Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Fortunately, most sports-related hand and wrist injuries, when addressed in a timely manner, do not represent a significant threat to limb viability, long-term function, or eventual return to sports.
Perhaps the greatest morbidity from these injuries results from delayed presentations or missed injuries, a common feature in athletes motivated to compete.
Hand function is closely linked to full flexion of the ulnar three digits (for power grip), prehension grip in the radial three digits (fine manipulation), and a stable, mobile wrist.
Do not minimize or underestimate subtle losses of finger flexion after open or closed potential injuries to the flexor mechanism. Delayed diagnosis and treatment of jersey fingers or flexor tendon disruption invites significant morbidity and limits treatment options.
Return to play (RTP) for hand injuries, as with other musculoskeletal conditions, will be influenced by level of participation (amateur vs. professional), sport/position, and tissue-specific healing requirements. As a general trend, we are apprehensive about power grip/contact sports (i.e., football/rugby) with K-wires in place, especially those crossing a joint.
Dictated by the context of the injury. No single, comprehensive evaluation applies to all maladies.
Attention is directed toward the individual part and system (bone, joint, tendon, nerve, etc.) in question.
Focal swelling, digital perfusion, digital malrotation, digital cascade, and any penetrating injury must be noted.
Any difference in posture of one digit relative to the others should not be dismissed or minimized, as this often signifies a displaced fracture, tendon disruption, or joint subluxation.
In the absence of a penetrating injury, isolated pallor of a digit usually represents spasm of the digital vessels. Although this often resolves with digital warming or reduction of associated displaced fractures or dislocations, digital viability remains in question until perfusion is actually observed.
Even in closed fractures, the digital vessels can tear or thrombose, representing a surgical emergency.
Dorsal swelling of the hand is a nonspecific finding and may not represent a significant injury.
Careful palpation of specific bones or ligaments in question is FUNDAMENTAL to hand/wrist assessment. There are not many “referred-pain” injuries in the hand or wrist—tenderness to palpation does not lie.
Focused palpation will usually localize the injured structure within an area of generalized edema demonstrating diffuse swelling; for example, a swollen wrist after distal radius fracture or perilunate injury.
Focal tenderness over the scaphoid or scapholunate ligament, even in the setting of normal radiographs, suggests an underlying ligament tear or fracture with poor prognosis if not recognized and treated.
Description: Any tear or disruption of the sterile or germinal matrix of the nail bed; may or may not be associated with an underlying distal phalanx fracture or actual disruption of the nail plate ( Fig. 51.1 ). Associated distal phalangeal fractures, particularly of the midshaft, may be open and require aggressive debridement/washout.
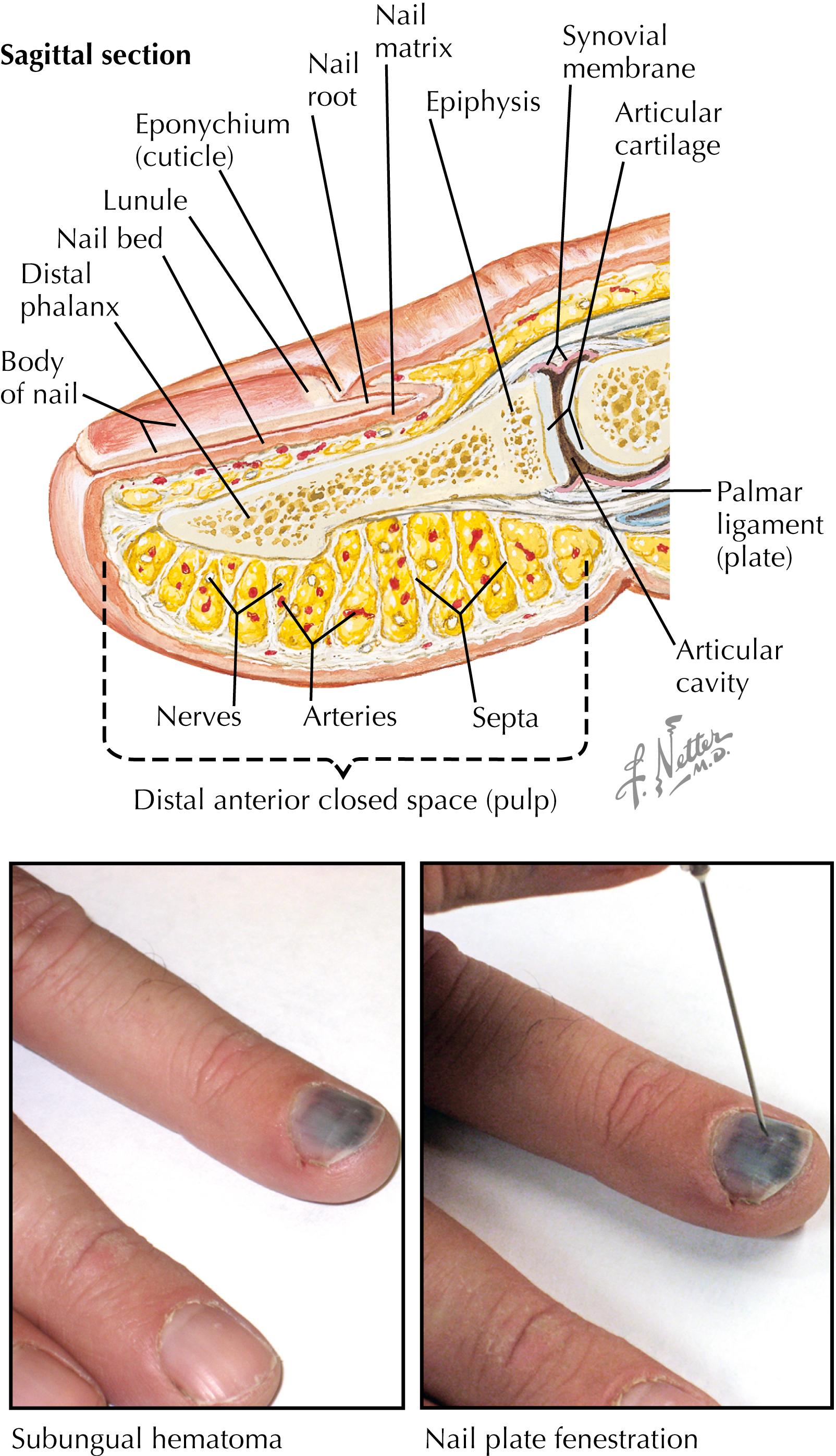
Mechanism of injury: Usually caused by dorsal crush of the fingertip (such as when the fingertip is crushed by another player’s cleated shoe); however, may also occur with axial load to the fingertip that results in flexion fracture of the distal phalangeal shaft and tear of the overlying nail bed.
Presentation: If the nail bed is disrupted, subungual hematoma results. The tear may extend peripherally beyond the borders of the nail fold into the surrounding skin (see Fig. 51.1 ).
Physical examination: Gross instability of the fingertip with nail bed injury is suggestive of a concomitant distal phalangeal shaft fracture.
Differential diagnosis: If the base of the nail plate is flipped out dorsally over the nail fold, consider an open fracture of the proximal portion of the phalanx. In skeletally immature patients, the presence of the physis at this location may result in failure to recognize what is, in fact, a Seymour (open Salter–Harris I distal phalangeal) fracture.
Diagnostics: Physical examination is usually sufficient. Anteroposterior (AP) and lateral radiographs reveal an underlying distal phalanx fracture.
Treatment: For a small subungual hematoma encompassing a portion of the nail plate, no intervention is necessary. Decompression of the hematoma through needle fenestration of the nail plate can offer pain relief; however, this may increase the likelihood of wound sepsis if performed on a playing field (see Fig. 51.1 ). For larger hematomas (50% of the nail plate) with tearing beyond the nail fold borders, formal repair is recommended. Under a digital block anesthetic and digital tourniquet the nail plate should be removed, the wound irrigated, and the nail matrix repaired with either a topical skin adhesive or a 7-0 resorbable suture. The adjacent skin rip is repaired with a 5-0 nylon suture. An underlying phalangeal tuft fracture is nonsurgically managed. However, an associated unstable distal phalangeal shaft fracture requires washout and pin stabilization, usually crossing the distal interphalangeal (DIP) joint.
Prognosis and RTP: If no nail bed repair is required, immediate RTP is alright. After nail bed repair, the fingertip (including DIP joint) should be dressed and splinted to protect from impact. If there is an associated unstable phalangeal shaft fracture requiring pin fixation, RTP should be delayed until pin removal in gripping sports. Prognosis for nail plate growth is directly related to anatomic restoration of the nail bed. If there is a wide scar in the matrix, a ridge or split in the nail plate will occur. Open fractures through the nail bed require urgent surgical debridement in the operating room. Displaced distal phalangeal shaft fractures are often unstable and require pinning.
Description: Loss of terminal extensor mechanism attachment to the distal phalanx with resultant flexion deformity of the DIP joint
Mechanism of injury: Sudden forced flexion of the DIP joint during active extension through the terminal tendon, often as a result of a ball jamming the fingertip ( Fig. 51.2 )
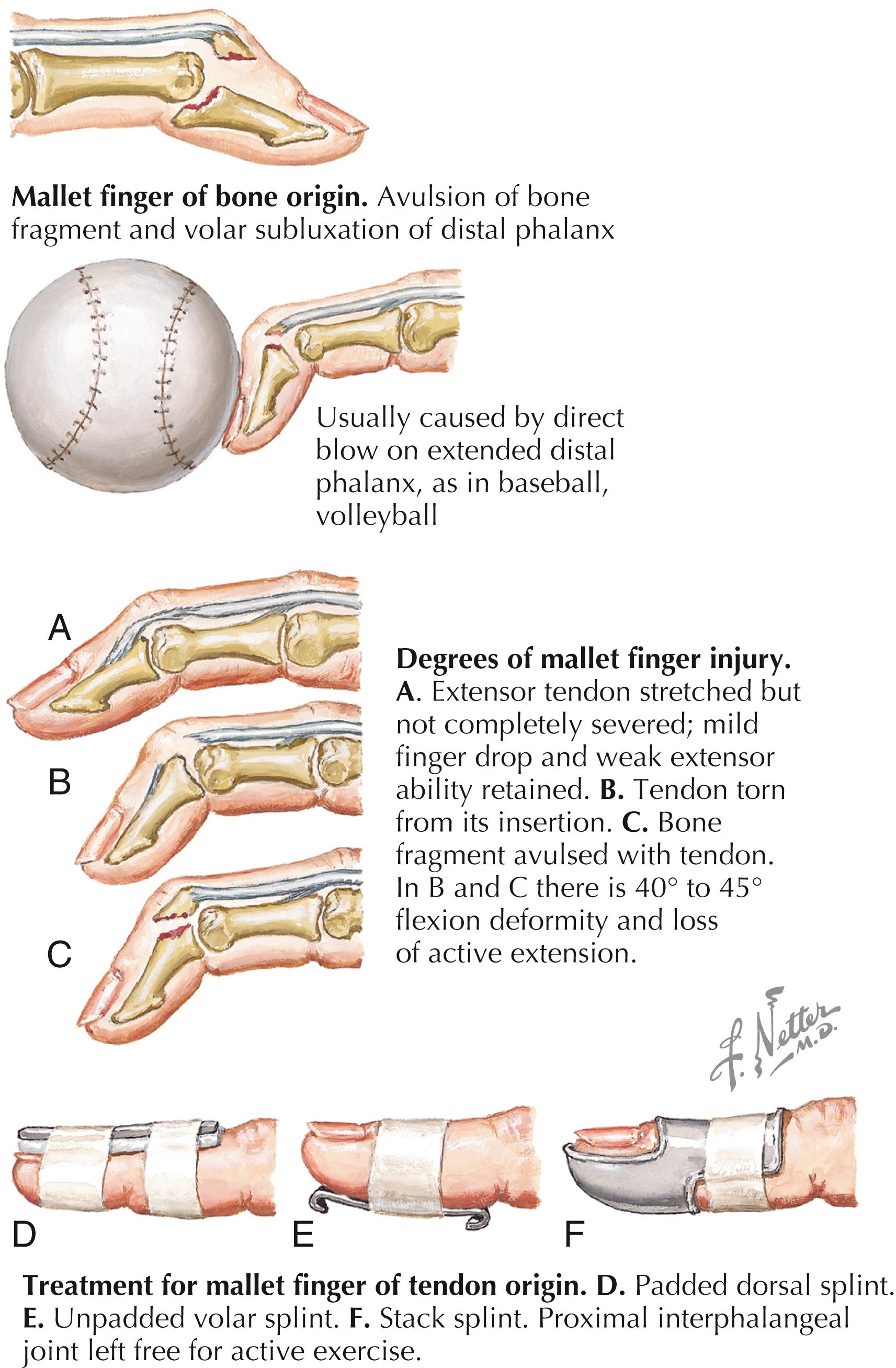
Presentation: The DIP joint is maintained in flexion with an inability to actively bring the joint into full extension. Varying degrees of pain, often with minimal or no pain; swelling or ecchymosis may be noted over the dorsal aspect of the joint.
Differential diagnosis: Distal phalanx fracture or DIP dislocation
Diagnostics: Posteroanterior (PA) and lateral radiographs of a digit to assess if injury is limited to the soft tissue (tendon only) or has associated bony avulsion (see Fig. 51.2 ). Lateral radiographs determine stability based on the size of the bony component and whether palmar subluxation is present.
Treatment: Acute mallet injuries with no subluxation on the lateral radiographs require full-time splinting of the DIP joint in extension for 6–8 weeks (see Fig. 51.2 ). Displaced bony components with joint involvement of >30% and/or palmar subluxation often require surgery to restore joint congruity. The DIP joint will usually require transarticular pinning in full extension with surgery. Primary surgical repair of acute, closed, soft tissue mallet injuries has not proven to be superior and may have more significant complications.
Prognosis and RTP: Noncompliance with splint wear will negatively affect the outcome and usually results in mild-to-moderate degrees of extension lag. The functional effect of this is variable. Most athletes nonsurgically treated will RTP within a week (while splinted). With surgical treatment, RTP will depend on the athlete’s ability to protect a transarticular pin. Any activity requiring grip is likely to result in bending or breakage of the pin.
Most patients will have some degree of extensor lag, even with full compliance, and should be advised of this. If lag is excessive and interferes with function, revision surgical options may be considered.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here