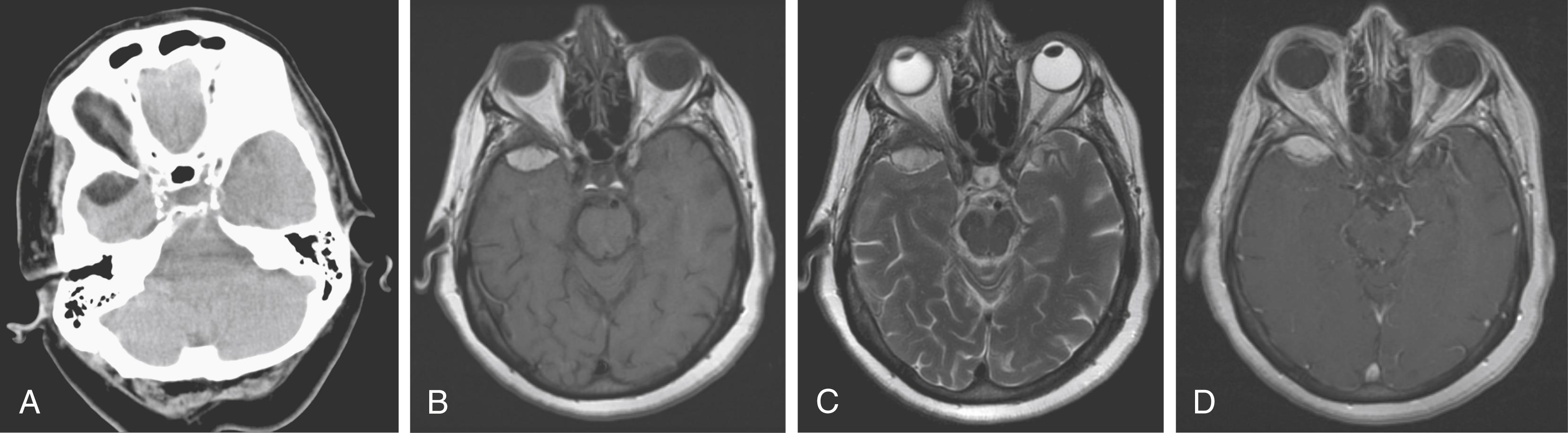
A widely discussed feature of meningiomas is the dural tail (see Fig. 144.3 ), which although highly sensitive for meningioma is not very specific, as it can be see with other neoplasms, such as dural-based metastasis and lymphoma, as well as nontumor etiologies, including sarcoidosis.
Bony hyperostosis can be observed adjacent to many meningiomas, best depicted on CT scans (see Fig. 144.3 ). Although these areas usually represent a reaction by osteoblasts to the tumor, in some cases meningiomas may permeate and expand the adjacent bones. Primarily lytic or destructive bony changes can occur with meningiomas, although these features are more commonly seen with other extra-axial neoplasms, such as hemangiopericytoma/solitary fibrous tumor and metastasis. Meningiomas can rarely invade brain parenchyma directly. The presence of vasogenic edema in association with meningiomas has been correlated with the lesion size as well as the degree of parasitization of dural venous structures.
The proton MRS features of meningiomas include absence of NAA and elevations of choline peaks. Alanine has been suggested to be a specific marker for meningiomas, but with variable sensitivities. On dynamic perfusion MRI, meningiomas typically show slow uptake of the contrast agent followed by its delayed clearance. This prolonged passage of contrast agent results in elevated CBV measurement, which can help differentiate meningiomas from dural metastases.
The blood supply of meningiomas can be evaluated by catheter angiography during preoperative planning. Meningiomas are typically supplied by branches of the external carotid arteries, including the middle meningeal arteries and the stylomastoid branches of the occipital arteries. At certain locations, meningiomas can receive additional blood supply from pial vessels. For example, tentorial arteries from the petrous internal carotid artery (ICA) may supply petroclival meningiomas. Meningiomas adjacent to cavernous sinuses may receive direct blood supply from branches of the cavernous ICAs, whereas those at the foramen magnum may be supplied by branches of the vertebral arteries or posterior inferior cerebellar arteries.
Schwannomas are the second most common intracranial extra-axial tumor. The majority of intracranial schwannomas occur in the cerebellopontine angle near the internal auditory canal (IAC), arising most often from one of the vestibular branches of the eighth cranial nerve. In this location, meningiomas are the other common tumor type that can have MR signal characteristics similar to those of vestibular schwannomas and can occasionally extend into the IAC, although they can be distinguished by the presence of dural tails. Vestibular schwannomas typically have components both within the IAC and within the posterior fossa cerebellopontine angle. They occasionally cause characteristic smooth widening of the IAC ( Fig. 144.6 ). In addition, vestibular schwannomas can contain cyst(s), necrosis, or hemorrhage and occasionally cause edema in adjacent brain tissue. Vestibular schwannomas can be discovered incidentally as small enhancing nodules within the IAC, although these small schwannomas are difficult to distinguish from other cause of perineural enhancement, such as neuritis, meningitis, and leptomeningeal metastases, requiring clinical correlation and often follow-up imaging. Occasionally, vascular loops or aneurysm formed by anterior inferior cerebellar arteries in the IAC can mimic tumor, particularly on low-resolution imaging, but can be distinguished by high-resolution MR or CT angiography.
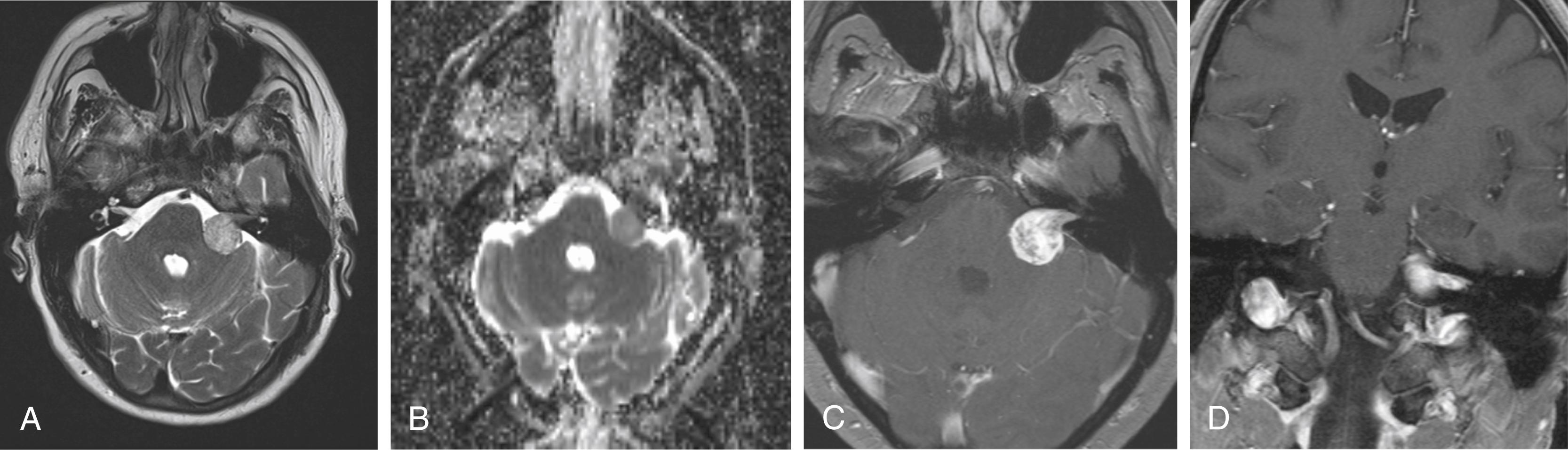
Schwannomas of other cranial nerves have imaging characteristics similar to those of vestibular schwannomas, but they can be distinguished by location and by the orientation of tumor growth. For example, trigeminal schwannomas track along a horizontal course from the lateral pons toward the Meckel cave inferolateral to the cavernous sinus. When these tumors extend extracranially through the foramen ovale, smooth widening of the bony foramen is typical. Schwannomas of the third, fourth, and sixth cranial nerves may manifest in the basal cisterns or within the cavernous sinus. When confined to the cavernous sinus, schwannomas can be difficult to distinguish from cavernous sinus meningiomas. Seventh cranial nerve schwannomas may occur in the cerebellopontine angle cistern, the IAC, or the temporal bone. They rarely are seen at the stylomastoid foramen region or in the parotid gland. Schwannomas of the 9th, 10th, and 11th cranial nerves are rarely seen in the intracranial compartment, but when they occur, they usually erode portions of the jugular foramen. Ninth cranial nerve schwannomas, in particular, occur more frequently in the intracranial compartment than in the head and neck region. Schwannomas of the 12th cranial nerves can cause widening of the hypoglossal canal and can be associated with clinical symptoms of tongue weakness as well as imaging findings of tongue atrophy. When multiple intracranial schwannomas are identified, neurofibromatosis type 2 should be highly suspected, and efforts should be made to search for other potentially associated intracranial tumor types, including meningiomas and ependymomas. This disease is termed MISME (multiple inherited schwannomas, meningiomas, and ependymomas) syndrome.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here