Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
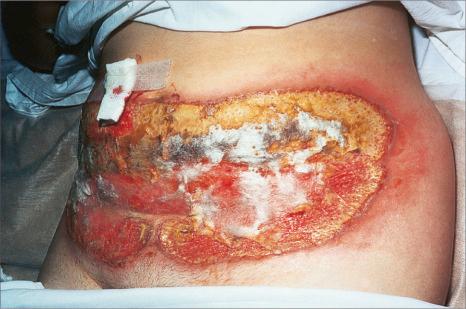
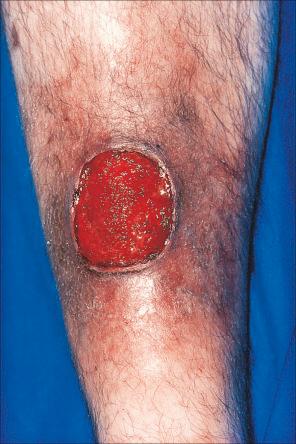
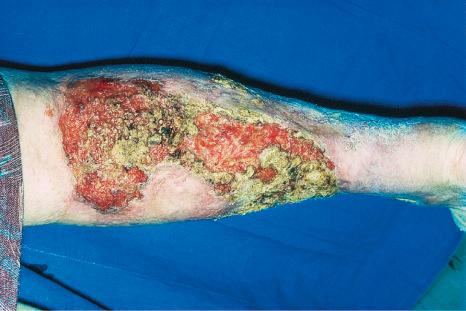
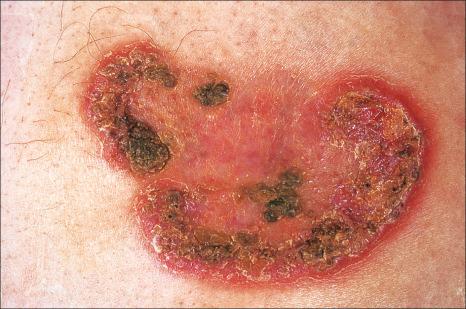
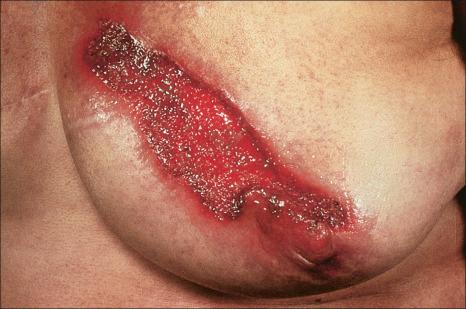
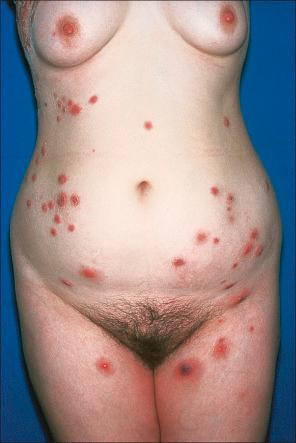
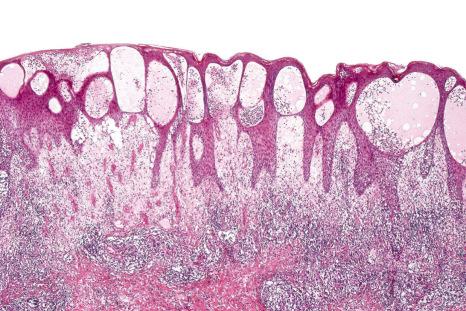
Pyoderma gangrenosum is an uncommon disease of obscure etiology. It appears to be somewhat more common in women and, although it may occur at any age, most patients are in their fourth or fifth decade. Presentation in children is uncommon, but it has been seen even in infants, and rare familial cases have been documented. The disease may also present in pregnancy, and in this setting it is associated with an underlying disease process in about 30–50% of the cases. Large, necrotic ulcers, often 10 cm or more in diameter, characterize the disease ( Fig. 15.1 ). Lesions may arise from acneiform pustules or on a background of erythematous nodules. Typically, the ulcers have undermined edges and red–purple borders ( Fig. 15.2 ). They may be solitary or multiple, and occur most often on the lower limbs, although other sites such as the trunk, face, arms, hands, and buttocks are sometimes affected ( Fig. 15.3 ). Rare sites of involvement include the oropharyngeal region, hand, eyelid, eye, vulva, penis, scrotum, and the cervix. The ulcers are painful and tender, and may persist for months or years. Complications usually result from the site of the lesion and can include cranial osteolysis, nasal perforation, and tendon rupture. Recurrent attacks are not uncommon. Cribriform scarring often follows healing. Systemic involvement has rarely been documented, affecting the lungs, liver, bone, joints, pancreas, heart, and spleen.
Occasionally, bullous or pustular variants are encountered. One large study found that bullous lesions are more common on the upper extremities, and they appear to be more frequently associated with hematological malignancy. Such lesions are sometimes designated atypical pyoderma gangrenosum. A vegetative form has also been described. Some patients have more than one clinical type concurrently.
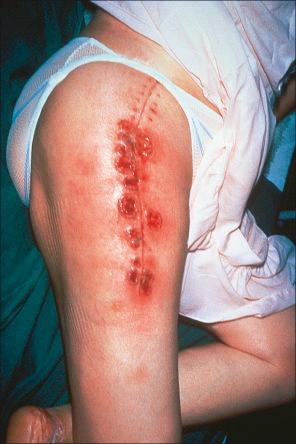
A particularly interesting feature seen in 20–50% of cases is development of lesions in traumatized areas (pathergy). Lesions may occur at sites of surgery and have been reported after cholecystectomy, breast reduction or augmentation, splenectomy, hysterectomy, cesarean section, appendectomy, cardiac surgery, orthopedic surgery, herniorrhaphy, bowel bypass procedure, excision of anal condyloma, at the site of a fasciocutaneous flap, a laparoscopic port insertion site, and in an amputation stump ( Fig. 15.4 ). In the postoperative setting, women appear to be disproportionately affected, with breast reconstruction surgery being the most common inciting incident. They also occur following rather trivial trauma such as injection or intravenous access site, arteriovenous dialysis shunt, blood-drawing, acupuncture, or a tattoo. Pressure from use of seat belts in automobiles has been associated with subsequent lesion development. Presentation has even been documented at the location of a spider bite. One case reports involvement of the scalp after receiving hair highlights at a salon, which could be due to physical and/or chemical trauma.
A variety of drugs have been implicated as potential triggers, including, alpha-2b interferon (IFN-α2b), isotretinoin, sulpiride, propylthiouracil, lenalidomide, rituximab, sunitinib, imatinib, gefitinib, pazopanib, ipilimumab, and adalimumab. Paradoxically, some of these medications (e.g., rituximab, ipilimumab, and adalimumab) have been used to treat pyoderma gangrenosum.
Pyoderma gangrenosum after combination therapy with cytosine arabinoside, aclarubicin, and granulocyte colony-stimulating factor for myelodysplastic syndrome has been reported. Pyoderma gangrenosum has also been linked to levamisole-adulterated cocaine abuse. . A granulomatous and suppurative dermatitis that may mimic pyoderma gangrenosum has been documented at the site of interferon-alpha (IFN-α) injections. Sclerotherapy has also been complicated by pyoderma gangrenosum on rare occasions. Of particular importance is the known association of pyoderma gangrenosum with a variety of conditions (in up to 50% of patients ) as outlined in Table 15.1 . Of these, inflammatory bowel disease (both Crohn disease and ulcerative colitis) and arthritis show the most well-established links. Pyoderma gangrenosum is reported to complicate around 1–2% of inflammatory bowel disease patients. In one study, 27% of patients had associated inflammatory bowel disease and 20% of patients had arthritis. In this same study, 27% of patients with superficial ‘atypical’ pyoderma gangrenosum had an associated hematological disorder. In another large study, idiopathic pyoderma gangrenosum and that associated with chronic inflammatory bowel disease were found to be more common in females, whereas pyoderma gangrenosum associated with hematological malignancy was more common in males. While pyoderma gangrenosum can fluctuate with inflammatory bowel disease activity, it may also be a presenting or heralding feature. The presence of pyoderma gangrenosum as a complication of inflammatory bowel disease does not appear to be an independent predictor of severity of the bowel disease. Although pyoderma gangrenosum lesions may improve as inflammatory bowel disease is brought under control, specific treatment is usually required. Most of the other numerous, rare associations mentioned in Table 15.1 are likely to be fortuitous, as a report of simple coexistence does not strictly imply a meaningful association. In any event, a diagnosis of pyoderma gangrenosum should always prompt an evaluation for an underlying disease association. Pyoderma gangrenosum-like lesions have been reported as the presenting feature of antiphospholipid antibody syndrome. Other underlying conditions causing lesions that mimic pyoderma gangrenosum are also well described including inflammatory and infectious processes, vasculopathies, and malignancies, stressing the importance of careful clinical investigation.
|
The disease may also occur in association with other neutrophilic dermatoses including Sweet syndrome and other dermatological diseases, such as lupus erythematosus and erythema nodosum, the latter typically in the background of concomitant inflammatory bowel disease. Pyoderma gangrenosum is one of the components of an autosomal dominant syndrome known as PAPA (pyogenic sterile arthritis, pyoderma gangrenosum and acne). This syndrome has been mapped to chromosome 15q and is associated with mutations in the gene CD2BP1 / PSTPIP1 . These mutations increase the binding affinity of this gene product to pyrin, overcoming the autoinhibition of this homotrimer and allowing activation of the downstream innate immune response. Ultimately, this mutation leads to an increase in caspase-1 activation, an underlying feature of multiple inherited autoinflammatory syndromes. These findings indicate that pyoderma gangrenosum may be best regarded as an autoinflammatory or autoimmune disease, and the pathways being studied in PAPA syndrome may also eventually shed light onto the pathogenic mechanisms of sporadic pyoderma gangrenosum. A related syndrome with hidradenitis instead of pyogenic arthritis (PASH) associated with mutations in PSTPIP1 has been described. Some patients have hidradenitis with arthritis (PAPASH). The genetics of pyoderma gangrenosum and these related syndromes is more complex than is appreciated. Cases lacking mutations in PSTPIP1 have been described, and a patient with a mutation in NCSTN , a gene implicated in hidradenitis suppurativa, has been reported. Pyoderma gangrenosum has also been associated with LAD-1 (leukocyte adhesion deficiency-1) secondary to mutation of ITGB2.
Para- and peristomal involvement in patients with ileostomy or colostomy for inflammatory bowel disease is a well-recognized phenomenon. In a large series, 13% of patients had peristomal pyoderma. Both Crohn disease and ulcerative colitis are associated with this complication. It should be noted that peristomal pyoderma gangrenosum has been seen in the absence of inflammatory bowel disease. It has been documented in patients with ostomy for gastrointestinal carcinoma and diverticular disease. Pyoderma gangrenosum may also occur at urostomy sites following cystectomy for bladder carcinoma. ,
Superficial granulomatous pyoderma is believed to represent a superficial and rare variant of pyoderma gangrenosum. However, the latter is controversial as patients with this condition usually do not have associated systemic disease and the histologic features are different with predominance of suppurative granulomas (see below). Patients develop single or sometimes multiple superficial ulcerated lesions with vegetative borders (for this reason, this variant is sometimes referred to as ‘vegetative variant of pyoderma gangrenosum’) as a consequence of trauma, frequently surgical ( Fig. 15.5 ). Pain is an occasional feature. The ulcers have a cleaner base than those seen in classic pyoderma. Lesions are most commonly found on the trunk and upper extremities, and heal with cribriform scarring ( Fig. 15.6 ). Draining sinuses are occasionally evident. Often there is no evidence of underlying systemic disease. Superficial granulomatous pyoderma is more likely to follow a chronic course compared with classic pyoderma gangrenosum. Rare cases involving the face, eye, and vulva have been reported.
So-called ‘malignant pyoderma’ is a controversial designation which we believe should be avoided. Some authors have used the term to describe a variant of pyoderma gangrenosum predominantly affecting the head and neck. It has been postulated that at least some cases of so-called malignant pyoderma more likely represent cutaneous granulomatosis with polyangiitis (cutaneous granulomatosis).
One study found that over 50% of patients with pyoderma gangrenosum required long-term therapy to control their disease. The disease may be fatal in some cases, particularly if diagnosis is delayed. In another study, 2 of the 21 patients reported died of pyoderma gangrenosum secondary to pulmonary involvement.
The precise pathogenesis of pyoderma gangrenosum is uncertain. The current state of knowledge suggests that it is due to immune dysfunction, perhaps innate, and/or that it develops on a vasculitic basis. A variety of immunological abnormalities have been described including:
absent delayed hypersensitivity reactions to common antigens such as mycobacteria and Candida albicans
defective neutrophil chemotaxis and irregular neutrophil trafficking
impaired neutrophil phagocytosis
diminished lymphokine (migration inhibition factor) production
overexpression of interleukin (IL)-8, a potent chemotactic polypeptide for neutrophils, has been reported in lesional tissue and may be an important pathogenetic factor
reduction in IL-8 and related molecules has been noted following successful therapy
overexpression of IL-17 and 23
aberrant neutrophil trafficking and metabolic integrin β2-CR3 and -CR4 oscillations in lesional tissue
elevated levels of HIF2a and downstream effectors vascular endothelial growth factor (VEGF) and Ang-2 have been noted in disseminated disease, suggesting that angiogenesis in improper control of the neutrophil oxidative burst may be involved
elevated tumor necrosis factor-alpha (TNF-α), MMP-9, and MMP-10 have also been noted
TNF-α may have some of its effects mediated by keratinocyte secretion of elafin, an elastase inhibitor. Indeed, anti-TNF-α therapy has been described to show some efficacy ; however, a case has also been described in association with TNF-α antagonists used to treat rheumatoid arthritis and the relationship may be complex.
The results of immunofluorescence studies in large series of patients have revealed both immunoglobulins (usually IgM) and complement in blood vessel walls in the dermis of the leading edge of the ulcer. Another study, however, failed to substantiate this finding, and immunofluorescence should not be considered and ancillary diagnostic test. There is no evidence to support an infective pathogenesis.
Expanding T-cell clones in both the skin and circulation have been described in a small series of patients, indicating that T-cell response plays a role in the disease and may be triggered by a local stimulus in the skin. T-cell clonality has been described in pyoderma gangrenosum in the absence of an underlying myeloproliferative disease.
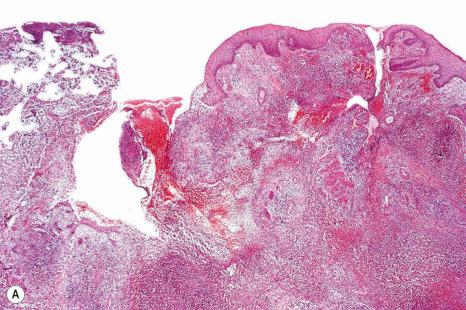
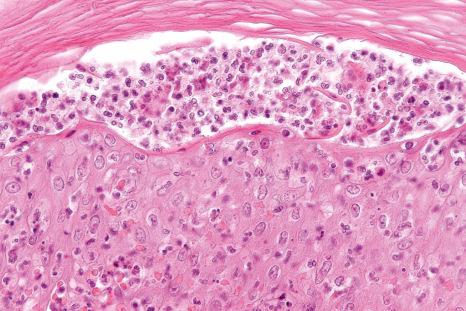
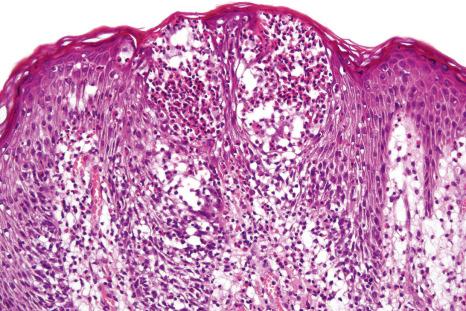
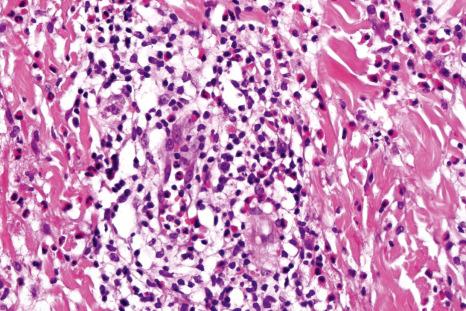
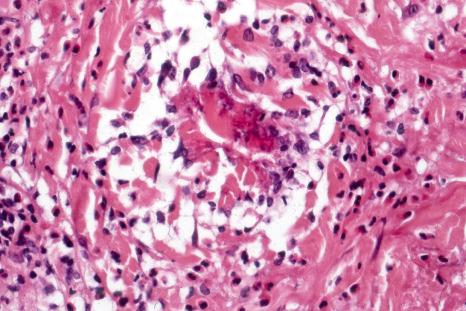
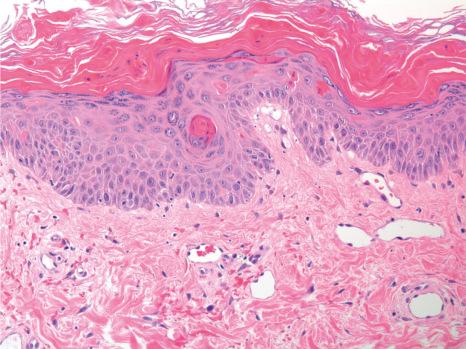
In general, the histopathology is that of non-specific ulceration with abscess formation ( Fig. 15.7 ). The adjacent dermis shows acute and chronic inflammation. A pseudo-Pelger-Huet phenomenon with hyposegmented neutrophils making recognition difficult has been described in one patient. Early lesions may present with subcorneal pustulation ( Fig. 15.8 ). Although the histologic features of both leukocytoclastic and lymphocyte-mediated vasculitis have been described, it is our experience that any vasculitis present is usually located within the floor of the ulcer or in the immediate adjacent tissues and is, therefore, more likely to be a consequence, rather than a cause, of the lesion ( Fig. 15.9 ). It has been suggested by some that some lesions of pyoderma gangrenosum may be initiated by acute folliculitis.
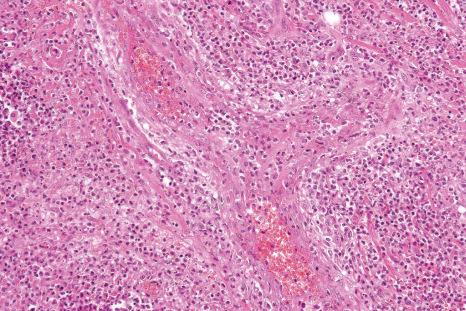
Giant cells appear to be a common feature of pyoderma gangrenosum in patients with Crohn disease. In one study, they were present in 6 of 13 patients with associated inflammatory bowel disease; of these, 5 had Crohn disease and 1 had ulcerative colitis. Giant cells were not found in any biopsies from 22 patients without associated inflammatory bowel disease.
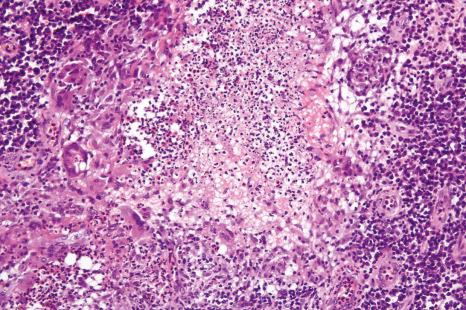
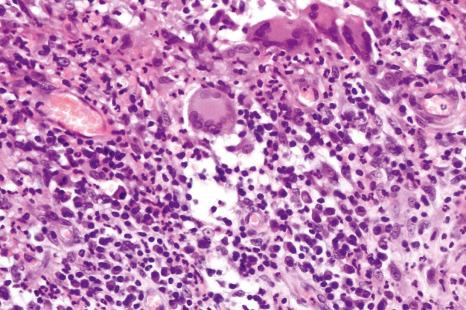
Superficial granulomatous pyoderma is characterized by a zoned inflammatory infiltrate in the superficial dermis. Focal and sterile abscesses are surrounded by a zone of granulomatous inflammation, mainly suppurative granulomas, bordered by a rim of lymphocytes and plasma cells ( Figs 15.10–15.12 ). Hemorrhage is often present and eosinophils may be evident. Any vasculitic change is thought to be secondary. The adjacent tissues may show scarring. Acanthosis and pseudoepitheliomatous hyperplasia predominantly, but not exclusively of the infundibular portion of hair follicles are frequently noted. Foreign material including starch, sutures, vegetable matter, wood, and hair has been identified in a large proportion of these cases. It should be noted that not all cases of pyoderma gangrenosum with granulomatous inflammation are limited to the superficial dermis. Some cases show involvement of the deep dermis and even subcutaneous tissue.
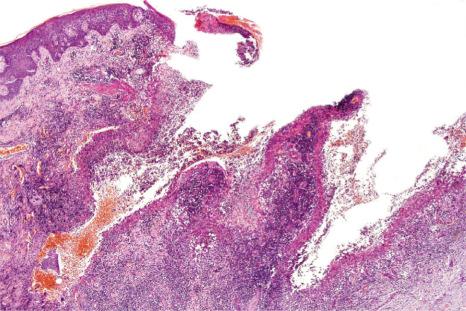
The histopathological findings in pyoderma gangrenosum are non-specific, and the diagnosis is primarily one of exclusion. Since surgery is used to manage some of the disorders considered in the histologic and clinical differential diagnosis – but is contraindicated in the treatment of pyoderma gangrenosum – early and accurate diagnosis is critical. Surgery, which tends to exacerbate the disease, is generally contraindicated in pyoderma cases because of the pathergic response. The mainstay of therapy is medical management, such as corticosteroids and more recently targeted therapies. Unfortunately, patients with pyoderma are often misdiagnosed early in the course of their disease, and the diagnosis is sometimes made only after multiple unsuccessful (and damaging) surgeries have been performed. In one study, an average of five physicians had examined the patient before a correct diagnosis was rendered. To avoid this error, obtaining accurate clinical information on wounds and debridement specimens is essential.
Culture is required to exclude infection (bacterial, mycobacterial, fungal). Necrotizing fasciitis tends to affect deeper fascial and subcutaneous tissue, while pyoderma is centered in the dermis (albeit some spillover into the subcutis may be seen). Usually, sheets of bacteria are evident in untreated necrotizing fasciitis. Distinguishing these two conditions is critical since the treatments are diametrical opposites with surgery and antibiotics for necrotizing fasciitis and avoidance of surgery with systemic anti-immune treatment and supportive wound care for pyoderma gangrenosum.
Sweet syndrome is generally not associated with ulceration and shows more prominent karyorrhexis relative to the number of neutrophils, and the inflammatory cell infiltrate tends to be restricted to the dermis. Bite reactions, particularly resulting from the brown recluse or other spiders, may show similar histologic features, and eosinophils may not be a prominent feature in early lesions of bites. Clinical information is necessary to distinguish pyoderma from many other forms of ulcer such as those due to trauma.
Although some authors have noted lymphocytic or neutrophilic vasculitis in lesions of pyoderma gangrenosum, this finding, in our experience, is limited to areas adjacent to the ulcer and likely represents a secondary finding. Indeed, it has been our experience that ‘secondary’ vasculitis is frequently present at the border of ulcers of many different etiologies in patients without any genuine underlying ‘primary’ vasculitic process. Evaluation for vasculitis as a cause of ulceration, therefore, depends upon examination of blood vessels in areas of dermis and subcutaneous tissue away from the ulcer.
It cannot be overemphasized how important accurate clinical information is in establishing the correct diagnosis. Failing to recognize this disease early in its course can be disastrous for the patient.
Acute febrile neutrophilic dermatosis (Sweet syndrome) is an uncommon disease of unknown etiology and pathogenesis. It is associated with a marked female predilection (5 : 1), and most patients affected are in their third through sixth decades. It may, however, occasionally be seen in children, and a few cases presenting in infancy have been documented. Infant brothers who both had Sweet syndrome have been reported. Patients present with variable numbers of asymmetrically distributed, frequently bilateral, circumscribed, tender, and painful red plaques or nodules, particularly on the face, neck, and upper and lower limbs ( Figs 15.13–15.15 ). An acral form of this condition is now termed neurophilic (or pustular) dermatosis of the dorsal hands ( Fig. 15.16 ). Whether this represents a distinct disease or a peculiarly localized variant of Sweet syndrome is uncertain.
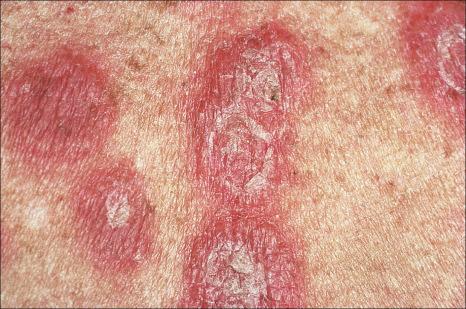
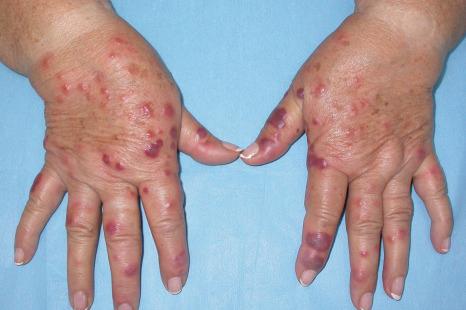
Occasionally, the lesions may become bullous or pustular. The plaques vary from about 1 to 4 cm in diameter and typically heal without scarring. Recurrences develop in approximately one-third of patients and postinflammatory hyperpigmentation is sometimes seen. Pathergy and koebnerization are occasional features, and necrosis with ulceration may rarely be encountered. Sweet syndrome may present with lesions mimicking palmoplantar pustulosis and sometimes erythema nodosum-like lesions are present. A Sweet syndrome-like eruption has been described in association with exposure to light.
Sweet syndrome often follows an upper respiratory tract infection. In some cases, it is a complication of drug treatment, for example, carbamazepine, furosemide, hydralazine, co-trimoxazole, abacavir, azathioprine, ofloxacin, doxycycline, clindamycin, minocycline, trimethoprim–sulfamethoxazole, bortezomib, lenalidomide, imatinib mesylate, nilotinib, etanercept, granulocyte colony-stimulating factor (G-CSF), radiocontrast agent, some vaccines, oral contraceptives, all- trans -retinoic acid, isotretinoin, nitrofurantoin, diazepam, clozapine, celecoxib, ketoconazole, azacitidine, omeprazole, mitoxantrone, vemurafenib, azathioprine, ipilimumab, and interferon (IFN). The temporal relationship with administration, development of symptoms, and resolution with withdrawal of the offending drug establishes the cause in drug-induced cases. The disease has also been reported after chemotherapy in patients with acute myeloid leukemia. Sweet syndrome can be broadly reviewed as falling into three general categories:
classic (and often idiopathic),
malignancy-associated (paraneoplastic),
drug-induced.
Patients may also have conjunctivitis, episcleritis, iritis, polyneuropathy, oral involvement (superficial ulcers), and arthralgias. The larger joints are usually affected, and involvement tends to be migratory. Patients with concurrent Sweet syndrome and erythema nodosum have been described, and it is possible that these two disorders share common pathogenetic mechanisms. Dyssynchronous and synchronous Sweet syndrome and erythema nodosum may occur.
Sweet syndrome is of particular importance since 10% to 40% of cases are associated with hematological malignancy such as leukemia (monocytic or myelomonocytic, including leukemia cutis), myelodysplasia, lymphoma, and multiple myeloma. Development of the disease may herald a relapse of the leukemia or precede it. Sweet syndrome has also been reported in patients with monoclonal gammopathy and myelodysplasia in the absence of frank leukemia or lymphoma. Hemophagocytic syndrome is also a reported association. The clinical lesions of Sweet syndrome are said to be more severe in patients with underlying hematological disease. An association with urticaria pigmentosa has also been documented.
Solid tumors may also be associated with Sweet syndrome in up to 7% of patients, including:
testicular,
bladder,
gastrointestinal,
breast,
lung,
ovary,
prostate,
gallbladder,
thyroid,
oral squamous cell carcinoma.
A rare case following treatment of herpes simplex in a patient with metastatic breast carcinoma and another associated with post-mastectomy lymphedema have been reported. Sweet syndrome has been described in conjunction with numerous conditions, some of which are listed in Table 15.2 . While its association with hematological and internal malignancies, upper respiratory tract infections, drugs, and certain inflammatory disorders such as erythema nodosum, rheumatoid arthritis, and sarcoidosis appears repeatedly, many of the others listed in the literature could be coincidental.
|
Systemic involvement may be a feature of Sweet syndrome with lesions described in the eye, lung, kidney, central nervous system, vagina, liver, gastrointestinal tract, and skeletal muscle. Neural involvement appears to be strongly associated with human leukocyte antigen (HLA)-Cw1. An exceptional case with gingival hyperplasia and myositis in the absence of cutaneous involvement has been documented.
Associated features include pyrexia, neutrophilia, and a raised erythrocyte sedimentation rate (ESR). Patients with antineutrophil cytoplasmic antibodies (ANCA) have been reported, and this finding may be more common with Sweet syndrome localized to the dorsal hands. The presence of ANCA, however, is not a consistent finding.
The etiology of Sweet syndrome is unknown; however, the disease most probably represents an unusual hypersensitivity reaction secondary to cytokine production. It is likely that neutrophils are activated by IL-1 and that Sweet syndrome represents a cytokine-mediated inflammatory reaction to a wide variety of different antigens including bacteria, viruses, drugs, and malignancies. Demonstration of elevated serum IL-1α, IL-1β, IL-2, and interferon-gamma (IFN-γ), but not IL-4, suggests that type 1 (but not type 2) helper T cells (Th) play a role in the pathogenesis. Not surprisingly, since exogenous treatment with G-CSF is associated with Sweet syndrome, endogenous G-CSF has been shown to be elevated in some cases.
In patients with G-CSF-associated Sweet syndrome, it has been suggested that the condition represents a form of neutrophilic recovery syndrome. The occasional presence of immune complexes in blood vessel walls may have pathogenetic significance.
Clonality in the skin infiltrate of a patient with Sweet syndrome and acute myelogenous leukemia undergoing treatment with G-CSF has been demonstrated, suggesting that the infiltrate may be the result of therapy-induced differentiation of neoplastic cells. However, a further demonstrating clonality in four patients in the absence of myeloproliferative disease argues against that theory.
Histologically, the epidermis in Sweet syndrome is usually unaffected although occasionally slight spongiosis is present; rarely, vesiculation, spongiform pustules, and necrotic keratinocytes have been described. The cardinal feature, however, is an intense neutrophil polymorph infiltrate within the reticular dermis ( Fig. 15.17 ). This may be diffuse or perivascular in distribution and often surrounds the sweat ducts. Typically, leukocytoclasis is marked ( Fig. 15.18 ). Admixed with the neutrophil polymorphs are variable numbers of lymphocytes, and histiocytes. Eosinophils are exceptional and when seen tend to be sparse. Ingestion of nuclear debris by histiocytes is sometimes a conspicuous feature. Rarely, degenerating neutrophils can resemble Cryptococcus. A histiocytic/histiocytoid form of the disease has increasingly been recognized. In this variant, the infiltrate is composed of mononuclear cells with lightly eosinophilic cytoplasm resembling histiocytes ( Fig. 15.19 ). This is more likely to represent a stage in the evolution of the disease rather than a specific variant of Sweet syndrome. It has been postulated that the histiocyte-like cells seen represent immature granulocytes based on immunoreactivity for myeloperoxidase in addition to histiocytic markers in most of the cells. Cells are positive for CD15, CD45, CD43, CD68, MAC-386, HAM56, lysozyme, and myeloperoxidase CD33. Awareness of this form of presentation is important to avoid a misdiagnosis. Exceptionally, cells in histiocytoid Sweet appear haloed mimicking a cryptococcal infection. Given the presence of a mononuclear cell infiltrate in these cases, it is extremely important to exclude leukemia cutis. Special stains and clinicopathological correlation are therefore paramount.
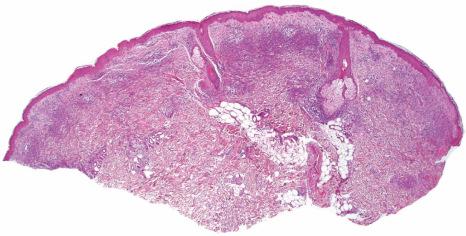
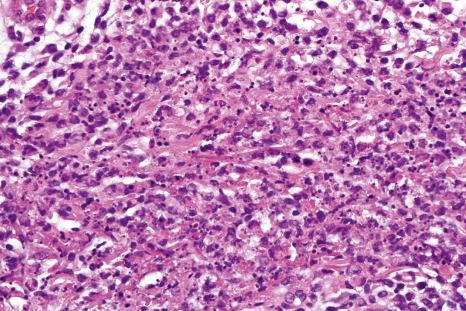
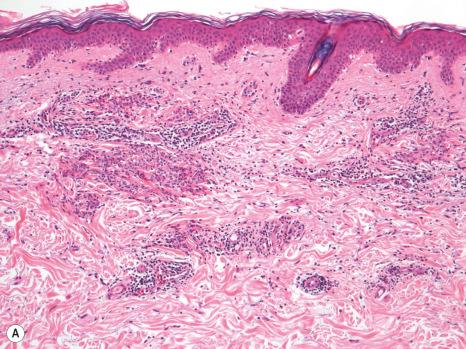
Often, the papillary dermis shows very marked edema, which sometimes results in subepidermal vesiculation ( Fig. 15.20 ). Rarely, the presence of dermal papillary neutrophil microabscesses may cause diagnostic confusion with dermatitis herpetiformis ( Fig. 15.21 ). In Sweet syndrome, the blood vessels are dilated and may show endothelial swelling but changes of frank vasculitis are generally absent in our experience (and certainly not prominent). However, others have reported features of vasculitis such as nuclear dust, extravasation of erythrocytes, and fibrin deposition in and around vessels walls, and thus argue that the presence of vasculitis should not exclude this diagnosis. Purpura is sometimes evident. Immunofluorescence examination of skin biopsies in Sweet syndrome is usually negative for immunoreactants in the walls of the vasculature.
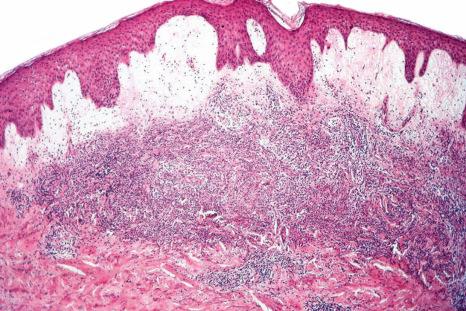
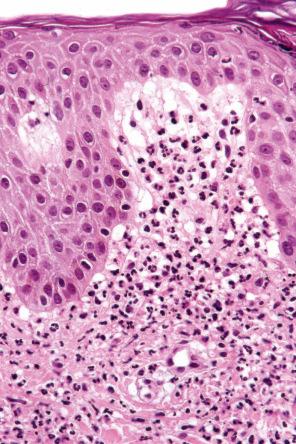
Cases associated with leukocytoclastic neutrophilic lobular panniculitis, have been reported, and this may represent subcutaneous Sweet syndrome. In other cases, the infiltrate may be predominantly composed of lymphocytes and histiocytes and, less commonly, neutrophils. Sweet syndrome has also been associated with an erythema nodosum-like panniculitis. Recently, cases with widespread cellulitis-like erythematous plaques have been described, termed giant cellulitis-like Sweet syndrome. This form can be either neutrophilic or histiocytoid. Elastophagocytosis and cutis laxa have been reported with resolution of Sweet syndrome lesions.
The presence of prominent fibrinoid vascular change can distinguish necrotizing vasculidities such as leukocytoclastic vasculitis, erythema elevatum diutinum, and granuloma faciale from Sweet syndrome; the clinical presentation and distribution of disease are also extremely helpful. In granuloma faciale, fibrinoid necrosis is often minimal and eosinophils tend to be prominent. Late lesions of erythema elevatum diutinum and granuloma faciale show fibrosis, a feature not seen in Sweet syndrome. Clinically, the presence of characteristic large ulcers helps distinguish pyoderma gangrenosum from Sweet syndrome. Also, pyoderma gangrenosum does not usually show the extent of karyorrhexis that is a typical feature of Sweet syndrome. A Gram stain and periodic acid-Schiff (PAS) or culture may be necessary to exclude infection. Distinction from some other forms of neutrophilic dermatosis including bowel bypass syndrome may be a definitional issue since the clinical setting determines the terminology applied. Behçet disease may also be associated with lesions similar to those seen in Sweet syndrome. Clinical correlation should ensure the correct diagnosis. CD30-positive forms can sometimes be found in Sweet syndrome, raising the possibility of lymphomatoid papulosis. However, neutrophils are usually rare in the latter condition and the number of CD30-positive cells in Sweet syndrome is not prominent. Knowledge of coexisting rheumatoid arthritis or systemic lupus eyrthematosus helps distinguish Sweet syndrome from rheumatoid neutrophilic dermatosis and systemic lupus erythematosus (SLE)-associated neutrophilic dermatosis, respectively. Although it has been suggested that in the later the dermal infiltrate tends to be paucicellular in contrast with the heavier infiltrate seen in Sweet syndrome, in fact moderate to prominent dermal neutrophilic infiltrates are more commonly seen in lupus. Therefore, distinction from Sweet syndrome is impossible without clinicopathological correlation.
Pyoderma gangrenosum, the most common neutrophilic dermatosis affecting patients with gastrointestinal disease (particularly ulcerative colitis), is discussed above. The spectrum of lesions described in this section shares many histologic (and likely pathogenetic) features with pyoderma gangrenosum but lack the characteristic progressive ulceration. Neutrophilic dermatoses associated with gastrointestinal disease may best be regarded as a continuum, with pyoderma gangrenosum representing an extreme end of the spectrum.
A syndrome of arthritis and pustular skin lesions was initially described in patients with inflammatory bowel and liver disease, and also in patients who have undergone jejunoileal bypass, gastric bypass, or Billroth II surgery for morbid obesity, but now has been described in other gastrointestinal disorders including Crohn disease and ulcerative colitis. Up to 20% of patients with jejunoileal bypass develop this condition. It has also been noted in association with peptic ulceration, appendicitis, and diverticular disease. An increasing number of papers call this process bowel-associated dermatosis-arthritis syndrome (BADAS); this terminology currently appears to be that preferred by the majority of authors.
The skin lesions may be papular or vesicular, or form large necrotic lesions resembling pyoderma gangrenosum. They are usually found on the trunk or extremities. Oral involvement has also been described. Associated panniculitis, which may resemble erythema nodosum, is a feature in some patients. Cutaneous manifestations often recur with exacerbation of the associated gastrointestinal disease. Some patients have an elevated ESR. The disease occasionally responds to antibiotic or steroid therapy.
A recurring vesiculopustular eruption may be seen in patients with hepatobiliary disease. The lesions – which can be pruritic and sometimes heal with an atrophic scar – often present on the extremities. In some patients, the eruption represents a necrotizing folliculitis. Occasionally, the cutaneous lesions precede the features of the hepatobiliary disease. A similar eruption may rarely be seen in Crohn disease.
Patients with Crohn disease can also be complicated by disseminated abscesses involving the spleen, lymph nodes, liver, pancreas, and brain. In some of these, the abscesses occurred before the diagnosis of Crohn disease. Histologically, a granulomatous element was commonly present. Successful treatment with immunosuppressive therapy suggests that such lesions may represent an unusual extraintestinal manifestation of Crohn disease.
An unusual presentation of aseptic pustulosis largely restricted to skin folds has been described in patients with inflammatory bowel disease. This seems to be a paradoxical reaction to TNF-α blockers.
The description of these entities suggests that they are overlapping or perhaps represent a disease continuum. BADAS is the most rigorously defined among these, and this terminology can probably be employed for all of the conditions mentioned above.
The presence of circulating immune complexes in occasional patients has led some authors to postulate a pathogenic role. It is postulated that bacterial overgrowth may play a role in the development of such circulating immune complexes. In patients with the paradoxical reaction to TNF-α blockers, the lesions had increased expression of IL-1, TNF-α, IL-17, IL-8 and matrix metalloproteinases. These observations are consistent with the concept that BADAS is an autoinflammatory disease similar to other neutrophilic dermatoses.
The histopathological findings, which are non-specific, are those of a neutrophilic dermatosis. The lesions show variable dermal edema and necrosis associated with a perivascular and interstitial neutrophilic infiltrate. Variable numbers of lymphocytes and histiocytes may also be present. Abundant karyorrhexis gives rise to a histologic pattern similar to acute febrile neutrophilic dermatosis (Sweet syndrome) ( Fig. 15.22 ). Leukocytoclastic vasculitis and pustular vasculitis have also been documented. The inflammation is often limited to the dermis, but in some patients it may be seen to involve the subcutaneous fat, resulting in erythema nodosum or an erythema nodosum-like panniculitis.
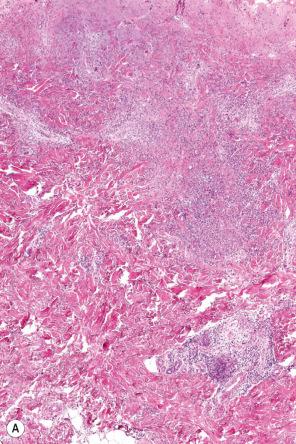
The small number of cases described in patients with hepatobiliary disease has shown bullae associated with a dermal neutrophilic infiltrate, sometimes accompanied by eccrine hidradenitis or folliculitis.
The main differential diagnoses include infection, Sweet syndrome, pyoderma gangrenosum, and rheumatoid neutrophilic dermatitis. Clinical history is essential to distinguish these conditions.
The literature relating to BADAS and Sweet syndrome is often confusing, and it seems likely that some patients who have been reported as the former would actually have been better classified as the latter. Contrariwise, occasional patients who presented with features more typical of BADAS have, in fact, been reported as Sweet syndrome. In many patients, such a distinction is semantic. In others, however, the clinical lesions are quite inconsistent with Sweet syndrome and in these patients a designation of BADAS is probably more appropriate.
Pyoderma gangrenosum is another neutrophilic dermatosis which patients with gastrointestinal disease are at risk of developing. Clinically, it may be distinguished by the progressive expansile nature of the cutaneous ulcers. Since the biopsy findings may be similar, clinical correlation is essential to distinguish this condition from BADAS.
It is likely, given the histologic and clinical spectrum encountered in the neutrophilic dermatoses associated with gastrointestinal and hepatobiliary disease, that they result from similar or shared pathogenetic mechanisms. Clearly, more research may clarify their precise pathogenesis and contribute to a more satisfactory classification system.
Rheumatoid neutrophilic dermatitis is an uncommon eruption seen in patients with rheumatoid arthritis. It presents most often as papules, nodules, and plaques on the extensor surfaces of the extremities, neck, and trunk. In some patients, it may clinically resemble urticaria. Bullous and pustular lesions have also been described. The lesions, which can ulcerate, are often pruritic or painful, and sometimes show an annular configuration. The disease is uncommon, as evidenced by documentation in just two of 142 and two of 215 patients with rheumatoid arthritis seeking medical attention for skin disorders in academic clinics in Japan and Turkey, respectively. The presence of rheumatoid neutrophilic dermatitis correlates with the severity of the patient's joint disease.
Typically, lesions last for up to several weeks. In some patients, the condition resolves spontaneously; in others, it responds to steroid, dapsone, or sulfamethoxypyridamine therapy.
Patients with seronegative arthritis but with cutaneous findings similar to rheumatoid neutrophilic dermatitis have recently been reported.
Magro and Crowson have described sterile neutrophilic folliculitis associated with a Sweet syndrome-like histology in a setting of systemic disease including rheumatoid arthritis, Crohn disease, connective tissue disease, hepatitis, Behçet disease, atopy, hematological dyscrasia, and mycobacterial infection. A similar folliculocentric acute inflammatory process has also been documented in patients with ulcerative colitis. It would seem probable that these reports reflect a similar condition or spectrum of disease that likely shares common histopathogenetic mechanisms.
The pathogenesis of rheumatoid neutrophilic dermatitis is not well understood, but some authors have suggested that it may represent an immune complex-mediated disease. Likely, it is related to autoinflammatory disease related to a combination of IL-1, TNF-α and other cytokines similar to other neutrophilic dermatoses.
Histologically, it is characterized by a dermal neutrophilic infiltrate with variable karyorrhexis ( Fig. 15.23 ). In some cases, however, karyorrhexis is minimal or absent. Variable numbers of histiocytes, plasma cells, and eosinophils may be present; abscess formation is sometimes a feature. Occasionally, the inflammatory infiltrate extends into the subcutaneous fat. The overlying epidermis may show spongiosis and intraepidermal vesiculation ( Fig. 15.24 ).
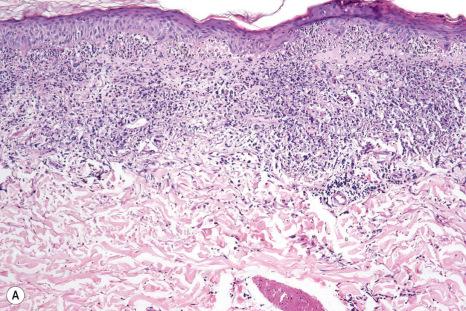
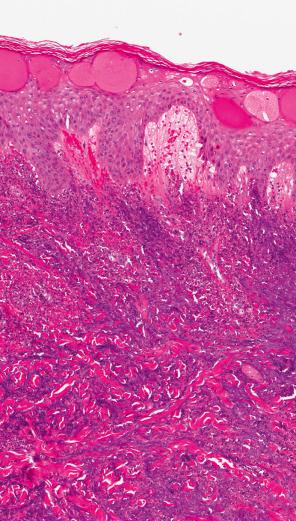
Infection must be considered in the differential diagnosis, particularly as patients are often at risk of infection as a result of immunosuppressive therapy. Furthermore, the cutaneous eruption may be treated with steroids, and failure to diagnose an underlying infective process could have disastrous consequences. Gram, AFB/acid fast, and silver stains for microorganisms should be routinely performed and the diagnosis made only after infection has been excluded. We have encountered several patients with rheumatoid arthritis on steroid therapy who developed pustular infiltrates associated with Mycobacterium chelonae infection.
Pyoderma gangrenosum may show similar, if not identical, features but differs by progressive ulceration. It should be remembered that patients with rheumatoid arthritis may also develop pyoderma gangrenosum. Clinical correlation is necessary to distinguish these entities. Pyoderma gangrenosum may form part of a continuum that may eventually prove to share similar pathogenetic mechanisms. To those who hold this view, documentation of a patient with concurrent typical features of both pyoderma gangrenosum and rheumatoid neutrophilic dermatitis should not be surprising.
Some authors have pointed out that rheumatoid neutrophilic dermatitis might be classified as a variant of Sweet syndrome. Certainly, the biopsy findings may be very similar. The lack of fever and the general malaise that accompany Sweet syndrome are distinguishing clinical findings. The presence of gastrointestinal disease distinguishes rheumatoid neutrophilic dermatitis from BADAS. As with pyoderma gangrenosum, one might consider Sweet syndrome and rheumatoid neutrophilic dermatitis to form a spectrum of disease. It is the characteristic clinical settings that allow these disorders to be distinguished.
Patients with rheumatoid arthritis may sometimes develop lesions which show histologic overlap with rheumatoid neutrophilic dermatitis but which can be distinguished by the presence of a palisading necrobiotic and granulomatous component (termed palisaded neutrophilic granulomatous dermatitis). This spectrum also includes interstitial granulomatous dermatitis encountered in a setting of systemic disease (including rheumatoid arthritis). Patients, predominantly adults, present with papules and nodules which particularly affect the extremities or trunk; these are often distributed in a linear pattern. The presence of necrobiosis associated with a histiocytic response reminiscent of granuloma annulare or necrobiosis lipoidica in addition to acute inflammation and variable karyorrhexis helps distinguish these lesions from typical rheumatoid neutrophilic dermatitis. A case has been described in a patient with rheumatoid arthritis treated with adalimumab.
Lesions in which the neutrophilic infiltrate is associated with dermal papillary abscess formation may be mistaken for dermatitis herpetiformis, linear IgA disease, and bullous SLE. IMF staining may be necessary in problematic cases.
The presence of vascular necrosis and fibrinoid change distinguishes rheumatoid neutrophilic dermatitis from vasculitis. It must be emphasized that a careful search for evidence of vasculitis is not simply an academic exercise, since patients with rheumatoid arthritis are also at risk of developing vasculitis. In fact, patients with rheumatoid arthritis may present with lesions histologically showing extravascular palisading granulomas, diffuse neutrophilic infiltrates, or vasculitis (neutrophilic, lymphocytic, or granulomatous). The different patterns may overlap, and classification should be based on the dominant histologic pattern.
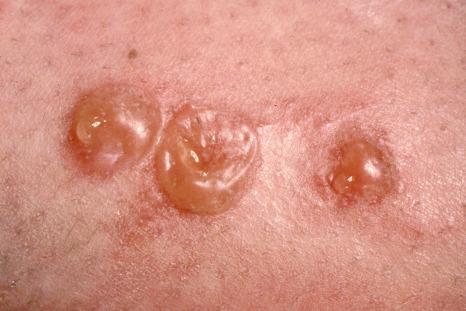
The vast majority of insect bites pose little more than a minor annoyance. The reaction that results from a given bite depends on the nature of the offending insect and the patient's immune response. The clinical response to a bite may vary from a trivial erythematous papule to a large nodule associated with marked pruritus and ulceration. Vesicles are sometimes seen in severe reactions ( Fig. 15.25 ). Careful inspection will often reveal a punctum at the site where insect mouth parts entered skin.
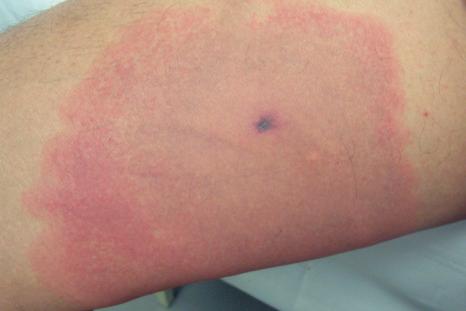
While arthropod bites are rarely of clinical importance, reactions following the bite of certain arachnids can lead to a more serious clinical lesion ( Fig. 15.26 ). Many different species of spiders may bite humans, and reactions to the most significant and well described – the brown recluse and the black widow – are detailed below.
The brown recluse spider ( Loxosceles reclusa ) bite begins as a painful bluish macule, papule, or nodule, often with a bruise-like appearance. A central punctum is commonly observed. The thigh was the involved site in almost 50% of cases, with the arm and abdomen accounting for most of the remainder in a large series from a single center of more than 50 patients with presumed bites. However, in some patients, blistering and ulceration, often progressing to a large necrotic lesion, is a feature. The lesion is often trivial. Chronic ulceration mimicking pyoderma gangrenosum may rarely ensue. The brown recluse is most commonly encountered in rural areas of the Midwest, south-central, and southeastern United States and is easily identified by a violin-shaped marking on the cephalothorax that gives it its vernacular name of ‘fiddleback’ spider. Most bites are seasonal, occurring between the months of April and October. However, other spiders are often misidentified as brown recluse, and the diagnosis may be overused as the spider is often not identified at the time of the bite. This makes much of the existing literature suspect.
Phospholipase D/sphingomyelinase-D in the venom of the brown recluse spider is thought to be responsible for the extensive necrosis that results in some patients. Spider bites may be associated with morbilliform rash, malaise, fever, nausea, hemoglobinuria, arthralgias, and vomiting. More serious complications (e.g., renal failure, shock, disseminated intravascular coagulation, acute hemolytic anemia, intravascular hemolysis, and a single case of bilateral optic neuropathy) have also been described. Many of the effects of the venom appear to be dose-dependent rather than idiosyncratic. ELISA-based assays to detect the Loxosceles venom at the site of the bite are available and can be helpful to confirm the diagnosis, as detectable toxin may persist for more than 2 weeks. Anti-loxoscelic sera are available for use in severe cases.
The five species of widow spiders found in the United States, including the notorious black widow ( Latrodectus mactans ), are most commonly encountered in the southern states. Compared with the brown recluse, bites by widow spiders are much less commonly encountered by healthcare providers. Many presumed or self-reported arachnid bites are ultimately discovered to be skin and soft tissue infections. The bite often shows a targetoid appearance with a pale center surrounded by an outer erythematous rim. A bite from a black widow spider is commonly associated with severe pain in the vicinity of the bite as well as systemic symptoms such as general malaise, abdominal pain, nausea, headache, and muscle spasms. Priapism has been noted as a rare complication. Occasionally, patients die as a result of the bite.
Alpha-latrotoxin is an active component of the venom that binds to presynaptic nerve terminals and stimulates massive neurotransmitter release. The neurological symptoms are termed latrodectism and consist of pain, diaphoresis, and non-specific systemic symptoms sometimes combined with additional autonomic or neurological dysfunction. Equine-derived antisera is available and effective as a treatment. Recombinant antisera are under development.
Recently, the Hobo spider ( Tegenaria agrestis ) has been implicated as a cause of significant bite reactions in the Pacific Northwest with migration to Montana and Colorado and evidence of continuing eastward expansion. While bites from this spider are believed to cause dermonecrotic injuries, additional studies are necessary to confirm this impression, as not all confirmed bites from this spider result in significant tissue necrosis.
Just as there is a spectrum of clinical response to an insect bite, the histopathological features also vary.
The typical arthropod bite reaction, such as follows a mosquito bite, is characterized by a wedge-shaped polymorphic inflammatory cell infiltrate composed of lymphocytes, histiocytes, eosinophils, and sometimes neutrophils ( Figs 15.27 and 15.28 ). Spongiosis (occasionally with vesicle formation) and dermal edema are variably seen ( Figs 15.29–15.32 ), but in many cases the epidermis can appear relatively unremarkable. Ulceration with scale-crust commonly forms in excoriated lesions. In some cases, insect mouth parts are identified in the center of the lesion. In our experience, this is more common in biopsies from tick bites than arachnid bites ( Figs 15.33–15.35 ).
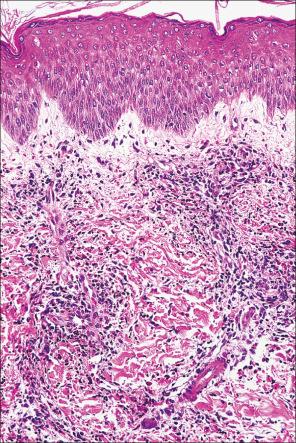
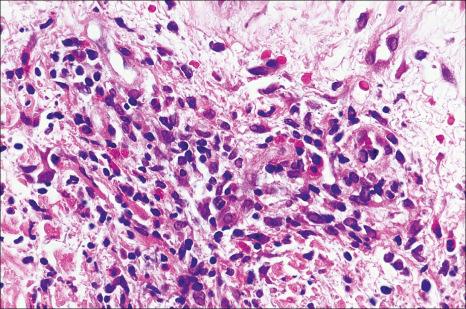
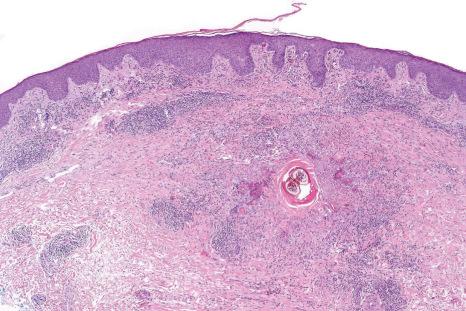
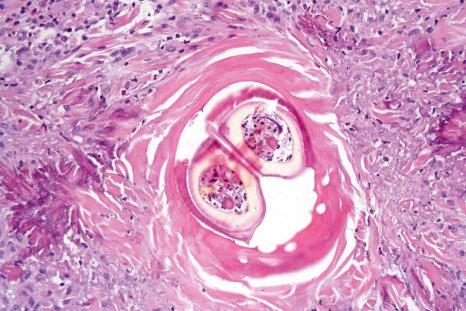
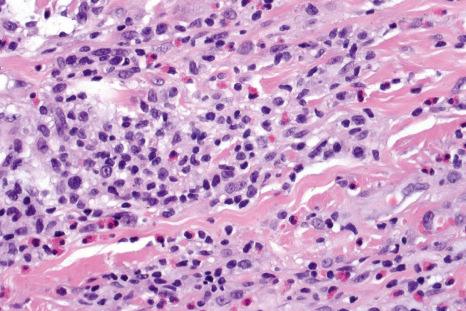
As with arthropod bite reactions, the histologic sequelae from arachnid bite are variable. Compared with the former, arachnid bite reactions are typically associated with more extensive necrosis and suppurative inflammation. Necrosis may extend to involve the subcutaneous fat and muscle. Variable numbers of eosinophils and lymphocytes are present, and marked dermal edema is often a feature. Secondary vasculitis, involving vessels within the lesion or in the immediate surrounding tissue, may be a feature in some cases. Injection of brown recluse spider venom into rabbits results in ‘mummified’ coagulation necrosis, a mixed inflammatory cell infiltrate, and vasculitis.
The histologic findings in biopsies of insect bites, short of identifying mouth parts in the specimen, are non-specific. The main differential diagnosis includes hypersensitivity reactions. The characteristic wedge shape of the infiltrate is an important clue to the diagnosis. Although scattered large atypical lymphocytes may be seen in bite reactions, these cells are more numerous and often arranged in aggregates in lymphomatoid papulosis. Bite reactions with a dense eosinophil-rich infiltrate may be indistinguishable from Wells syndrome. The occasional presence of flame figures heightens the similarity. Clinical correlation may be necessary to distinguish these two conditions.
The histologic findings associated with arachnid bite are also non-specific. Arachnid bites must be distinguished from pyoderma gangrenosum, factitial disease, primary vasculitis, and infections including cellulitis and necrotizing fasciitis. Arachnid envenomation appears to be overreported; thus, some cases have been reported in regions where the spiders have never been documented to exist. ELISA-based assays may be helpful to confirm the diagnosis. Without definitive evidence of involvement of an arachnid, the diagnosis must be considered one of exclusion so as not to overlook important clinical alternatives with a different treatment approach.
Seabather's eruption, sometimes referred to as ‘sea lice’, is attributed to stings from larval forms of coelenterates, often the thimble jellyfish ( Linuche unguiculata scyphomedusae ). Typically, patients develop a papular eruption in areas covered by the bathing suit, often accentuated where the suit is tight fitting, such as the waistline. The eruption is usually pruritic and may cause a burning sensation. Patients sometimes experience systemic symptoms such as malaise, fever, nausea, diarrhea, and vomiting.
Reactions to coelenterates such as jellyfish vary from minor irritation to fatal reactions following stings by highly venomous species such as the ‘box jellyfish’ ( Chironex fleckeri and Chiropsalmus quadrigatus ). Jellyfish stings are often erythematous and show a ‘whiplash-like’ appearance. Certain species may have more serious consequences, such as the Portuguese man-of-war ( Physalia physalis ), where systemic effects from neurotoxins can be seen, including cramping of muscles, respiratory distress, profound hypotension, and even death in extreme cases. It appears that the length of the nematocyst tube may correlate whether a jellyfish has the ability to sting; jellyfish with longer nematocysts can result in stings while those with shorter ones do not.
A topically applied envenomation inhibitor based on the mucous coat of clown fish is effective in dramatically reducing both some coelenterate stings and seabather's eruption, although it may lack efficacy against certain coelenterate species.
Biopsy of papules of seabather's eruption shows a non-specific perivascular inflammatory cell infiltrate composed of variable numbers of lymphocytes, eosinophils, and neutrophils. Epidermal changes are apparently not usually a feature.
Only few authors have reported the histologic findings following reaction to coelenterate stings. Non-specific perivascular inflammation with lymphocytes and variable numbers of eosinophils appear to be characteristic. Some cases show dense, sheetlike aggregates of lymphocytes, and histiocytes. Variable dermal edema may be an additional feature. Spongiosis and vesicle formation are also sometimes described. One fatal case showed only vascular congestion without significant inflammation, a histologic picture that likely reflects the fact that the patient died only 40 minutes after being stung. Only occasionally are nematocyst capsules and tubes identified.
The histologic differential diagnosis of reactions to coelenterates includes other hypersensitivity reactions. Short of finding nematocysts, the diagnosis depends entirely on clinical correlation.
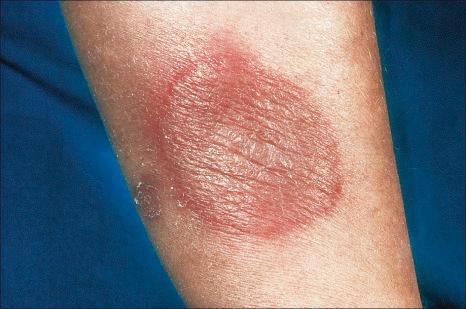
Once a common disease, it was thought that, with the effective antibiotic treatment of the causative infection, rheumatic fever would become of historical interest only. However, there has been a resurgence of the condition over the past few decades, particularly in developing countries.
Rheumatic fever is an immunologically mediated disease that follows an infection with Lancefield group A beta-hemolytic streptococcus. The infection causes pharyngitis and carditis. Additional features include polyarthritis, a neurological movement disorder known as Sydenham chorea, and subcutaneous nodules. Carditis, characterized by a valvular disease, is a major cause of morbidity and mortality.
Erythema marginatum rheumaticum is the designation given to the distinctive annular or polycyclic eruption of rheumatic fever. The lesions are nonpruritic, multiple, flat, erythematous maculopapules which change and spread over hours, and are often recurrent. The trunk and proximal extremities are most frequently affected. The hands and face may also be involved. By definition, erythema marginatum rheumaticum is associated with rheumatic fever, but occurs in only 1–18% of patients. Some studies have failed to identify significant HLA associations. However, there are conflicting reports of certain HLA subtypes and the disease.
The pathogenesis of rheumatic fever is incompletely understood. It appears likely that it results from a hypersensitivity reaction triggered by streptococcal infection. Specifically, patients develop autoantibodies that cross-react with streptococcal antigens due to molecular mimicry. For example, autoantibodies cross-react with cardiac muscle, causing carditis. Mice immunized with the streptococcal M protein develop myocarditis. Bradykinin in dense deposits can be seen in stromal and endothelial tissues, suggesting it may mediate some facets of this condition.
Variable numbers of neutrophils (sometimes associated with leukocytoclasis) and mononuclear cells are present in the infiltrate. Importantly, however, there is no evidence of vasculitis. Dermal papillary neutrophil microabscesses have occasionally been described.
It has been reported that rare cases are devoid of neutrophils and the infiltrate is instead composed of lymphocytes and histiocytes.
The biopsy findings in erythema marginatum are non-specific. Similar histologic features may be seen in patients with Still disease and acute lupus erythematosus. Careful search for vascular damage is necessary to exclude leukocytoclastic vasculitis. Special stains and culture to rule out an infectious etiology are sometimes required. Urticaria can demonstrate perivascular neutrophils, but additionally it shows significant dermal edema, and an interstitial inflammatory cell infiltrate, including neutrophils, eosinophils, and lymphocytes
Juvenile rheumatoid arthritis or systemic juvenile idiopathic arthritis (Still disease) is a heterogeneous group of disorders which share in common an inflammatory arthritis with many features similar to rheumatoid arthritis in adults. Juvenile rheumatoid arthritis patients, however, are seronegative for rheumatoid factor. There are marked differences in prevalence from region to region. Whites in Europe, the United States, and Australia (4 per 1000) have the highest prevalence. One study has suggested that the incidence of the disease is decreasing. This same study also documented incidence peaks indicating a possible cyclical pattern. Other studies have found seasonal variation in certain regions such as the Canadian prairies. However, such seasonal onset has not been apparent in other areas of Canada, in Denmark, or in Japan.
Juvenile rheumatoid arthritis is classified into three variants: pauciarticular, polyarticular, and systemic onset.
The pauciarticular (oligoarticular) form is characterized by arthritis involving up to a maximum of four joints. Systemic manifestations are uncommon. Uveitis, however, is frequently present.
The polyarticular form is manifest by symmetrical arthritis typically involving the knees, wrists, and ankles. Fever and hepatosplenomegaly are sometimes present.
The systemic-onset form is a severe variant in which lymphadenopathy, fever, and rash precede development of polyarteritis, which most often affects the knees, ankles, and wrists. Additional features may include hepatosplenomegaly and effusions. In general, the term Still disease is restricted to this form of juvenile rheumatoid arthritis; however, some authors use it for any of the variants. The majority of patients with the systemic form have the characteristic rash in contrast to the pauci- and polyarticular variants in which only 20–40% are affected.
The rash of Still disease is typically evanescent, and is characterized by a faint erythematous (salmon-colored), sometimes pruritic, macular eruption involving the trunk, extremities, head, and neck. Often, there is an association between onset of rash and febrile episodes, particularly in the late afternoon or evening. The rash is typically present for only a short period, usually a matter of a few hours; however, some lesions persist for more than 24 hours. It characteristically reappears without regard for its former distribution. Macules are often only a few millimeters in size but frequently become confluent to form larger lesions. Central pallor is sometimes a feature of the latter. The eruption – which may persist for weeks to years – tends to localize to areas of mild trauma and pressure.
Laboratory abnormalities include elevated ESR and C-reactive protein. Serum immunoglobulins may also be raised. Patients often have leukocytosis and increased ferritin levels and may have anemia, and thrombocytosis. Occasional patients have rheumatoid factor, and some authors consider this to represent bona fide juvenile rheumatoid arthritis. Antinuclear antibodies are commonly found in patients with pauci- and polyarticular variants of the disease. In contrast, antinuclear antibody is usually not present in the systemic-onset form.
It is very difficult to predict the outcome of this disease in the individual patient. Approximately 50% of patients experience symptoms into adulthood. Progression of juvenile rheumatoid arthritis to SLE has been documented. Serious complications including uveitis, cardiac tamponade, portal vein thrombosis, liver failure, disseminated intravascular coagulation, parenchymal lung disease, and hemophagocytic syndrome have been documented.
Despite the name juvenile rheumatoid arthritis, Still disease is not limited to the pediatric population. Adult onset is well described in the literature ( Fig. 15.36 ). Patients with the adult form of the disease may develop persistent papules and plaques and hyperpigmentation. Lesions are mainly seen on the face, neck, trunk, and extensor surfaces of the extremities.
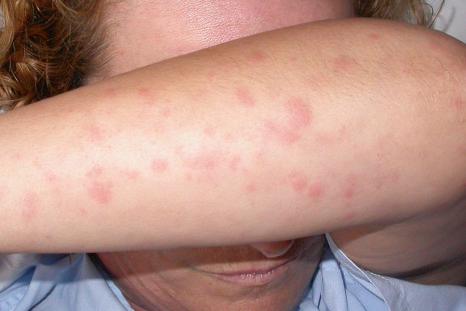
The pathogenesis of juvenile rheumatoid arthritis is poorly understood. It would seem likely, however, that the various subtypes have different etiologies. Thus:
IL-2 mRNA is detected more often in pauciarticular juvenile rheumatoid arthritis than in the polyarticular form.
A shift toward a Th1 type cytokine profile is seen with increased serum levels of IFN-γ, IL-6, IL-18, and TNF-α.
IL-18 may play a particularly crucial role in activating macrophages and inducing the TH1 cytokine profile in Still disease.
It has been suggested that nucleotide-binding and oligomerization domain (NOD)-like receptors (NLR) that detect microbes and help constitute the inflammasome (a complex of proteins which initiates an inflammatory reaction) may be involved in autoimmune disease generally and in Still disease in particular.
Data suggesting that the incidence of the disease is decreasing with cyclical peaks raise the possibility that environmental factors could play a role in the pathogenesis. Demonstration of T-cell oligoclonal expansions within synovial tissue suggests that an antigen or group of antigens may trigger the disease. The nature of such triggering factors, however, has not yet been identified.
The prevalence of autoimmune disease is increased in relatives of patients with juvenile rheumatoid arthritis compared with control subjects, suggesting that shared susceptibility genes may be of importance in the pathogenesis of juvenile rheumatoid arthritis and other autoimmune diseases.
The influence of various HLA alleles and their association with juvenile rheumatoid arthritis has been an area of considerable interest and has yielded a complex picture of the relationship between certain HLA alleles and risk of disease. HLA-A2, DR8, DR5, and DPB1*0201 are associated with increased risk of pauciarticular disease early in life. While B27 and DR4 may be protective in the early years, these alleles seem to confer increased risk of disease later in life.
CD4-reactive T lymphocytes are the predominant cell type in the inflamed synovium. As with other autoimmune disorders, production of predominantly Th1 cytokines (IFN-γ and IFN-β) has been observed in the synovium of juvenile rheumatoid arthritis patients.
The biopsy findings are non-specific and variable. There is often a perivascular neutrophilic infiltrate. In some cases, mononuclear cells are the predominant cell type, and in others there is a mixed infiltrate of neutrophils and mononuclear cells. A neutrophilic panniculitis may be associated with the disease. In adult-onset Still disease, distinctive histologic features have been described particularly in the persistent papules and plaques sometimes seen in the disease. The epidermis displays dyskeratotic keratinocytes in single units or aggregates ( Fig. 15.37 ). They tend to be present mainly in the upper layers of the epidermis and even in the stratum corneum. Other changes include subcorneal pustules, upper dermal lymphocytes and neutrophils, interface change, neutrophilic eccrine hidradenitis, and increased dermal mucin.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here