Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
A V/Q scan takes approximately 20 to 30 minutes and consists of two parts. During the ventilation part, the patient will have a face mask placed over his or her mouth and nose and will be asked to inhale oxygen and a radioactive gas that has no smell. The mask will be left on for approximately 5 to 10 minutes, and posterior projection scintigraphic images of the lungs will be obtained. Then the patient will be asked to lie supine in order to receive an intravenous injection of technetium-99m ( 99m Tc) radiolabeled macroaggregated albumin (MAA) to assess the blood flow to the lungs. Scintigraphic images of the lungs are then acquired in multiple projections over a period of approximately 20 minutes. There is no specific preparation for the patient, and the patient does not need to fast in preparation for the study. Although patients can receive oxygen, patients who are dependent on significant amounts of oxygen (i.e., require O 2 by face mask) are unlikely to be able to successfully perform the ventilation portion of the study, although the perfusion scan would not be affected.
The first imaging study performed in a patient with suspected pulmonary embolism is typically a chest radiograph. This will often reveal as well as exclude many underlying etiologies and is also necessary for the adequate evaluation of a V/Q scan. The next imaging study performed depends on a number of variables including the current diagnostic evaluation protocols regionally determined by individual hospitals but, more important, on whether the chest radiograph is normal or abnormal. Many hospitals now utilize contrast-enhanced computed tomography (CT) tailored toward evaluation of the pulmonary arterial tree to evaluate for presence of pulmonary embolism as well as for other cardiopulmonary disease conditions. In patients with significant abnormalities seen on chest radiography, it is more likely that a V/Q scan will result in an indeterminate test result and not provide additional diagnostic information. Therefore, only patients with relatively normal chest radiographs generally proceed to V/Q scanning. If a CT and/or a V/Q scan are equivocal for detection of pulmonary embolism, then conventional pulmonary angiography may be performed. Lower extremity ultrasonography (US) may also be used to evaluate for the presence of deep venous thrombosis (DVT).
133 Xe is a radioactive isotope of an inert noble gas. It can be inhaled into the lungs and will wash out quickly in a normal lung, although there will be persistent radiotracer activity (gas trapping) in parts of the lung affected by obstructive airways disease such as with asthma or chronic obstructive lung disease (COPD). These areas of gas trapping will typically correspond to matching perfusion defects on the perfusion scan, thereby increasing the specificity of the V/Q scan.
Radioaerosols are typically made from 99m Tc radiolabeled diethylene triamine pentaacetic acid (DTPA) particles suspended in air. Following inhalation, such aerosols are deposited on the lining of the alveolar spaces and therefore do not wash out. Although the presence of gas trapping in the lungs cannot therefore be assessed, the particles remain in the lungs and allow for images to be obtained in multiple projections that can be more easily compared to the perfusion images or via single photon emission computed tomography (SPECT) imaging.
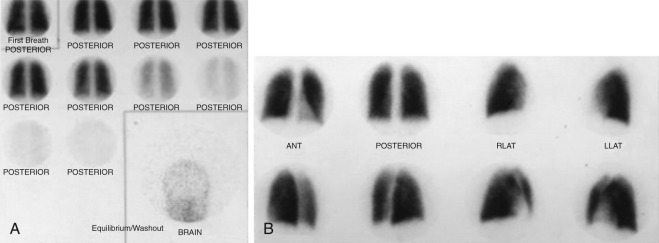
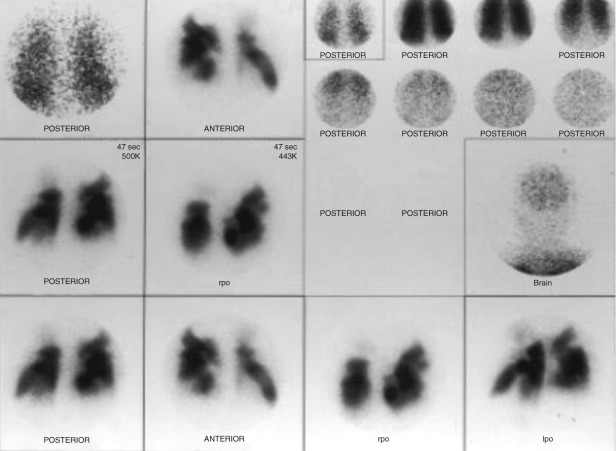
A normal V/Q scan ( Figure 79-1 ) consists of uniform ventilation throughout both lung fields. On a 133 Xe ventilation scan, there is usually good inflow of the gas, uniform radiotracer activity in the lungs during the equilibrium phase that lasts approximately 3 minutes as the patient breathes into the closed system of the machine, and then rapid and uniform washout from the lungs within about 1 to 2 minutes. No radiotracer activity should be observed in the brain, because this would imply the presence of a right-to-left shunt ( Figure 79-2 ). On the 99m Tc-MAA perfusion scan obtained in the supine position, uniform radiotracer uptake is seen throughout the lungs.
The early data on V/Q scans came from the Prospective Investigation Of Pulmonary Embolism Diagnosis (PIOPED) study, which divided scan results into low, intermediate, and high probability for pulmonary embolism (PE); the latest trend in V/Q scan interpretation is sometimes referred to as the trinary interpretation system. In this system, V/Q scans are interpreted as “PE absent,” “PE present,” or “nondiagnostic.” The “PE present” interpretation refers to one or more wedge-shaped perfusion scan defects, segmental or subsegmental, unmatched to any finding on the ventilation scan or the chest radiograph. If the perfusion scan is normal, or has nonsegmental defects (whether or not they are matching), the study is interpreted as “PE absent.” Any study that does not fall into either of the aforementioned categories, or cannot be interpreted due to extensive parenchymal abnormalities on the chest radiograph, is referred to as “nondiagnostic.”
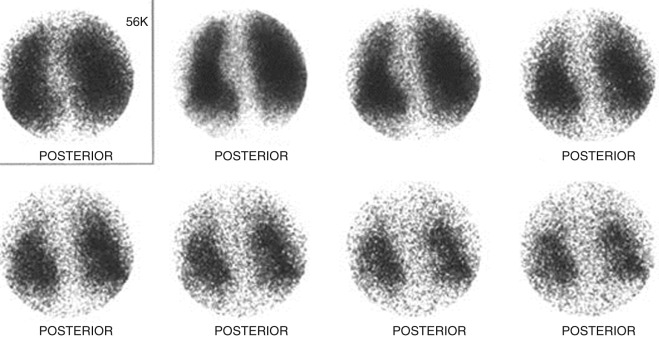
Gas trapping refers to radioactive gas that persists in certain areas of the lungs during the washout phase of the ventilation scan. Potential causes for gas trapping are listed in Box 79-1 . The implication of gas trapping is that there is an airway process that is contributing to the patient's clinical symptoms or signs. Regardless of the underlying cause, a perfusion scan defect that matches an area of gas trapping on the ventilation scan would not be due to an embolic perfusional abnormality.
Asthma
COPD
Chronic bronchitis
Mucous plug
Cystic fibrosis
Smoke inhalation
Airways-obstructive tumor
Airways-obstructive foreign body
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here