Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Until 2018, pulmonary arterial hypertension (PAH) was formally defined as a mean pulmonary artery pressure (mPAP) of greater than or equal to 25 mm Hg at rest, accompanied by a pulmonary vascular resistance (PVR) of greater than 3 Wood units with a normal pulmonary artery wedge pressure (<15 mm Hg) in the absence of any known cause of pulmonary hypertension (PH). A recently revised World Health Organization (WHO) classification system for PAH decreased the upper limit of mPAP from 25 mm Hg to 20 mm Hg. In both prior and revised classification schemes, PAH encompasses the first of the five groups of PH. The pathophysiology and clinical characteristics of Groups 2 through 5 of PH (i.e., PH associated with left-sided heart disease; lung disease/chronic hypoxia; thromboembolic PH; and other groups) are reviewed in Chapter 56 . In this chapter, we will focus on WHO Group 1, PAH, which includes idiopathic and hereditary PAH as well as PAH associated with various secondary diseases ( Box 55.1 ). Until improved therapeutic options became available during the past two decades, PAH was considered a rare but rapidly progressive, devastating condition, leading to death from right heart failure by a median of 2.8 years from the time of diagnosis. In recent years, an improved conceptual framework has been developed to better delineate the pathogenesis and clinical presentation of PAH, accompanied by improved directed therapeutic approaches. Nonetheless, PAH still carries a 9% 1-year mortality rate, and current therapeutics have been more effective at slowing illness progression rather than reversing or curing the disease. This chapter will highlight the current molecular understanding of the complex disease, via the still incompletely characterized interplay of genetic and exogenous upstream stimuli with downstream vascular effectors. This framework will then be coupled to the current understanding of the clinical presentation and progression of PAH, and the current and evolving modalities for treatment.
Modified from Simonneau G, Montani D, Celermajer D, et al. Haemodynamic definitions and updated clinical classification of pulmonary hypertension. Eur Respir J . 2018 [Epub ahead of print].
1 Pulmonary arterial hypertension (PAH)
1.1 Idiopathic PAH
1.2 Heritable PAH
1.3 Drug and toxin induced PAH
1.4 PAH associated with
1.4.1 Connective tissue disease
1.4.2 HIV infection
1.4.3 Portal hypertension
1.4.4 Congenital heart disease
1.4.5 Schistosomiasis
1.5 PAH with long-term response to calcium channel blockade
1.6 PAH with overt features of pulmonary veno-occlusive disease or pulmonary capillary hemangiomatosis
1.7 Persistent PH of the newborn
While PH in general is relatively common, PAH is a rare disease, with recent estimates placing the prevalence at 15 to 50 cases per million worldwide. Of these, idiopathic PAH has been reported with an annual incidence of one to two cases per million persons, and is thought to account for at least 40% of all PAH cases. While diagnoses of heritable causes of PAH are on the rise, the overall prevalence likely accounts for a very small fraction of total PAH prevalence, as reviewed recently. PAH associated with secondary illnesses is thought to account for the remaining cases. For instance, 7% to 12% of patients with systemic sclerosis develop PAH. Moreover, while the prevalence of PAH secondary to human immunodeficiency virus (HIV) infection was originally reported as 0.5%, estimates in sub-Saharan African populations suggest this number may be much higher. PAH associated with the newborn, termed persistent pulmonary hypertension of the newborn (PPHN), may occur in 0.2% of live-born term infants.
Overall, however, the exact incidence and prevalence of this disease are difficult to estimate on a global scale, given the difficulty of diagnosing PAH and overall limited access to healthcare worldwide. The disease affects women more frequently than men (1.7:1). This female predominance is exaggerated in the population of African descent (4.3:1), although the overall racial distribution of patients reflects that in the general population. Primary PAH presents most commonly in the fourth decade of life; ages range from 1 to 81 with 9% of the patients older than 60 years of age. Some sources cite a similar gender ratio among children diagnosed with the disease, whereas others note an equal distribution between male and female children. Primary PAH is typically difficult to diagnose, and the average time from the onset of symptoms to diagnosis was 2 years in the NIH Registry, thus resulting in most patients suffering from a more severe stage of disease at initial diagnosis (New York Heart Association [NYHA]/WHO Functional Classes III-IV). More recently, however, owing to improved clinical awareness coupled with more sophisticated invasive and noninvasive techniques for PAP measurements, time to diagnosis has decreased considerably, at least in the developed world.
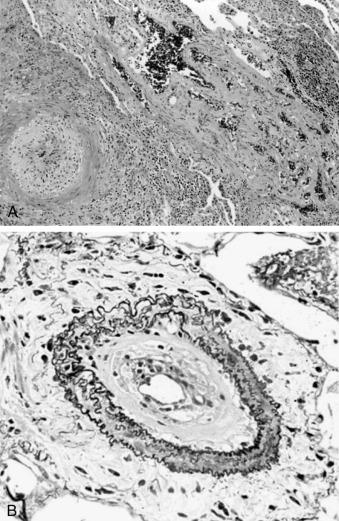
In humans, the natural history of PAH lesions is unknown, as patients usually present when the disease is advanced. The pathological appearance of severe PAH is similar regardless of the cause and reflects the end stage of a common response to pulmonary vascular injury. Common histologic features in nearly all types of PAH occur at the level of the small peripheral pulmonary arteries (100 to 1000 μm; Fig. 55.1 ); these include intimal fibrosis, distal localization and proliferation of vascular smooth muscle cells, and pulmonary arterial occlusion. Furthermore, a hallmark of severe, end-stage disease is the formation of a vessel “neointima,” characterized by increased deposition of extracellular matrix (ECM) and myofibroblasts. Plexiform lesions can predominate, characterized by overproliferation of endothelial-like cells encroaching upon the vessel lumen.
Multiple cell types in the pulmonary arterial wall and pulmonary arterial circulation contribute to the specific response to injury and the development of vessel remodeling ( Fig. 55.2 ). First, in the endothelium, it is increasingly appreciated that there exists extensive pathogenic reprogramming of pulmonary arterial endothelial cells (PAECs) in PAH, but these programs are complex and poorly understood. Early in the disease, it is thought that the endothelium serves as a central sensor of injurious stimuli, such as hypoxia, shear stress, inflammation, and toxins, leading to cell death and apoptosis. Such PAEC apoptosis has been observed readily in multiple types of animal and human forms of PAH, and plays a causative role particularly early in PAH to trigger pathogenesis. Apoptosis may trigger abnormalities in angiogenesis and contribute to the pathophenotype of pulmonary vascular rarefaction that is typical of PAH. Yet, in addition to apoptosis, increased PAEC proliferation also has been noted and linked to PAH pathogenesis. Historically, evidence for proliferation has included the study of plexiform lesions (previously described as “disorganized endothelial proliferation”). Moreover, recent studies have demonstrated that cultured PAECs isolated from human PAH patients demonstrate increased proliferation as compared with nondiseased control PAECs, accompanied by an imbalance of a multitude of downstream secreted vasoactive factors that contribute to overall increases of pulmonary vasomotor tone. Importantly, by modulating either microRNAs or matrix stiffness that consequently affect such endothelial proliferation, PAH manifestations improved in rodent models of PAH, indicating the importance of such proliferation to overall disease development. Other studies have isolated highly proliferative endothelial cells from PAH patients and multiple animal models of PH. In total, some investigators believe that endothelial apoptosis early in PAH initiates the selection of apoptosis-resistant endothelial cells that can further proliferate and drive later stages of disease. Yet it is also possible that a single or distinct population of proliferative endothelial cells may exist that continually transforms cellular identity, such as in the endothelial-to-mesenchymal transition that has been observed in PAH.

Unlike diseased PAECs where apoptosis and proliferation may contribute in parallel to PAH, pathogenic function of pulmonary artery smooth muscle cells (PASMCs) is characterized by a pro-proliferative and antiapoptotic phenotype. In these diseased PASMCs, numerous proliferative signaling pathways are dysregulated, accompanied by a profound metabolic shift involving a deregulation of oxidative cellular metabolism in favor of glycolysis. This hyperproliferative, antiapoptotic, and glycolytic phenotype of the vasculature in PH has drawn comparisons to the cellular phenotype (Warburg effect) observed in cancer, collectively contributing to proliferation and resistance to apoptosis. Recently, extrapolation of this “cancer theory of PAH” has led to a reported association of developing PAH with lung cancer. By end-stage disease, such processes result in substantial remodeling and medial arteriolar thickening, leading to a hypercontractile phenotype.
Pulmonary arterial adventitial fibroblasts (PAAFs) also display increased proliferative capacity in PAH and undergo a similar metabolic shift as diseased PASMCs. In response, diseased PAAFs can orchestrate a variety of alterations in the ECM driving profound vascular stiffening. The study of vascular stiffness is an emerging principle in PAH. Stiffness occurs in the proximal and distal pulmonary arterial tree in various forms of PAH, and stiffness is an index of disease progression. Vascular ECM remodeling occurs through changes in the balance between collagen and elastin deposition, matrix degradation, and matrix remodeling via collagen crosslinking enzymes such as lysyl oxidase (LOX). Metalloproteinase activation in the ECM can also induce cellular migration and leads to the production of additional mitogenic factors. Recent studies have reported that vascular matrix stiffness is not merely a consequence of long-standing disease but, rather, an early, pervasive driver of PAH. Consequent metabolic and proliferative reprogramming in PAAFs as well as PAECs and PASMCs has been directly linked to mechanoactivation after exposure to stiff matrix as well as inflammatory cell activation.
In addition to the importance of canonical cellular layers of the vascular wall, dysfunction of alternative vascular components may participate in these processes. Multiple lines of evidence now converge to connect immune dysregulation to clinical PAH in humans and animal models. Previous reports suggest altered inflammatory dynamics, such as hematopoietic and myeloid expansion, B- and T-cell dysfunction, mast cell activation, increased cytokine production, circulating autoantibodies, and tertiary lymphoid tissue neogenesis, may initiate or drive PAH. Clinically, there is a well-established causative link between autoimmune connective tissue disorders and PAH. Furthermore, infective agents, such as Schistosoma mansoni , HIV, and recently endogenous retrovirus HERV-K, are known to alter the immune cell repertoire and predispose to the development of PAH. Consistent with a significant presence of T and B cells in remodeled vascular lesions in end-stage PAH, lymphocytes have been implicated in a severe inflammatory state in this disease. Athymic nude rats, which lack functioning T cells, display greater sensitivity to PAH. T cell dysregulation may figure prominently, as regulatory T cells (T reg ) are increased while CD8 + cytotoxic cells are decreased in idiopathic PAH. An alteration of the helper T cell response (TH1 vs. TH2 vs. TH17) may also factor into the pathogenic response, but these features have not been described fully. Myeloid leukocytes, especially macrophages, are among the primary effectors of inflammation in pulmonary lesions in PH patients. A role of macrophages in aggravating PH pathogenesis has been proposed. A number of soluble chemoattractants and proinflammatory cytokines are upregulated in human and animal models of severe PAH. These include interleukin-1β, interleukin-6, interleukin-8, transforming growth factor-β1, bradykinin, monocyte chemotactic protein-1, fractalkine, RANTES, tumor necrosis factor (TNF)-α, and leukotrienes, among others. In particular, macrophage-derived leukotriene B4 has been implicated in mediating both endothelial and fibroblast dysregulation in PAH. A further mechanistic understanding of the exogenous or endogenous factors that drive immune dysfunction awaits elucidation.
Activated platelets appear to predominate in later stages of PAH, with histological evidence of in situ thrombosis in diseased arterioles of end-stage PAH. Finally, circulating or resident progenitor cells have been proposed to factor significantly in vessel wall injury and repair; dysregulation of these functions may also contribute to PAH. Yet our understanding is still limited regarding the mechanistic role of these cellular populations in disease progression.
Importantly, the WHO classification of PAH refers to distinct patient groups that cluster according to clinical association. In recent years, these clinical associations have been defined by much more precise molecular mechanisms that are now believed to be important in initiating or triggering this disease.
An understanding of the mechanism of genetic predisposition to PAH is of paramount importance for the identification of the root pathogenesis ( Fig. 55.3 ). The familial variety of idiopathic PAH accounts for at least 6% of all cases of PAH. Pedigree analysis has demonstrated an autosomal dominant inheritance but with variable penetrance, as only 10% to 20% of putative genetic carriers develop clinical PAH. Genetic anticipation is present, as each successive generation of affected families is afflicted at a younger age and with greater severity compared with the preceding generation.

Mutations in the transforming growth factor-β receptor (TGF-β receptor) superfamily have been genetically linked to PAH and play a causative role in the development of disease. The most prevalent cohort of hereditary PAH patients carries mutations in the bone morphogenetic protein receptor type 2 ( BMPR2 gene). More than 140 mutations in BMPR2 have been reported in patients with familial PAH, mainly located in the extracellular ligand-binding domain, in the cytoplasmic serine/threonine kinase domain, or in the long carboxyterminal domain. These account for 70% of all familial pedigrees of PAH and 10% to 30% of idiopathic PAH cases. BMPR2 loss-of-function mutations have only been found in the heterozygous state. The absence of BMPR2 mutations in some familial cohorts and in most of the sporadic cases indicates that additional, unidentified genetic mutations can also predispose to development of PAH. Furthermore, the presence of incomplete penetrance (approximately 25% of carriers in affected families develop clinical PAH) and genetic anticipation suggest that BMPR2 mutations are necessary but alone insufficient to result in clinically significant disease.
The mechanism of action of BMPR2 is complex, and its role in PAH progression is still unclear ( Fig. 55.4 A ). It functions as a receptor with serine/threonine kinase activity, and it activates a broad and complex range of intracellular signaling pathways. Upon binding one of many possible BMP ligands, BMPR2 forms a heterodimer with one of three type-I receptors. BMPR2 phosphorylates the bound type-I receptor, which, in turn, phosphorylates one of the Smad family of proteins to allow for nuclear translocation, binding to DNA, and regulation of gene transcription. Alternatively, BMPR2 activation can also lead to signaling via the LIM kinase pathway, the p38/MAP kinase/ERK/JNK pathways, or the c-Src pathway, independent of Smad activation.

The cellular effects of BMPR2 activation are multiform and complex. In the adult, BMPR2 is expressed predominantly in the pulmonary endothelium, medial smooth muscle cells, and macrophages. Under normal conditions, BMP ligands bind BMPR2 to suppress the growth of vascular smooth muscle cells. In contrast, binding of BMP2 and BMP7 to BMPR2 in pulmonary endothelium protects against apoptosis. It has been found that selective enhancement of BMPR2 signaling with BMP9 can reverse PAH. Furthermore, BMPR2 signaling has been linked to numerous cellular pathophenotypes important in driving PAH, including metabolic dysfunction, angiogenesis, endothelial-to-mesenchymal transition, cell survival via peroxisome proliferator-activated receptor-gamma (PPAR-γ) signaling, macrophage recruitment, and endothelial migration, among others. These dysfunctional signaling pathways have been corroborated in multiple rodent models of PAH, as well as endothelial cells derived from inducible pluripotent stem cells (iPSCs) of patients carrying pathogenic BMPR2 mutations. In correlation, pulmonary levels of BMPR2 are reduced both in familial cases of PAH without any BMPR2 mutation and in cases of secondary PAH. Thus dysregulation of the BMP signaling pathway may be a common pathogenic finding in multiple types of PAH, due to genetic or exogenous stimuli. However, the comprehensive in vivo effects of these mutations have been difficult to decipher. Specifically, robust PAH has been difficult to reproduce in mouse and rat models harboring specific BMPR2 heterozygous mutations, again suggesting that dysfunctional BMPR2 is likely insufficient alone to cause disease. As a result, a clear mechanistic explanation of the impact of BMPR2 mutations on pathogenesis remains elusive.
In addition to mutations of BMPR2, other genetic causes of PAH have been identified in recent years, owing to the advances in genomic sequencing and genome-wide association studies (GWAS). In correlation with the extent of BMPR2 mutations found in hereditary PAH, pathogenic mutations of other BMP/TGF-β superfamily members have been identified in PAH. For instance, a rare group of patients with hereditary hemorrhagic telangiectasia (HHT) and PAH harbor specific mutations in ALK1 or endoglin , genes encoding two such members of the TGF-β receptor superfamily. Other related mutations to BMP/TGF-β signaling include those in the genes SMAD9 and caveolin 1 . Rare mutations in the potassium two-pore-domain channel subfamily K member 3 (KCNK3) have been described as pathogenic and thought to control ion channel homeostasis and electrical conduction in diseased PASMCs. By candidate gene strategy approaches, mutations in the gene encoding T-box 4 have been identified in 10% to 30% of pediatric PAH patients, but rarely in adults with PAH. A GWAS identified an association at the CBLN2 locus with PAH but has been difficult to replicate in independent cohorts. Finally, biallelic EIF2AK4 mutations have been identified as a cause of pulmonary veno-occlusive disease (PVOD), a related form of PAH; in some cases, these mutations have been found in PAH patients, either singly or accompanied by BMPR2 mutations. (Additional genes including the water channel AQP1, the ATPase ATP13A3, and more recently Sox17 and HLA-DPA1/DPB1 have been implicated in hereditary PAH. )
In addition to these primary gene mutations, alternative mechanisms involving complementary “modifier” genes may also contribute to a genetic predisposition to PAH. The most promising data identifying such modifier genes have analyzed the association of particular single nucleotide polymorphisms (SNPs) with the development of PAH. Some analyses of specific SNP variants have suggested certain genes, such as the serotonin transporter (SERT), Kv1.5 , and the TRP cation channel, subfamily C, member 6 ( TRPC6 ). Such associations may not reflect a causal relationship, and thus additional mechanistic data are necessary for proper interpretation.
In addition to genetic predisposition, development of PAH likely depends on a variety of physiologic, acquired, and/or exogenous stimuli. Some of these factors have been studied to a sufficient degree to hypothesize a potential pathogenic mechanism(s) (see Fig. 55.3 ).
In idiopathic PAH, a paradigm of sex predisposition has evolved. Historically, the incidence and prevalence of PAH has been demonstrably higher in females as compared with males in multiple cohort registries. For example, the REVEAL registry, based in the United States, reported a female to male ratio of 4.1:1 in idiopathic PAH patients as compared with a published French registry (1.9:1) and the National Institutes of Health registry (1.7:1). A female bias was also reported in other subtypes of Group 1 PAH, including PAH due to congenital heart disease (2.8:1), PAH due to connective tissue disease (9.1:1), and PAH secondary to drugs and toxins (5.4:1). However, a clinical paradox has emerged. Namely, these registries have suggested that when males develop PAH, they tend to present at a much earlier age and have poorer prognosis and survival. Thus increased female susceptibility to disease is balanced by enhanced survival compared with males.
The molecular bases for these observations remain incompletely described. Recent advances have focused on alterations of sex-hormone signaling, mainly in regard to estrogen and its related metabolites. Historically, this concept has been based on observations that PAH has been associated with oral contraceptive (OCP) use. Hormone replacement therapy has also been associated with severe PAH in postmenopausal women. However, a direct mechanistic link between estrogen and PAH has been challenging to prove, given a separate paradoxical finding that many standardized rodent models of PAH are protected from disease with estrogen. Importantly, there are some specialized genetically altered rodent models in which PAH is more prevalent in females. Notably, in rats exposed to both SU5416 (a VEGF2 receptor antagonist) with chronic hypoxia, the aromatase inhibitor anastrozole, an anti–breast cancer drug that prevents the production of estrogen, and metformin, an antidiabetic drug that also inhibits aromatase, both protect against PAH. Clinical trials of anastrazole in PAH are ongoing. Furthermore, recent genetic evidence from mice genetically deficient in both estrogen receptors has indicated that lack of estrogen signaling protects against PAH in BMPR2 mutant mice via reducing the burden of metabolic deficiencies in the pulmonary vasculature. Estrogens may interact with several modifying factors such as serotonin and BMPR2 to enhance potential damaging effects of estrogens on the pulmonary vasculature. Androgens, such as dehydroepiandrosterone, may also contribute but via incompletely described mechanisms. Interestingly, recent data from animal models have proposed a chromosomal explanation for the sex disparity in that the presence of the male Y chromosome can protect against PAH. Currently, it is thought that estrogens or differential sex hormone metabolism influence PAH risk among susceptible subjects in a context-specific manner. Yet it remains unclear why all estrogens and related metabolites do not behave similarly and sometimes paradoxically. Moreover, it is not fully known which factors and pathways may synergize with these hormones to converge on disease manifestation.
The pulmonary vascular response to hypoxia has been well studied in cell culture and in animal models, but its full impact on PAH is unclear. In general, pulmonary vascular responses in acute and chronic hypoxia are thought to drive WHO Group 3 PH due to chronic lung disease. Yet, at least in part, these cellular events in chronic hypoxia overlap with the remodeling events in end-stage PAH. Indeed, various forms of PAH have demonstrated the vascular upregulation of the master transcription factors of hypoxia, HIF-1α and HIF-2α, thus driving the “pseudohypoxic” cellular reprogramming important in disease progression. Recent work with mice carrying conditional genetic deficiencies of these transcription factors have implicated specifically endothelial HIF-2α as essential to the development of severe PAH, at least in mouse models of PAH. Acute hypoxia induces vasodilation in systemic vessels but induces vasoconstriction in pulmonary arteries. This acute and reversible effect is mediated in part by upregulation of endothelin-1 (ET-1) and serotonin, and also in part by hypoxia- and redox-sensitive potassium channel activity in pulmonary vascular smooth muscle cells. Coordinately, these events lead to membrane depolarization in smooth muscle cells, increase in cytosolic calcium, and vasoconstriction. In contrast, chronic hypoxia and HIF-activation induce a range of vascular cell reprogramming events. In PASMCs and PAAFs, these events are centered on a profound metabolic shift favoring glycolysis over oxidative metabolism, proliferation, migration; and deposition, remodeling, and crosslinking of ECM. In PAECs, these events influence angiogenesis, elaboration of vasoactive effectors promoting vasoconstriction, and, more recently described, endothelial-to-mesenchymal transition. However, because the histopathology of hypoxic PH does not recapitulate all aspects of PAH, further mechanistic differences in pathogenesis certainly exist but have not yet been fully identified. These are important considerations, especially in the context of interpreting studies of hypoxic PH and extrapolating those findings to the pathogenesis of PAH.
Pulmonary arteriopathy complicates autoimmune diseases, especially in the setting of the CREST variant of limited systemic sclerosis and, to a lesser degree, in mixed connective tissue disease, systemic lupus erythematosus (SLE), and rheumatoid arthritis, as recently reviewed. PAH has been reported in approximately 10% to 30% of patients with mixed connective tissue disease, 5% to 10% of patients with SLE, and more rarely in the settings of rheumatoid arthritis, dermatomyositis, and polymyositis. Sjögren syndrome may rarely be complicated by rapidly progressive PAH. It is particularly important to distinguish between PAH and thromboembolic PH in patients with SLE and antiphospholipid syndrome. The occurrence of PAH in each disease has been associated with the Raynaud phenomenon, suggesting at least some similarities in pathogenesis. The presence of interstitial lung disease and pulmonary fibrosis, seen at varying frequency in these autoimmune syndromes, may represent a common pathogenic factor in the development of PAH. More recently, significant perivascular inflammation has been hypothesized as a key feature linking various subtypes of PAH, including those associated with autoimmune diseases, which may increase vasoconstriction, proliferation, and vessel remodeling. Murine models of interstitial lung disease and/or autoimmune disease may prove important in further elucidating the pathogenic mechanisms.
Portopulmonary hypertension is defined as PAH associated with portal hypertension (portal pressure > 10 mm Hg), with or without hepatic disease, as reviewed previously. Approximately 9% of patients with severe PAH are reported to have portal hypertension. The diagnosis of PH is usually made 4 to 7 years after the diagnosis of portal hypertension, but it has occasionally been reported to precede the onset of portal hypertension. The correlation between the severity of portal hypertension and the development of PH is debated. The female predominance of primary PAH is not seen in this form of PAH. Because patients with nonhepatic causes of portal hypertension have been reported with this entity, it appears that it is the portal hypertension and not cirrhosis that triggers the development of PAH, yet the molecular mediators of portopulmonary hypertension are unknown. Hypotheses include an inability of the liver to metabolize serotonin and other vasoactive substances. Alternatively, the shear stress from increased pulmonary blood flow may result in endothelial injury, triggering a cascade of events that result in the characteristic adverse remodeling described earlier. The circulating marker macrophage migration inhibitory factor (MIF) has recently been proposed as a specific biomarker of portopulmonary hypertension, but its importance in promoting direct pathogenesis of this form of PAH is unclear. The risk of PH increases with duration of disease and tends to have a much worse prognosis than other forms of PAH. Notably, survival of portopulmonary hypertension patients in the United Kingdom National Pulmonary Hypertension Service was found to be worse than patients with idiopathic PAH, despite the advent of targeted pulmonary vasodilator therapy. Portopulmonary hypertension affects 4% to 6% of patients referred for liver transplantation. Although perioperative mortality in these patients is significantly increased in patients with a mean PAP greater than 35 mm Hg, recent retrospective studies have indicated stabilization and sometimes reversal of portopulmonary hypertension when using a combination of liver transplantation and targeted therapy. However, randomized control trials are lacking in the study of this form of PAH, thus making any treatment recommendations much less definitive.
Exposure to a number of drugs and toxins has been associated with PAH, but not all such toxins have been established as true pathogenic causes. Anorexigens have been confirmed as causes for at least two separate outbreaks of PAH. In the 1960s, aminorex fumarate was marketed as an over-the-counter appetite suppressant in Europe, which led to a 10-fold increase of PAH over the next 7 years in Austria, Germany, and Switzerland. Similarly, in 1996, fenfluramine/phentermine was a combined appetite suppressant approved by the Food and Drug Administration for marketing in the United States. A 23-fold increase of PAH was reported after taking this drug combination for 3 months. While different classes of drugs, these medications may carry similarities in promoting the expression of specific vascular mitogens. In the case of aminorex, its pharmacological effects are thought to be based mainly in the release of catecholamines, which themselves can increase vasoconstriction. In the case of fenfluramine/phentermine, this drug combination is thought to act as an inhibitor of serotonin reuptake and stimulator of serotonin secretion, thereby leading to increased levels of circulating, free serotonin. Serotonin is both a vasoconstrictor and mitogen that promotes smooth muscle hyperplasia and hypertrophy (see Fig. 55.4 B), and many lines of genetic and pharmacologic evidence now point to the dysregulation of serotonin and its signaling and transport pathways as causative for PAH. More recently, stimulants of the central nervous system, such as methamphetamines and cocaine, have become a more prevalent cause of PAH. In particular, methamphetamine-induced PAH is a severe disease subtype and portends a worse prognosis than other forms of PAH. The importance of serotonin release has been suggested in the mechanisms of methamphetamine-induced PAH; however, more recent studies have indicated a more complex yet still undefined pathogenic explanation, implicating endothelial mitochondrial dysregulation and DNA damage and autophagy in disease progression.
HIV infection predisposes to the development of PAH. There are epidemiologic challenges when studying the HIV-PAH population that have led to evolving notions of the exact prevalence of this disease. Originally, prevalence was estimated at 0.5% of HIV-positive individuals. However, echocardiographic evidence indicates that many more HIV-positive individuals suffer from higher pulmonary arterial systolic pressures (PASP) and right ventricle (RV) dysfunction in Africa and in the United States, with extrapolations of 1.2 to 3.4 million people in sub-Saharan Africa potentially exhibiting elevated pressures. Importantly, mortality risk in HIV-positive US veterans has been documented to be greater in all persons with higher PASPs. Notably, because echocardiography does not always correlate with invasive pressure measurements, it is unclear if echocardiographic estimates may suggest more subtle or early forms of pulmonary vascular dysfunction rather than overt PAH. However, the global majority of HIV-PAH patients does not have access to invasive hemodynamic study. Thus there is a pressing need to understand the underlying pathogenesis of HIV-PAH in order to design more accurate and noninvasive diagnostics that can track the underlying molecular mechanisms of disease.
Insights into the molecular pathogenesis of HIV-PAH are sparse. Depending on active HIV replication, suppressive antiretroviral therapy (ART) may ameliorate it. Yet ART neither prevents nor cures PAH. Direct HIV infection of the vasculature has not been observed. Contributing mechanisms may include effects of HIV viral proteins such as Nef, Tat, and gp120 or the HIV coreceptor CCR5 ; immune activation induced by HIV or comorbid infections; or risk factors (i.e., drug use ) in the HIV population. Diastolic left ventricular dysfunction may also contribute, as well. It had been proposed that human herpes virus 8 (HHV-8), the causative agent of Kaposi sarcoma and an opportunistic pathogen highly associated with HIV infection, may play a role in PAH development with progression to plexiform lesions, but that link has not been consistently validated after study of additional populations. Ultimately, HIV-induced PAH likely results from multifactorial effects, and the underlying pathogenesis may involve both direct results of viral infection and indirect consequences of associated pathogens.
Exposure to the parasite Schistosoma mansoni accounts for the most frequent cause of PAH in the developing world. While antiparasitic medications and prevention strategies are effective in the treatment of this subtype of PAH, economic, cultural, and political barriers have led to substantial prevalence of this tropical disease. At the molecular level, schistosomiasis-associated PAH is characterized by altered vascular TGF-β signaling, similar to other idiopathic, heritable, and autoimmune-based causes. Recently, the secreted effector thrombospondin-1 (TSP-1) was identified as a key upstream regulator of TGF-β activation and was both necessary and sufficient for developing PAH in Schistosoma-exposed mice. Pharmacologic TSP-1 blockade prevented experimental PAH and thus is being explored as a therapeutic approach for this subtype of PAH and perhaps other TGF-β-dependent vascular diseases.
Increased flow through the pulmonary circulation has long been associated with development of PAH. Certain types of congenital heart disease with functional systemic-to-pulmonary shunts, such as unrestricted ventricular septal defects (VSDs) and large patent ductus arteriosus (PDA), invariably lead to pulmonary vascular remodeling and the clinical syndrome of PAH during childhood (Eisenmenger syndrome). Approximately one-third of patients with uncorrected VSDs and PDAs die from PAH. The timing of surgical repair greatly influences the outcome. If the shunt is repaired within the first 8 months of life, patients tend to have normal pulmonary pressures regardless of pathologic findings; by contrast, patients operated on after age 2 tend to have persistent PAH. Importantly, when PVR equals or exceeds systemic vascular resistance, surgical correction of a shunt will increase the load on an already overburdened RV, worsen the clinical condition of the patient, and not reverse PAH.
The presence of atrial septal defects (ASDs) with systemic to pulmonary shunts may also lead to PAH over time. Yet, in contrast with cases of unrestricted VSD and PDA, only 10% to 20% of all persons with ASD progress to PAH. This observation may reflect differences in the response of the pulmonary vasculature to pressure overload (as seen in shunts with VSD and PDA) as compared with volume overload (as seen in shunts with ASD). Furthermore, patients with ASD may harbor a specific, unidentified genetic predisposition to the development of PAH that may exacerbate the increased volume load to the pulmonary circulation. Yet data supporting this hypothesis are scarce.
At the molecular level, the physiologic flow patterns of laminar shear stress, turbulent flow, and cyclic strain are all sensed by endothelial cells, leading to transduction of intracellular signals and modulation of a wide variety of phenotypic changes. Significant prior work has focused mainly on the endothelium of the peripheral vasculature, suggesting that laminar flow induces a vasoprotective, quiescent vascular state, while turbulent flow leads to a proinflammatory and thrombogenic state. It is unclear if these flow-dependent phenotypes are recapitulated in the pulmonary vasculature. In part, this stems from the difficulty of directly studying the in vivo or ex vivo flow patterns at the anatomic level of the pulmonary arteriole. Alternatively, studies of large animal models of pulmonary overcirculation have yielded mechanistic insights, implicating dysregulation of endothelial mitochondrial bioenergetics and reactive oxygen species (ROS) secondary to alterations in carnitine metabolism, nitric oxide synthase (NOS), and PPAR-γ. Therefore, chronically elevated flow may allow for the selection of cells with dysregulated endothelial cell growth and resulting clonal or polyclonal expansion to plexiform lesions. More recently, pulmonary overcirculation has been identified as a trigger for PASMC hyperproliferation via a decrease of both mitochondrial oxidative metabolism and glycolysis in favor of flux through the pentose phosphate pathway.
PPHN is characterized by persistent elevation of PVR, right-to-left shunting, and severe hypoxemia. PPHN can occur with pulmonary parenchymal diseases, including sepsis, meconium aspiration, pneumonia, or maladaptation of the pulmonary vascular bed, or without an apparent cause. Persistent PH in newborns may lead to death during the neonatal period, and severe cases may necessitate extracorporeal membrane oxygenation (ECMO). Approximately 14% to 46% of PPHN survivors develop chronic impairments, such as hearing deficits, chronic lung disease, and cerebral palsy, among other neurodevelopmental disabilities. Alterations in redox signaling and inadequate production of nitric oxide (NO) may be important contributors to persistent PPHN. Inhaled NO is useful in treating this disorder. More recently, other targeted pulmonary vasodilators have been studied as effective therapies in this form of PAH. An expert consensus statement has been released regarding best practices for diagnosis and management of pediatric PAH.
PVOD is a rare form of PAH defined by specific remodeling of pulmonary venules in the absence of histologic alterations in pulmonary arterioles. In the current WHO PH classification, PVOD and pulmonary capillary hemangiomatosis (PCH) are considered to be variants of PAH and common entities thought to reflect separate manifestations of the same root pathogenesis. Clinically, these disease entities offer challenging diagnostic dilemmas, owing to the difficulty in differentiating their presentations from true PAH affecting the pulmonary arterioles. Yet differentiating PVOD from PAH is an important clinical priority, since PVOD carries a worse prognosis, and on occasion fatal pulmonary edema can result from targeted pulmonary vasodilator therapy use in PAH. An accurate diagnostic algorithm for PVOD has been proposed, based on noninvasive testing utilizing specific oxygen parameters, low diffusing capacity for carbon monoxide, and characteristic signs on high-resolution chest computed tomography. Unfortunately, there is a lack of evidence-based recommendations for medical therapy of PVOD. Lung transplantation is the preferred definitive therapy for eligible patients. Molecular pathogenesis is still unclear. Prior studies have implicated the Ets transcription factor Erg and its partner the apelin receptor Aplnr in the pathogenesis of PVOD. Moreover, the recent discovery of biallelic mutations in the EIF2AK4 gene as a heritable cause of PVOD may spur substantial insight into the origins of this disease subtype in the near future.
Downstream of the genetic and acquired triggers of PAH, the histopathologic processes that predominate later stages of disease include vasoconstriction, cellular proliferation, and thrombosis. These processes are influenced by a complex and dysregulated balance of vascular effectors that serve as signaling messengers for cell-cell crosstalk, controlling vasodilation and vasoconstriction, growth suppressors and growth factors, and pro- versus antithrombotic mediators. Most of these effectors have been described in previous comprehensive reviews and will be described here specifically with regard to their known roles in the pathogenesis of PAH ( Table 55.1 ).
| Vascular Effector | Change in Activity in PAH | Effect on Vasoconstriction | Effect on Cell Proliferation | Effect on Thrombosis |
|---|---|---|---|---|
| Serotonin | Increased | Increased | Increased | Increased |
| Nitric oxide | Decreased (increased in plexiform lesions) | Increased | (?) Increased in plexiform lesions | Increased |
| Thromboxane A2 | Increased | Increased | Increased | Increased |
| Prostacyclin | Decreased | Increased | Increased | Increased |
| Endothelin-1 | Increased | Increased | Increased | (N/A) |
| Vasoactive intestinal peptide (VIP) | Decreased | Increased | Increased | Increased |
| Natriuretic peptides | Increased (from cardiomyocyte stretch) | Increased | (?) Decreased | (N/A) |
| Notch ligands | Increased | (N/A) | Increased | (N/A) |
Gaseous vasoactive molecules regulate pulmonary vascular homeostasis, and alterations in their endogenous production have been linked to the progression of PAH. NO is the best described of these factors (see Fig. 55.4 C). It is a potent pulmonary arterial vasodilator, as well as a direct inhibitor of platelet activation and vascular smooth muscle cell proliferation. NO diffuses into recipient cells (such as vascular muscle), where it activates soluble guanylyl cyclase (sGC) to produce cyclic guanosine monophosphate (cGMP). In turn, cGMP interacts with at least three different groups of effectors: cGMP-dependent protein kinases, cGMP-regulated phosphodiesterase (PDE), and cyclic-nucleotide-gated ion channels. The synthesis of NO is mediated by a family of NOS enzymes. In the pulmonary vasculature, the endothelial isoform (eNOS) figures most prominently and is regulated by a multitude of vasoactive factors and physiologic stimuli, including hypoxia, inflammation, and oxidative stress. Reduced levels and reduced activity of eNOS, reduced NO bioavailability, dysregulated intracellular NO transport via caveolae, and increased degradation of cGMP all aggravate PAH progression in human studies and/or animal models. Dysregulation of NO may also depend on still incompletely characterized processes of NO transport in blood. Specific polymorphisms of NOS have also been associated with PH. Together, these effects indicate a coordinated mechanism of dysregulated vasoconstriction. Correspondingly, murine models that genetically lack eNOS, GTP cyclohydrase-1 (the rate limiting enzyme for synthesis of an essential cofactor of NOS, tetrahydrobiopterin), or dimethylarginine dimethylaminohydrolase (DDAH, an enzyme important in degradation of NOS inhibitors) all display exaggerated susceptibility to developing PH in response to other endogenous stimuli. Finally, the impact of NO has been reflected in its therapeutic role in PAH, such as inhaled NO, NO intermediates such as nitrate and nitrite, and the NO-dependent PDE5 inhibitors (discussed in detail later).
The arachidonic acid metabolites prostacyclin and thromboxane A 2 also play crucial roles in vasoconstriction, thrombosis, and, to a certain degree, cell proliferation in the vessel wall (see Fig. 55.4 C). Prostacyclin (prostaglandin I 2 ) activates cyclic adenosine monophosphate (cAMP)–dependent pathways and serves as a vasodilator, an antiproliferative agent for vascular smooth muscle, and an inhibitor of platelet activation and aggregation. In contrast, thromboxane A 2 increases vasoconstriction and activates platelets. Protein levels of prostacyclin synthase are decreased in small- and medium-sized pulmonary arteries in patients with PAH, particularly with the idiopathic form. Biochemical analysis of urine in patients with PAH has shown decreased levels of a breakdown product of prostacyclin (6-keto-prostacyclin F 2 alpha), accompanied by increased levels of a metabolite of thromboxane A 2 (thromboxane B 2 ). Therefore, it appears that production of these effectors is coordinately regulated with the imbalance toward thromboxane A 2 favored in the development of PAH. The mode of this regulation remains to be characterized. Nonetheless, recognition of this imbalance has led to the success of prostacyclin therapy and improvement of hemodynamics, clinical status, and survival in patients with severe PAH.
ET-1 is expressed by pulmonary endothelial cells and has been identified as a significant vascular mediator in PAH (see Fig. 55.4 C). It acts as both a potent pulmonary arterial vasoconstrictor and mitogen of pulmonary smooth muscle cells. The vasoconstrictor response relies on binding to the endothelin receptor A (ET-A) on vascular smooth muscle cells, which leads to an increase in intracellular calcium, along with activation of protein kinase C, mitogen-activated protein kinase, and the early growth response genes c- fos and c- jun. The mitogenic action of ET-1 on pulmonary vascular smooth muscle cells can occur through either the ET-A and/or the ET-B receptor subtype, depending on the anatomic location of cells. ET-A predominantly mediates mitogenesis in the main pulmonary artery, whereas mitogenesis in resistance arteries relies on contributions from both subtypes. The resulting vasoconstriction, mitogenesis, and vascular remodeling are thought to lead to significant hemodynamic changes in the pulmonary vasculature and to PAH. Plasma levels of ET-1 are increased in animal and human subjects suffering from PAH due to a variety of etiologies and correlate with disease severity. Again, improvements in hemodynamics, clinical status, and survival of PAH patients treated with chronic ET receptor antagonists highlight the significance of these effects.
As described previously, serotonin is both a vasoconstrictor and mitogen that promotes smooth muscle hyperplasia and hypertrophy (see Fig. 55.4 B). Primarily stored in platelet granules, secreted serotonin binds G-protein-coupled serotonin receptors present on PASMCs. Activation of these receptors leads to a decrease in adenylyl cyclase and cyclic AMP, resulting in an increase in contraction. Furthermore, the cell-surface SERT allows for transport of extracellular serotonin into the cytoplasm of smooth muscle cells, thereby activating cellular proliferation directly through the action of serotonin or indirectly via potential pleiotropic mechanisms.
Numerous observations in idiopathic and familial disease, congenital disease, and environmental exposure have implicated the proliferative effects of serotonin in PAH. In idiopathic PAH, pulmonary expression of serotonin receptors is increased, and plasma levels of serotonin are chronically elevated. A mouse model of hypoxic PH parallels these changes. A positive association has been noted among patients with congenital platelet defects in serotonin uptake (i.e., delta storage pool disease) and development of PAH. As discussed previously, exposure to anorexigens, such as dexfenfluramine, is associated with levels of circulating serotonin. In mice, these changes are accompanied by increased 5-HT receptor type 2B response and inhibition of SERT responses. In humans, these changes correlate with an increased risk for the development of PAH. In addition, the L -allelic variant of SERT is associated with increased expression of the transporter and enhanced smooth muscle proliferation. In some human studies, this variant has been associated with an increased risk of PAH in the homozygous population.
Animal models of PH have also implicated the activated serotonin pathway in disease progression. Treatment with serotonin and chronic hypoxia in a rat model led to worsened hemodynamics and increased vessel remodeling. Exposure to increased serotonin led to worsened PH in a BMPR2 +/− heterozygote murine model. Similarly, overexpression of SERT in mice resulted in spontaneous development of PAH in the absence of hypoxia and exaggeration of PH after an hypoxic stimulus. Conversely, vessel remodeling and hypoxic PH are reduced in a 5-HT1B receptor-null mouse and are abrogated in a 5-HT2B receptor-null mouse. As a result, serotonin signaling modulates pulmonary smooth muscle function in both normal and disease states and likely contributes to disease progression of PAH. However, attempts at using selective serotonin reuptake inhibitors (SSRIs) as a therapeutic approach have yielded mixed results to date. Thus the exact contribution of this mechanism in PAH needs further clarification.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here