Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Overtraining syndrome (OTS) is among the most challenging medical disorders that confronts the sports medicine provider. OTS, although most commonly associated with endurance athletes (e.g., runners, swimmers), can also be identified in strength athletes. At present, OTS is complicated by multiple diagnostic and therapeutic challenges, as current research in this area is limited by a small number of studies and inconsistent results.
Researchers have concluded the following: there are poorly established diagnostic criteria; there are significant confounding influencers, including illness, injury, menstruation, and unique training methods for different sports; and it is difficult, if not impossible, to establish controls and/or laboratory models to study the illness.
Recent consensus statements reflect that there are currently no conclusive data on the causes, pathophysiology, early identification, and prevention of OTS.
This chapter will review the epidemiology and key terminology of this disorder and describe the proposed pathophysiology of OTS. Importantly, we will discuss current guidance on the clinical presentation, diagnosis, management, and prevention of this complex disorder.
OTS is an issue that has plagued athletes, trainers, coaches, and clinicians for generations. As evidenced by this quote from Dr. D. C. Parmenter in 1923, this ailment is not new to the medical literature:
“Overtraining or staleness is the bug-a-boo of every experienced trainer…a condition difficult to detect and still more difficult to describe…evaluation should focus on training load, nutrition, sleep and rest, competition stress and psychological state.”
The current literature on OTS has limited insight into the incidence and prevalence of this disorder. However, observational data and clinical experience suggest that OTS is not rare, with some authors postulating that the prevalence of the disorder may be increasing and spreading to nonelite athlete populations. An early study reported that 65% of elite competitive swimmers had experienced staleness at some time in their career. A subsequent survey study of endurance runners described a prevalence rate of 10% during one training cycle and a lifetime risk of 64% and 60% among male and female runners, respectively. A recent systematic review of the literature evaluating overtraining in strength athletes identified an urgent need for practical tools for diagnosis in this population.
Athletes who have experienced OTS also appear more likely to relapse: a study of college swimmers reported that 91% of swimmers who experienced OTS in their freshman year suffered a repeat episode during the subsequent year as opposed to 34% of those who did not experience an initial episode.
Training: A series of stimuli used to stress or displace homeostasis to provide stimulation for adaptation. Training involves progressive load in an effort to improve performance in a sport or activity. Training for success involves a balance between achieving peak performance and avoiding negative consequences of overtraining.
Load: Training results in a stimulus that is identified as the load. Load is further defined as external, which is the actual work completed by the athlete, and internal, which represents the individual physical, physiologic, and psychological characteristics that respond to the load. Athletes respond individually to internal and external loads.
Adaptation: Physiologic response to stress that results in an adjustment in function or dimension of an organism.
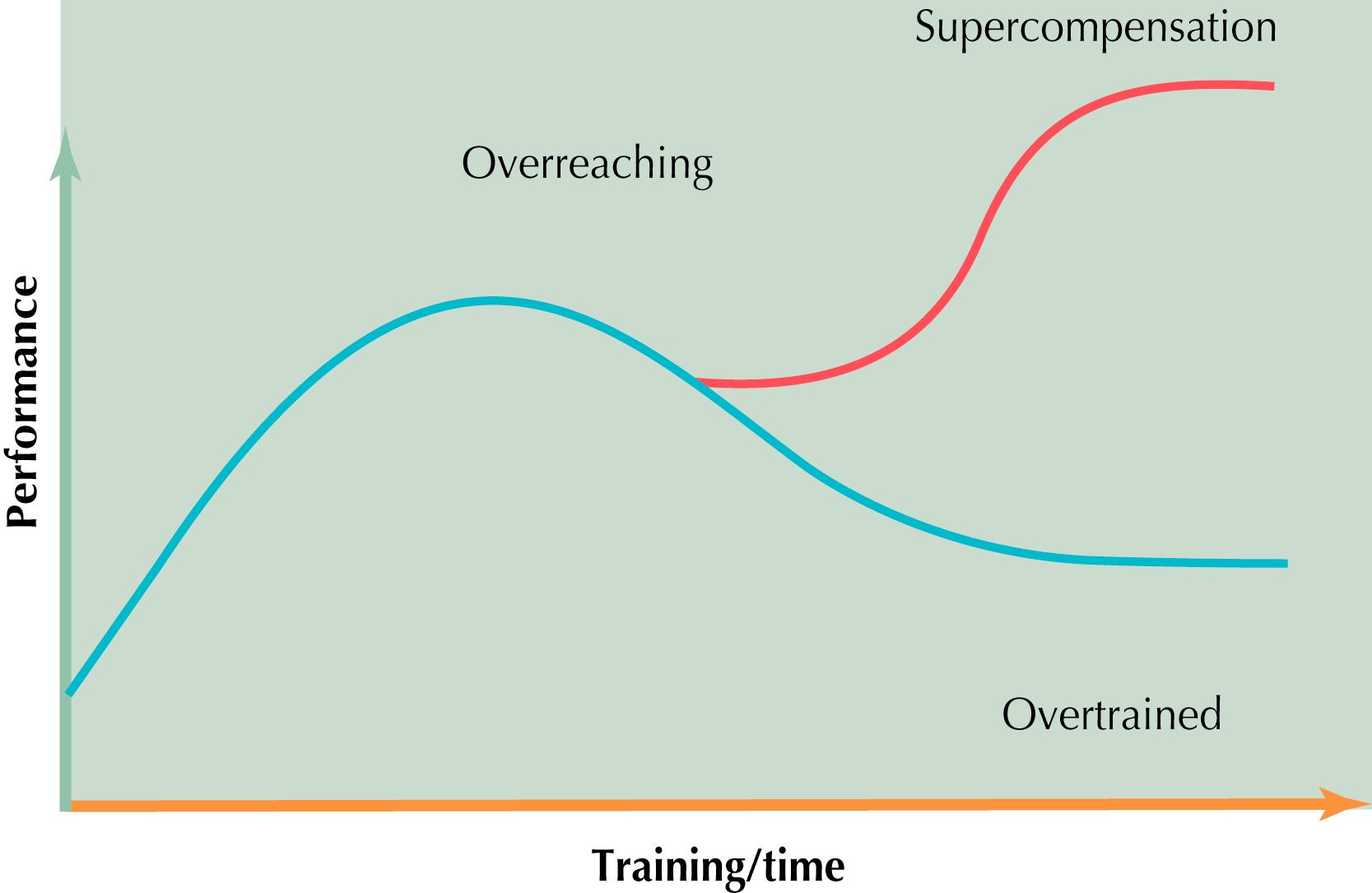
Recovery: The period after a training stimulus when work capacity returns to prestimulus levels. If recovery time is optimal, supercompensation results, whereas excessive training, without rest, can result in a decline in performance ( Fig. 28.1 ). The available literature describes four components of recovery: hydration and nutrition; sleep and rest; relaxation and emotional support; and stretching and active rest. Recovery that is inadequate results in fatigue. Fatigue may be classified as either pathologic or physiologic.
Physiologic fatigue includes categories such as insufficient sleep, nutritional, jet lag, pregnancy, and training-induced (from either excessive competition or overreaching).
Pathologic fatigue includes the following categories: medical, including infectious; neoplastic, hematologic, endocrine, toxic, iatrogenic, and psychiatric; chronic fatigue syndrome; and OTS.
Periodization: Planned sequencing of increased training loads and recovery periods within a training program.
Overload: Overload occurs when the balance between external and internal loads is dysfunctional so that the body’s adaptive response and capacity are exceeded with resultant decreased performance.
Acute fatigue (AF): The immediate response to overload training; although fatigued, the athlete experiences no perceivable decline in performance.
Recovery–fatigue continuum: Recovery and fatigue are on a continuum and jointly affected by both physiologic and psychological determinants. An imbalance of accumulated long-term fatigue and inadequate recovery create an unfavorable environment for nonfunctional overreaching, OTS, and decreased performance.
Functional overreaching (FOR): Short-term decrement in performance after a period of overload training usually lasting <2 weeks after a period of overload training.
Nonfunctional overreaching (NFOR): A longer period of performance decline (2 weeks to 2 months) after a period of overload training.
OTS: Maladaptive response to training from an extended period of overload (usually 2 months or more); the result of too severe or a prolonged period of overreaching (see Fig. 28.1 ). Overtraining is manifested by decreased sport-specific performance and enhanced fatigability, pronounced vegetative complaints, sleep disorder, emotional instability, organ-related complaints without organic disease, overuse injuries, blood chemistry changes, and immune dysfunction.
The pathophysiology of OTS has not been fully elucidated. Multiple models and hypotheses attempt to explain the signs and symptoms of this disorder, including the autonomic imbalance hypothesis, the central fatigue hypothesis, the glycogen depletion hypotheses, and the cytokine hypothesis.
Fig. 28.2 summarizes the various hypotheses to explain the complexity of this disorder.
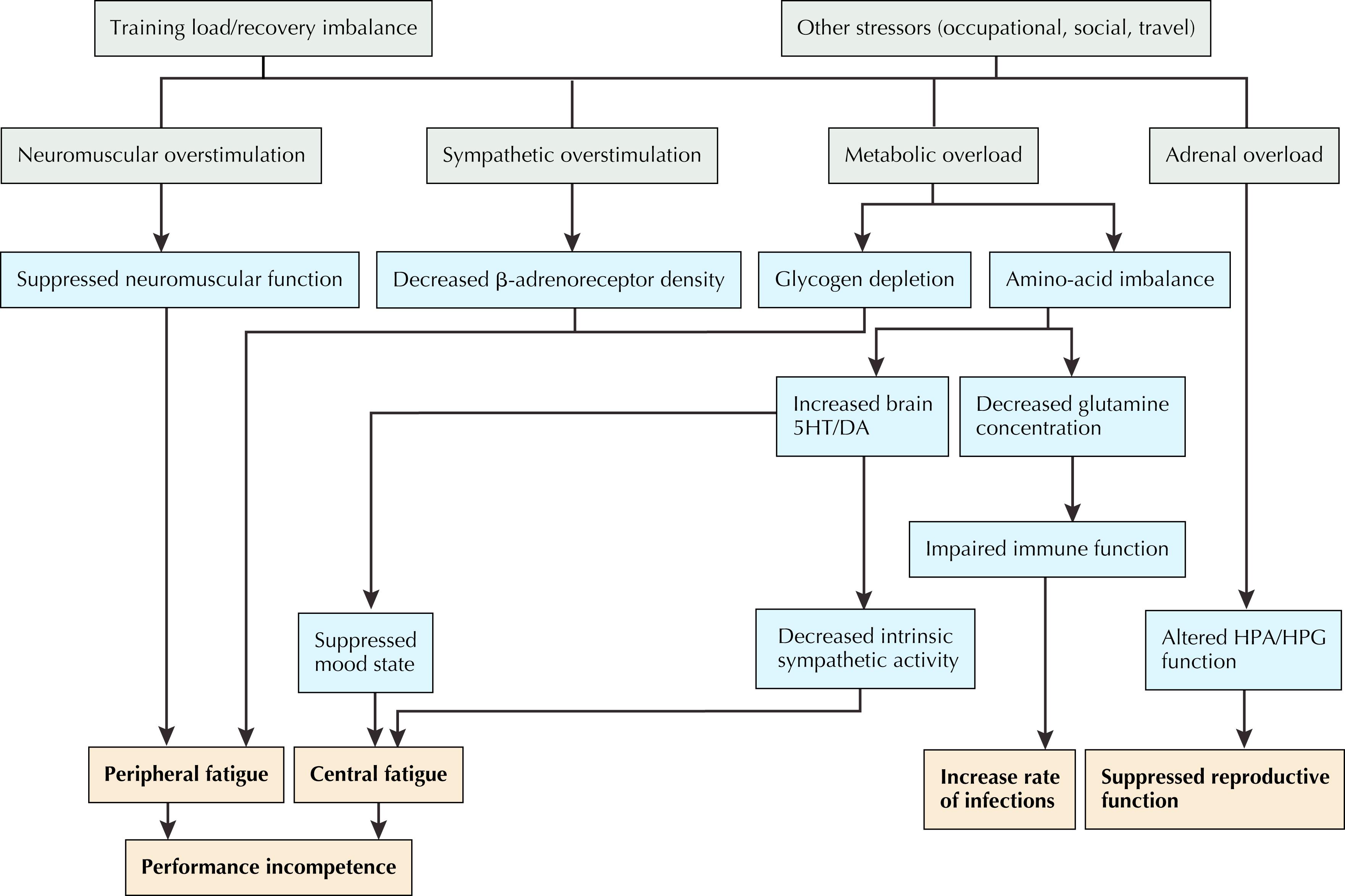
The autonomic imbalance hypothesis proposes that underlying imbalances in the autonomic nervous system cause OTS. The initial stage of this proposed mechanism involves negative feedback caused by a surge of catecholamine release during periods of heavy training. This causes a decrease in baseline catecholamine secretion. Second, an increase in metabolism during exercise causes an imbalance among plasma amino acids and alterations in brain neurotransmitter metabolism, leading to an increase in the concentrations of aromatic amino acids (phenylalanine, tryptophan, and tyrosine). The resulting increases in hypothalamic tryptophan and cerebral dopamine concentrations cause “metabolic error signals” with inhibitory effects on the sympathetic nervous system. In addition, the increase in core temperature associated with high-intensity training (HIT) may exert inhibitory effects on the sympathetic centers of the hypothalamus. Third, a neuronal negative feedback system results in down-regulation of catecholamine receptors in the exercising muscles.
The central fatigue theory hypothesizes that OTS is caused by an increase in the synthesis of 5-hydroxytryptomine (5-HT) in the central nervous system (CNS). Extensive exercise results in glycogen depletion in muscles, leading to the use of secondary energy sources by these muscles. The branched-chain amino acids (BCAAs: leucine, isoleucine, and valine) are oxidized to glucose. Concurrently, levels of fatty acids increase as well. Fatty acids compete with tryptophan for albumin-binding sites, leading to an increase in plasma tryptophan. Because both BCAAs and tryptophan use the same transporter to pass through the blood-brain barrier, a decrease in plasma BCAAs and an increase in plasma tryptophan lead to an increase in tryptophan passing through into the CNS. In the brain, tryptophan is converted into the neurotransmitter 5-HT. 5-HT is known to play a role in various neuroendocrine and emotional functions, all of which can be seen with OTS. This connection between OTS and an increase in the free tryptophan/BCAA ratio form the basis for this hypothesis.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here