Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Surgery for spasticity should aim only to suppress the excess of tone in the muscular groups with harmful components of the disorder.
By reequilibrating the balance between agonist and antagonist muscles, surgery may reveal some voluntary motricity if preoperatively hidden behind hypertonia.
If botulinum toxin injections are insufficient, peripheral neurotomy (PN) can be indicated when spasticity is limited to one or a few muscular groups. A block test may be helpful to make a decision.
For spastic diplegic or quadriplegic children with cerebral palsy, dorsal rhizotomy is indicated before contractures and joint deformities appear and become irreducible.
Intraoperative mapping/monitoring is of paramount importance to achieve selective and tailored surgery.
In adult paraplegic patients who are severely affected at the point of being bedridden, microsurgical DREZotomy (MDT) can be an alternative to intrathecal baclofen (ITB).
If botulinum toxin injections are insufficient in hemiplegic patients, PN in the lower limb (especially for spastic foot) and/or upper limb (for spastic triple flexion) may be indicated.
MDT can be proposed when the entire upper limb is affected, especially when there is associated focal dystonia.
Functional neurosurgery for spasticity should be decided within the frame of a multidisciplinary team. Furthermore, regardless of the type of surgery performed, an adapted and tailored rehabilitation program is crucial.
Spasticity is defined as a velocity-dependent resistance to passive movement of a joint and its associated musculature. Spasticity is characterized by hyperexcitability of the stretch reflex related to loss of inhibitory influences from the descending supraspinal structures. Spasticity should not be treated just because it is present as it may serve to compensate for loss of motor power. Spasticity should be treated only when excessive tone leads to functional disability and impaired locomotion or to contractures and deformities. Neurosurgical interventions should be considered when the harmful spasticity cannot be controlled by physical therapy and medical treatment.
Management of spasticity includes not only intrathecal baclofen (ITB) therapy and botulinum toxin injections but also lesioning surgery directed at peripheral nerves, dorsal roots, the dorsal root entry zone (DREZ) and the spinal cord. Methods of surgical management are classified according to whether their impact is general or focal and whether the effects are reversible or permanent ( Fig. 126.1 ).
Lesioning procedures must be performed so excessive tone is reduced without suppressing useful muscular tone or impairing any residual motor/sensory functions. In patients who retain some masked voluntary motility, the aim is to re-equilibrate the balance between paretic agonist muscles and spastic antagonist muscles so treatment results in improvement in or reappearance of voluntary motor function ( Fig. 126.2 ). In patients with poor preoperative residual function, the aim is limited to halt the evolution of orthopedic deformities, improve comfort, and make care easier.
Our department has treated more than 1200 patients with spasticity over the past 25 years. We believe that teams dealing with spasticity should have all of the technical modalities at hand. , ITB therapy, which is discussed in detail in Chapter 269 , is indicated primarily for paraplegic or tetraplegic adult patients with diffuse spasticity, especially of spinal or brainstem origin, although it can also be used to treat spasticity related to cerebral palsy in older children, especially when dystonia is associated with spasticity. , Lesioning operations are indicated for focal spasticity of the limbs when treatment with botulinum toxin injections proves insufficient. Peripheral neurotomy (PN) is justified when harmful spasticity affects one or a few muscular groups. When harmful spasticity affects the entire limb or in the setting of paraplegia/diplegia or hemiplegia, surgery directed at the dorsal roots (dorsal rhizotomy) or the DREZ (microsurgical DREZotomy [MDT]) may be the solution in selected cases. Complementary orthopedic operations are frequently needed in patients with associated irreducible contractures, tendon retractions, joint deformities, or any combination of these problems.
PN was introduced for the treatment of a spastic foot by Stoffel. Later, PN became more selective by using microsurgery and mapping via intraoperative electrical stimulation to better identify the function of the individual nerve fascicles ( Fig. 126.3 ). Neurotomy consists of partial sectioning of motor branche(s) or fascicle(s) corresponding to the muscles in which spasticity is considered excessive. It works by interrupting the segmental reflex arc in both its afferent and efferent limbs. Neurotomy must not include sensory nerve fibers because even partial sectioning of them could result in neuropathic pain. Motor branches must be clearly isolated from the nerve trunk; the constituting fascicles must be dissected and identified to be stimulated independently ( ![]() ). On an empirical basis, it is agreed that neurotomy must include sectioning of approximately 50% to 80% of all branches to a targeted muscle for it to be effective.
). On an empirical basis, it is agreed that neurotomy must include sectioning of approximately 50% to 80% of all branches to a targeted muscle for it to be effective.
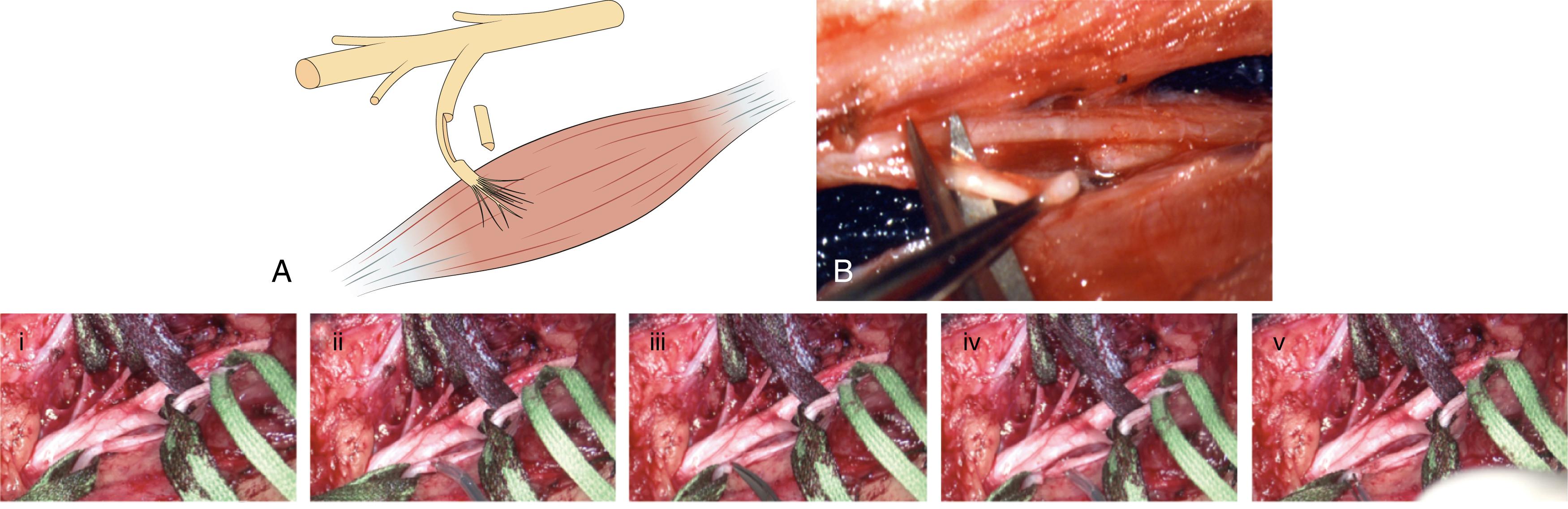
Before recommending PN, local blockade with a long-lasting anesthetic (2 to 3 hours with bupivacaine or ropivacaine) can be performed to evaluate the strength of the antagonist muscles and to determine whether the articular limitation results from spasticity or musculotendinous contractures/articular ankylosis. Botulinum toxin injections can also be used as a “prolonged” test for several months. This strategy, which aims at mimicking the effect of a neurotomy, allows patients to appreciate the benefit that could follow the neurotomy. In the lower limb, surgery can improve limb walking. In the upper limb, surgery can help patients achieve cosmetic benefit, allow patients to put hand in the pocket, provide functional improvement, or allow caregivers to wash the palms of the patient’s hands.
General anesthesia must be induced without long-lasting muscle relaxants so the motor evoked responses to electrical stimulation used to identify nerve fascicles can be detected. Nitrogen monoxide and propofol are also contraindicated because they modify reflex excitability.
Use of an operating microscope is required for accurate identification of the motor fascicles, which is essential for performing an effective neurotomy and avoiding sensory impairment. Stimulation is performed at a frequency of 2 Hz with low intensity (1-mA current). Bipolar stimulation (or tripolar, composed of an anode between two cathodes) should be used to limit electrical diffusion and therefore incorrect interpretation. The response to stimulation is visualized in the form of clinically observable movements of the corresponding muscles and, if considered useful, electromyography (EMG) recordings.
Once all motor branches (or their constituting fascicles) have been identified, those considered corresponding to harmful spasticity are sectioned in variable proportions (50% to 80%), depending on the degree of spasticity. A resection can be performed over approximately 5 mm; the proximal stump is then coagulated with fine bipolar forceps to prevent regrowth of fibers. The effect of each nerve interruption is then evaluated by comparing the muscle responses to electrical stimulation distal and then proximal to the resected portion. If the response after proximal stimulation is still intense, further resection is performed.
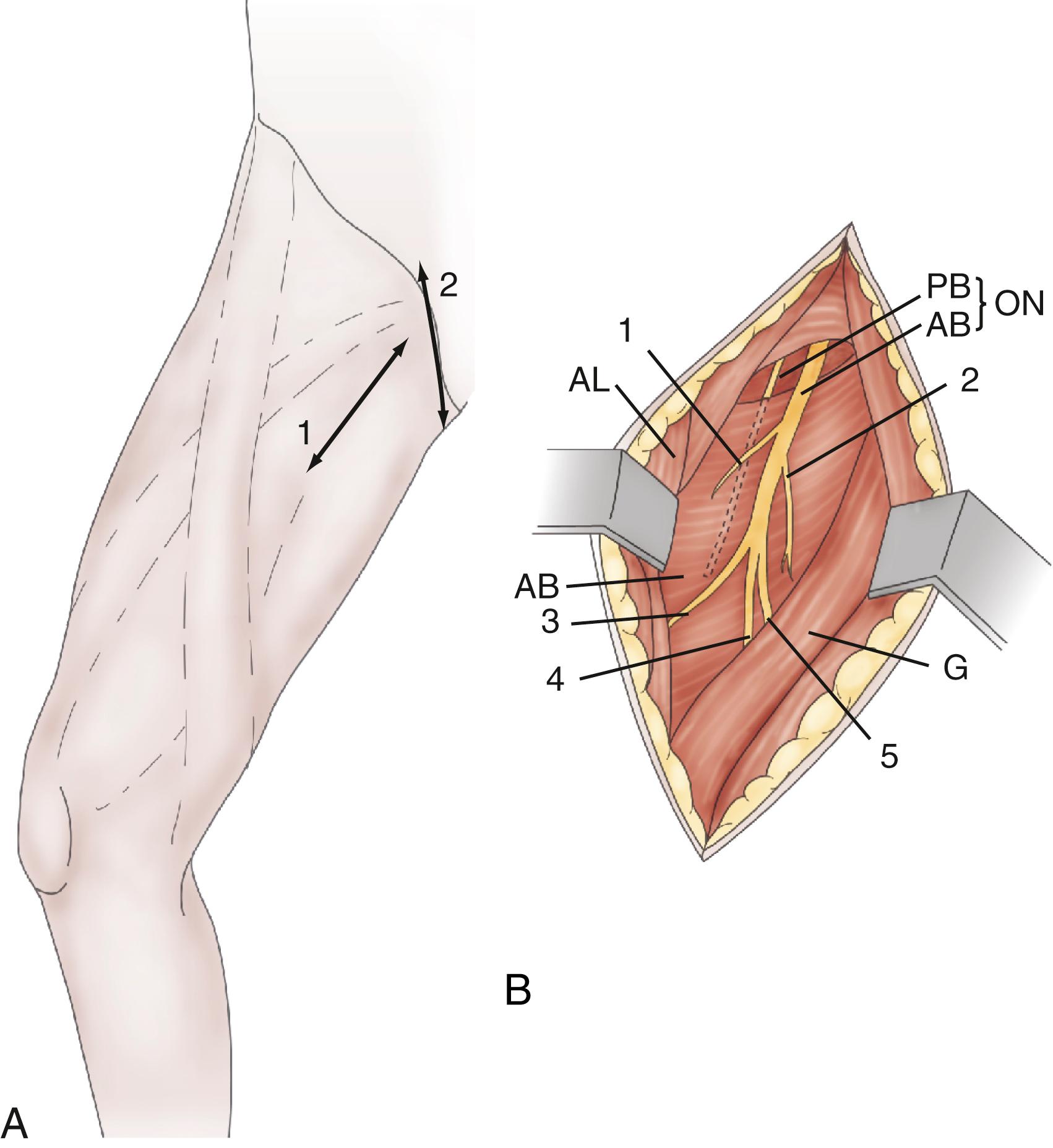
Obturator neurotomy ( Fig. 126.4 ) is for spasticity in the adductor muscles. It is often proposed for diplegic children with cerebral palsy when crossing or “scissoring” of the lower limbs hampers positioning or walking. It can also be performed on paraplegic patients to facilitate perineal washing, toileting, and self-catheterization. The dissection is conducted along the adductor longus muscle and should target the anterior branch of the obturator nerve. Its posterior branch, which is situated more deeply, should be spared to preserve the hip-stabilizing muscles.
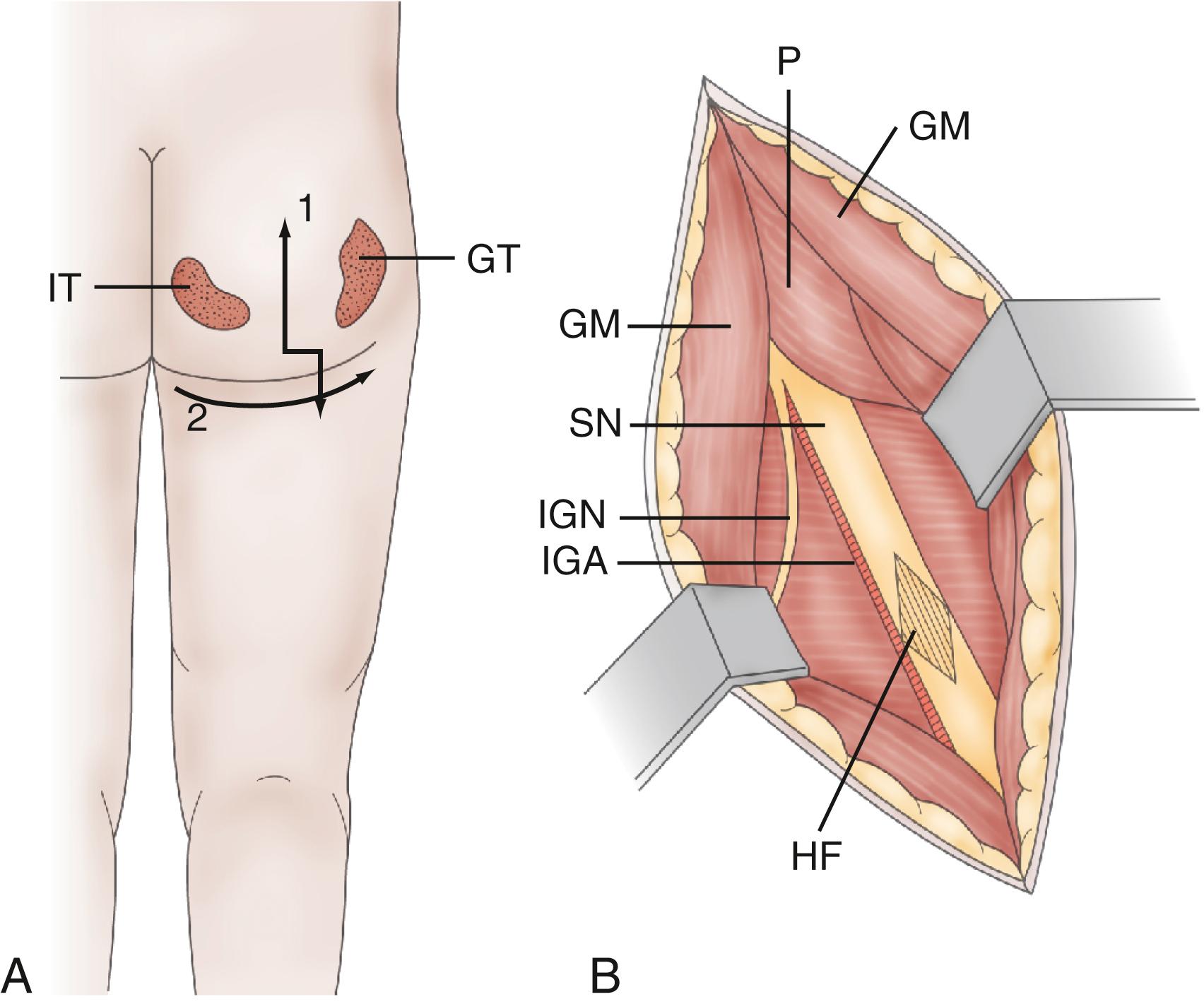
Hamstring neurotomy ( Fig. 126.5 ) is indicated to counterflex deformity of the knees. Branches to the hamstring muscles are isolated at the medial border of the sciatic nerve, primarily based on evoked responses to the semitendinosus muscle, which is the major muscle responsible for spasticity.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here