Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Head injuries in sports are comparatively mild compared with those in high-velocity motor vehicle accidents (MVAs), yet they remain significant and important injuries for team physicians to evaluate and manage.
Concussion is the most common head injury in sports. Information is evolving regarding pathophysiology, diagnosis, natural history, and treatment of concussion in sports.
Consider focal, vascular, and associated injuries (e.g., cervical spine, skull fractures, intracranial hemorrhage) when evaluating head-injured athletes.
Cumulative injury, persisting symptoms after concussion, and other sequelae of head injury may contribute to significant morbidity.
Head injuries occur across a large spectrum, from minor to catastrophic. Classifications such as diffuse versus focal or nonstructural versus structural are not absolute, but they permit the organized discussion of specific pathologies.
Involves diffuse axonal disruption in the white matter of the brain and brainstem
Severity of injury determined by clinical course
Mild DAI: comatose for 6–24 hours; mortality rate is approximately 15%
Moderate DAI: comatose for more than 24 hours; often associated with basilar fracture; mortality rate is approximately 25%
Severe DAI: prolonged coma, severe disability, or persistent vegetative state common if patient survives; high mortality rate.
Caused by shear or tensile forces; often results from falls or MVAs
Presentation: All patients present in coma, may exhibit decorticate or decerebrate posturing, severe posttraumatic amnesia, and cognitive deficits after awakening (moderate DAI). Can include hypertension and hyperpyrexia, increased intracranial pressure (ICP), and herniation syndromes.
Treatment: Supportive during coma; medical or surgical measures as needed for increased ICP and associated injuries.
The Fifth International Conference on Concussion in Sport (CIS) defined sports-related concussion (SRC) as a “subset of traumatic brain injury.”
It is a “complex pathophysiologic process affecting the brain, induced by traumatic biochemical forces.”
Several common features that incorporate clinical, pathologic, and biomechanical injury constructs that may be used in defining the nature of a concussive head injury include:
May be caused by direct impact to head or elsewhere on body with “impulsive” force transmitted to head.
Results in the rapid onset of short-lived impairment of neurologic function that usually resolves spontaneously, though symptoms may arise over minutes to hours.
May result in neuropathologic changes, but acute clinical symptoms reflect functional rather than structural disturbance.
Results in a graded set of clinical syndromes that may or may not involve loss of consciousness. The resolution of symptoms typically follows a sequential course, but in some cases may be prolonged.
The clinical signs and symptoms cannot be explained by drug, alcohol, or medication use; other injuries (such as cervical injuries, peripheral vestibular dysfunction); or other comorbidities (e.g., psychological factors or coexisting medical conditions).
Typically associated with grossly normal structural neuroimaging studies
Advanced neuroimaging (e.g., diffuse tensor imaging, functional magnetic resonance imaging (MRI), magnetic resonance spectroscopy) may demonstrate abnormalities; however, imaging will remain normal in many clinical cases.
Advanced imaging currently remains a research tool.
SRC is the most common head injury in athletes; in the majority of cases resolves completely (within 2 weeks in adults and 4 weeks in adolescents and children).
In the sports tracked by the National Collegiate Athletics Association, the incidence of SRC is shown in Table 45.1 .
| Head Protection Required | % of All Game Injuries | No Head Protection | % of All Game Injuries |
|---|---|---|---|
| Men’s ice hockey a | 7.9 | Women’s lacrosse a | 6.3 |
| Women’s ice hockey | 18.3 | Wrestling | 3.3 |
| Men’s lacrosse a | 5.6 | Women’s soccer | 5.3 |
| Football a | 6.0 | Men’s soccer | 3.9 |
| Spring football a (practice) | 5.6 | Field hockey | 3.9 |
| Softball | 4.3 | Women’s basketball | 4.7 |
| Baseball | 2.5 | Men’s basketball | 3.2 |
| Concussion Injuries in Games and Practices Per 1000 Athlete Exposures | |||
| Head Protection Required | No Head Protection | ||
| Football a | 0.37 | Wrestling | 0.25 |
| Men’s ice hockey a | 0.41 | Men’s soccer | 0.28 |
| Women’s ice hockey | 0.91 | Women’s soccer | 0.41 |
| Men’s lacrosse a | 0.26 | Women’s lacrosse a | 0.25 |
| Spring football a | 0.54 | Field hockey | 0.18 |
| Softball | 0.14 | Women’s basketball | 0.22 |
| Baseball | 0.07 | Men’s basketball | 0.16 |
Caused by acceleration/deceleration (tensile), rotational (shearing), and/or impact (compressive) forces. Coup injuries often result from direct impact, whereas contrecoup injuries occur from acceleration/deceleration forces (e.g., athlete falls and strikes ground with head).
Presentation: The hallmark of concussion is confusion; other signs and symptoms may occur immediately or several minutes later. In some situations, they may be delayed ( Table 45.2 ).
| Early (Minutes to Hours) | Late (Days to Weeks) |
|---|---|
|
|
Treatment: initial period of rest (physical and cognitive), education, protection from further injury, and serial follow-up evaluations (see detailed discussion later)
SRC is associated with neurochemical and metabolic changes with changes in glutamate, potassium, lactate, and glucose, in addition to changes in cerebral blood flow.
Force on the brain may cause stretching of neuronal cell membranes and axons, resulting in a complex cascade of ionic, metabolic, and pathophysiologic events.
There are no current objective biomarkers, neuroanatomic or neurophysiologic, that can be used practically and reliably to determine if an athlete has a concussion, though several options are actively being researched. See the “Additional Diagnostic Testing” section. After concussion, the brain cells may be in state of injury-induced vulnerability; a second injury during this time of heightened vulnerability may produce additional deficits.
Injury-induced vulnerability is characterized by a fuel need–fuel delivery mismatch. The brain’s need for glucose increases acutely (hyperglycolysis), and cerebral blood flow and oxidative metabolism are relatively reduced.
Increased levels of extracellular potassium probably activate adenosine triphosphate (ATP)–dependent sodium–potassium pumps, which increases energy consumption and adds to metabolic stress (e.g., need for glucose).
Glutamate (excitatory amino acid) levels increase extracellularly and may contribute to an increased flux of potassium.
Increased intracellular calcium may be related to regional reduction of cerebral blood flow.
Low-pressure venous bleed into potential space (subdural) between the arachnoid and dura mater; classified by time to clinical presentation ( Fig. 45.1 ).
Acute: within 24 hours; often associated with other intracranial pathology (e.g., contusion, axonal injury)
Subacute: 24 hours to 2 weeks
Chronic: 2 weeks or more
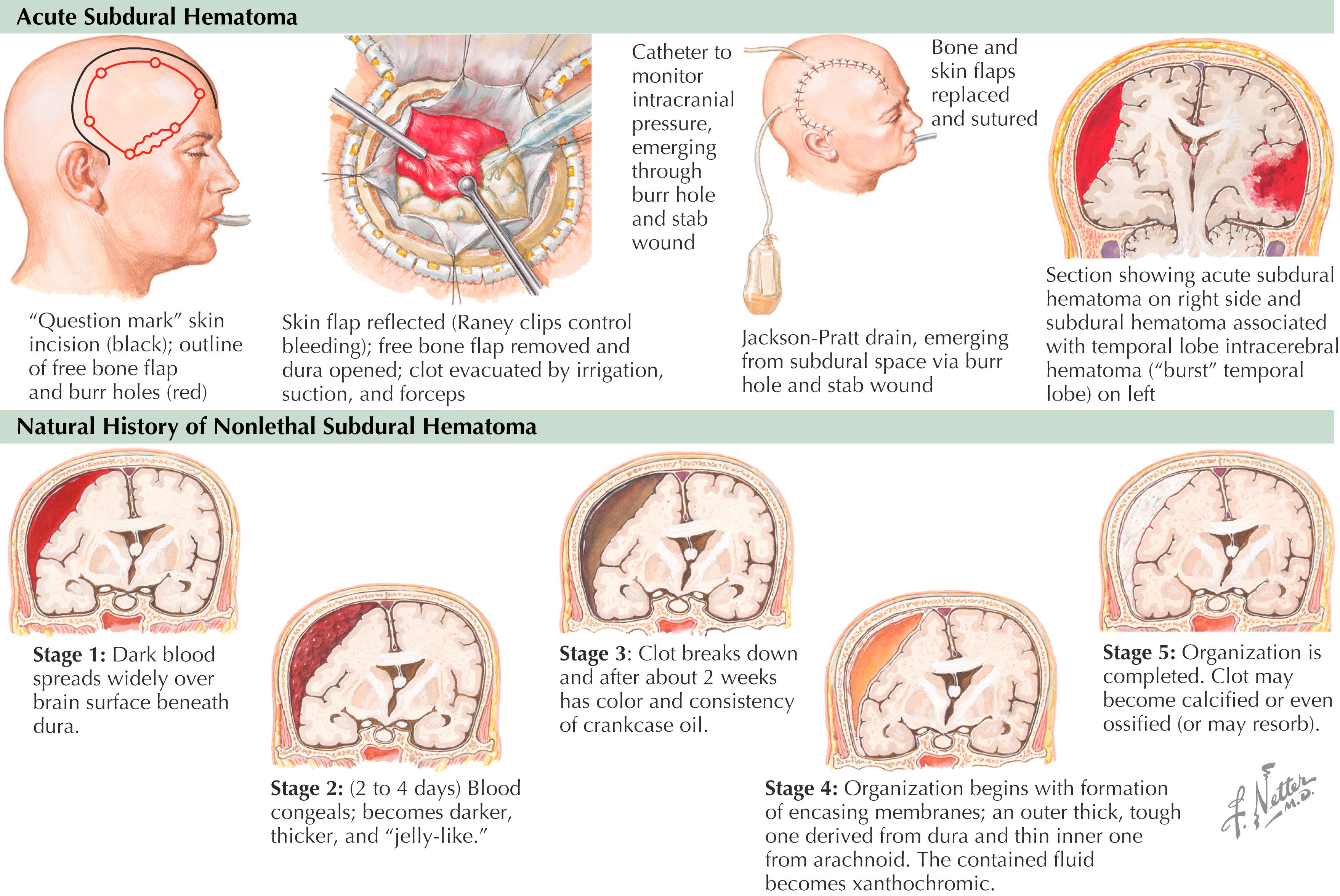
Leading cause of death related to head injury; overall mortality rate of 35%–50%; loss of consciousness implies poor prognosis.
Elderly and alcoholics at greatest risk because of increased space between brain (atrophy) and dura.
Caused by brain movement within the skull: acceleration–deceleration, rotational, shearing injuries.
Presentation: Decreased/altered level of consciousness, lucid interval followed by declining mental status and headache; patients may have pupil inequality, motor deficit (e.g., unilateral weakness or paralysis), or other indicators of brain swelling.
Treatment: Usually prompt surgical evacuation (see Fig. 45.1 ).
Surgery within 2–4 hours after onset of neurologic deterioration is associated with a lower mortality.
Craniotomy may be associated with better outcomes than burr hole evacuation.
Nonoperative management may be an option for patients with small hematoma (<10 mm and <5 mm of midline shift on head computed tomography [CT]).
Patient may be observed if prognosis is poor (e.g., prolonged loss of consciousness) or if elderly and asymptomatic.
High-pressure arterial bleed between inner table of skull and dura mater (epidural space); middle or other meningeal arteries often disrupted; 80% associated with a skull fracture in the temporoparietal region; occasionally caused by tear of underlying dural sinus (most common in posterior fossa) ( Fig. 45.2 ). Mortality rate is low if diagnosed acutely; comatose state is associated with the highest mortality rate (<20%); mortality rate higher with associated injuries.
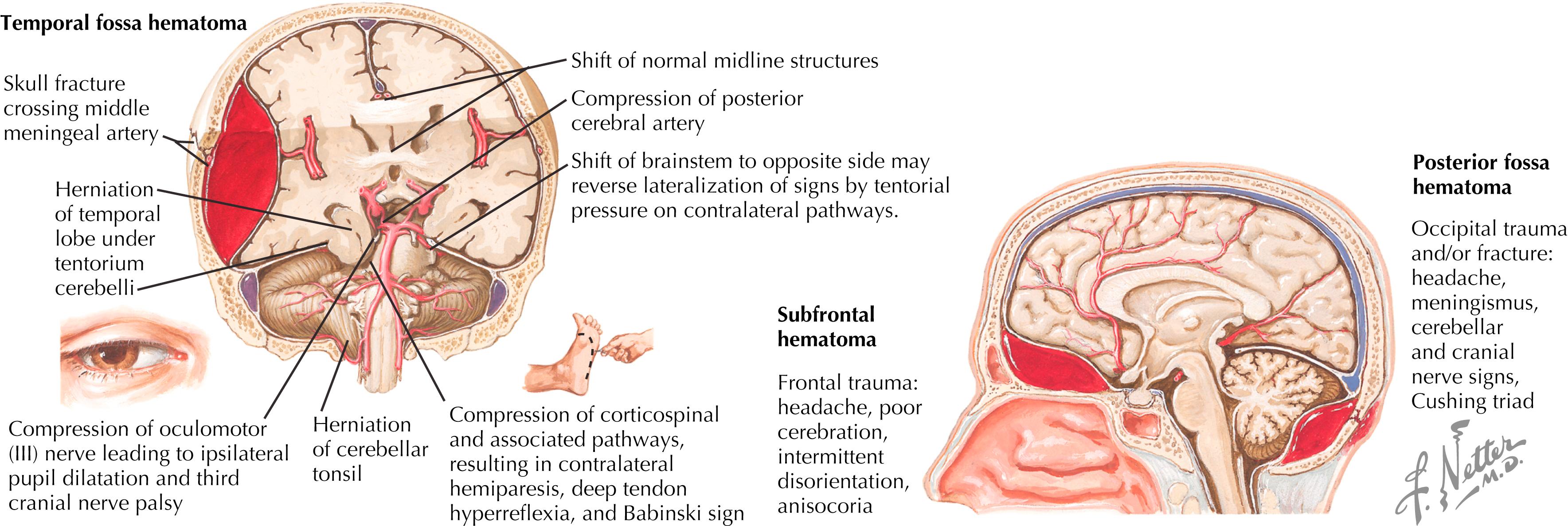
Presentation: Decreased level of consciousness followed by lucid interval, deteriorating mental status with eventual loss of consciousness, headache, confusion, sleepiness, nausea, vomiting.
Late signs: Ipsilateral dilated pupil, contralateral muscle weakness, coma
Lucid interval may last for several hours and lead to false reassurance and a missed diagnosis.
Treatment: Surgical evacuation of hematoma.
Craniotomy may be preferred over burr hole, as it allows for more complete evacuation.
Bleeding from small-caliber arterioles within the brain parenchyma; frontal and temporal lobes are affected most often; may be accompanied by brain laceration ( Fig. 45.3 ). Caused by tensile or shearing forces that stretch the brain (coup or contrecoup mechanism of injury).
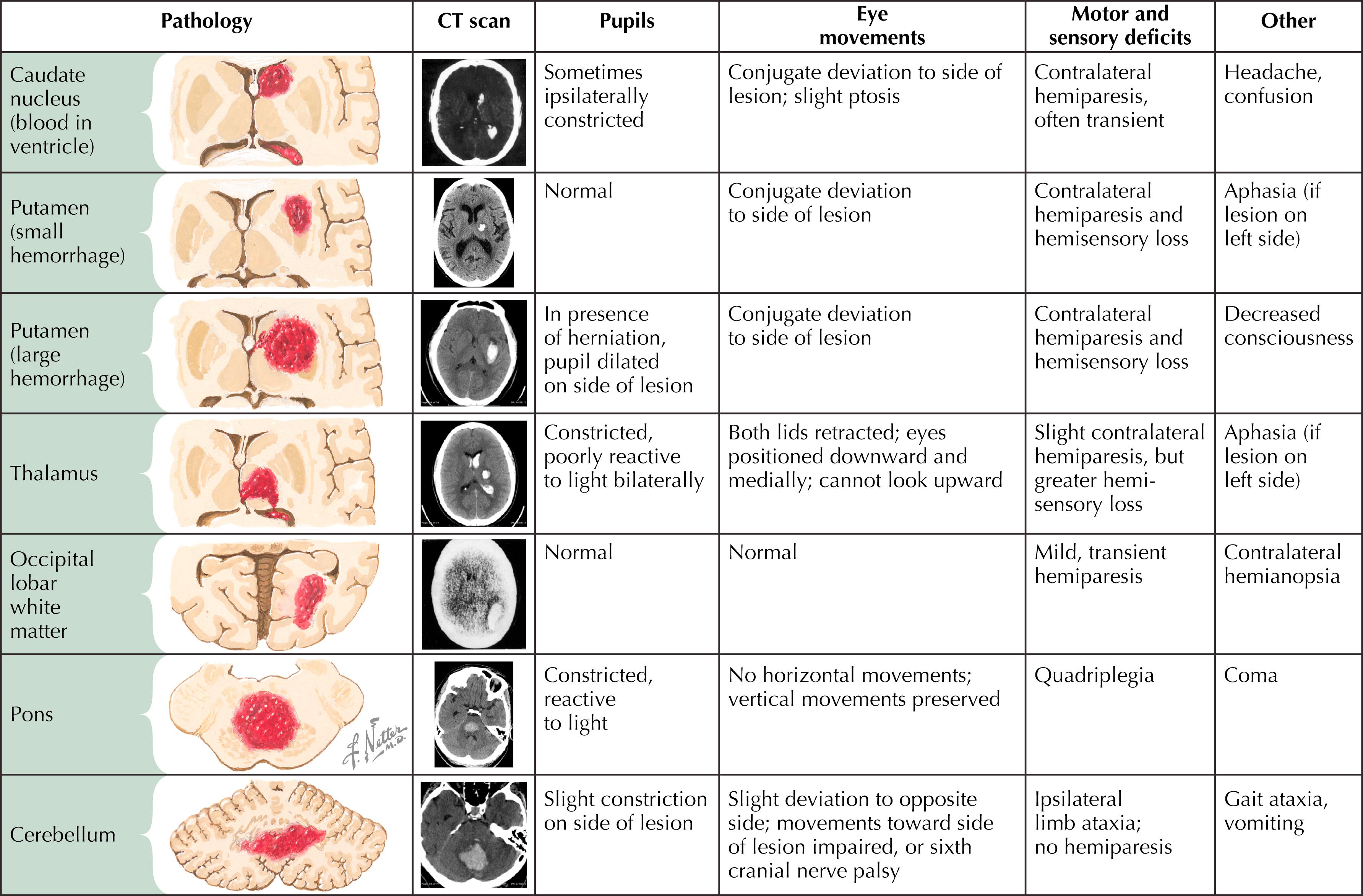
Presentation varies with the size and location of lesions, as well as any associated pathology (e.g., contusion, postinjury edema); loss of consciousness (<50%), headache, confusion, nausea, vomiting, focal deficits (affected areas) (see Fig. 45.3 ). Symptoms may develop over hours or days.
Treatment: Many require emergent intervention to lower ICP and/or stop bleeding; depends on severity of clinical presentation, bleed, and associated pathology
Bleeding between the arachnoid and pia mater (subarachnoid space) into the cerebrospinal fluid (CSF); may be traumatic or spontaneous.
Traumatic SAH results in small tears of subarachnoid vessels; spontaneous SAH (and sometimes traumatic SAH) is often associated with intracranial aneurysms and arteriovenous malformations, and sometimes with hypertension and arteriosclerosis ( Fig. 45.4 ).
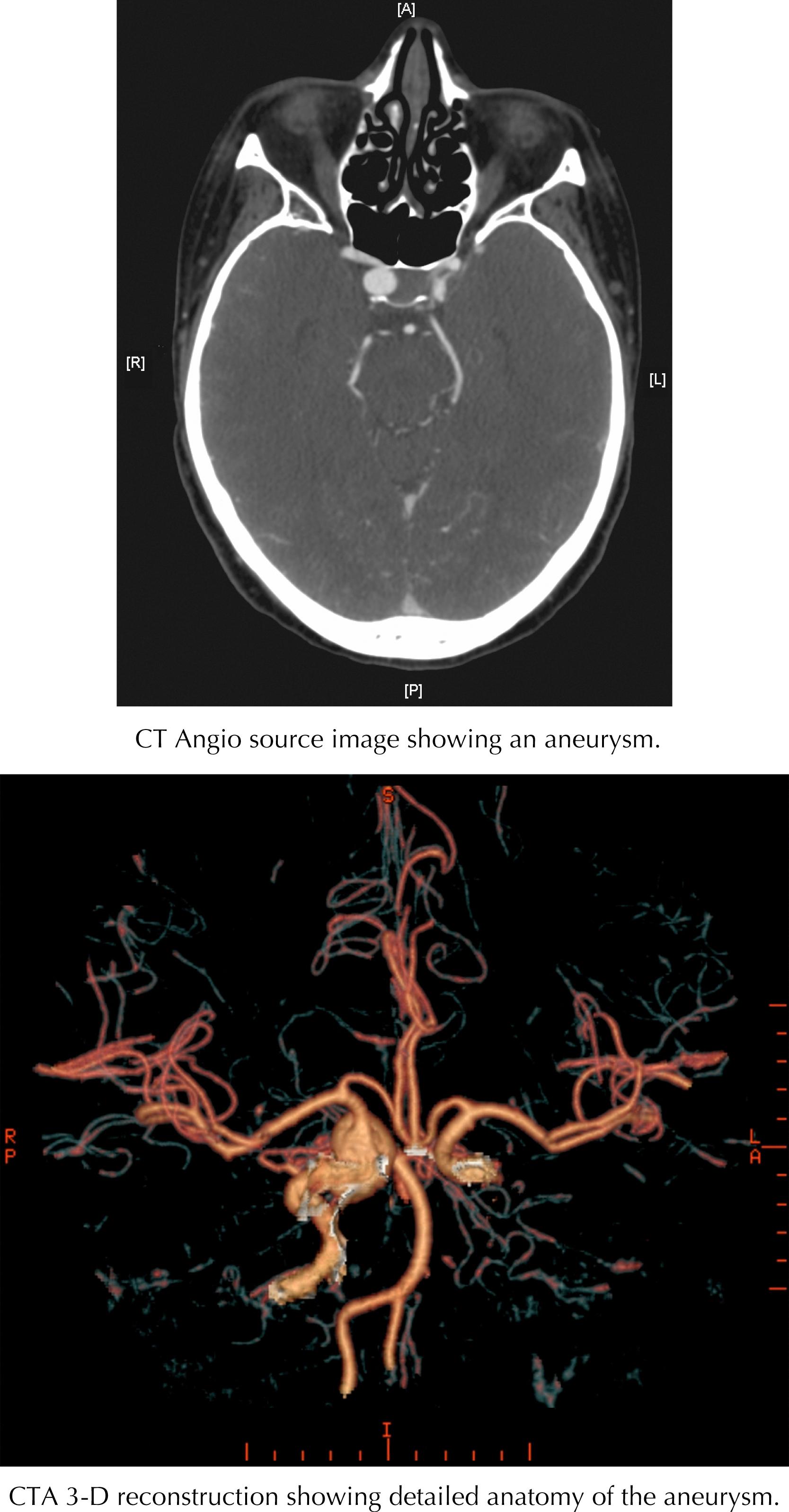
Presentation depends on associated pathology and whether SAH is traumatic or spontaneous. Symptoms include headache (often described as the “worst ever”), photophobia, nausea, vomiting, dizziness, confusion, neck stiffness, and focal deficits (affected areas).
Must be differentiated from a “bad” migraine or meningitis. Lumbar puncture done only after funduscopic examination (to rule out papilledema) and CT scan. Xanthochromia of the CSF may be the most specific finding with SAH.
Treatment varies with individual case and pathology; may involve surgical intervention (e.g., clipping of aneurysm), medical management (e.g., calcium channel blocker for vasospasm), and conservative measures.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here